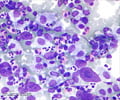
Treatment
Strict adherence to protocols, treatment without delays, dose reductions and avoiding certain drugs to prevent toxicities may be important for therapeutic progress in an adult with ALL.
Doctors look into various aspects while treating patients, such as their age or the subset of ALL before deciding on their treatment. The goal of ALL treatment is to cure the patient of the disease completely.
There is a high probability for children with ALL to be cured of the disease. Currently, at least 80% of childhood ALL are considered curable. In recent times, the numbers of adult patients whose diseases are in remission have also considerably increased.
The following are some of the treatment methods employed for treating ALL:
a) Chemotherapy
During chemotherapy, drugs are employed that completely destroy the leukemic cells or prevent them from proliferating. Chemotherapy treatment for ALL are carried out in three phases:
- Induction therapy
- Consolidation therapy
- Maintenance therapy
- Induction Therapy - This intense therapy, which lasts for nearly a month, aims to revive normalcy in a patient by bringing the disease to remission. Induction therapy brings about achieves remission in more number of children (95%) than in adults (75% - 89%). Depending on the treatment protocol, the next step may be consolidation chemotherapy or bone marrow transplantation.
Standard induction therapy typically involves the following drugs:
- Vincristine
- Prednisone
- Anthracycline
- Cyclophosphamide
- L-asparaginase
These drugs are administered over 4-6 weeks.
- Intrathecal Therapy - This chemotherapy is usually given twice during the first month of induction treatment and 4 to 6 times during the next 1-2 months period. It is then repeated less often during consolidation and maintenance. Drugs are introduced into the cerebrospinal fluid to destroy any leukemia cells that may have spread to the central nervous system.
Usually, methotrexate is delivered through spinal taps during intrathecal chemotherapy. Drugs like hydrocortisone (a steroid) and cytarabine (ara-C) may be added, particularly in the treatment of high-risk children.
However, most clinicians prescribe the following antibiotics for patients undergoing induction therapy. A commonly used regimen includes the following:
- Ciprofloxacin
- Fluconazole or itraconazole
- Acyclovir or Valtrex
If patients taking these antibiotics become febrile, they are switched to another antibiotics and these are administered intravenously.
Induction therapy requires the patient to be hospitalized.
Supportive care with growth factors such as granulocyte colony-stimulating factor (G-CSF) may also be provided.
- Consolidation therapy- The second phase of chemotherapy is also carried out in an acute and vigorous manner and lasts for about 4-8 months. If a patient is diagnosed with leukemia, about 100 billion leukemic cells will be present in the body. When 99.9% of these cells are eliminated the patient is reported to have entered remission.
However there are still about 100 million leukemic cells in the patient’s body. The role of this therapy is to bring down the numbers of these remaining cells. The dosage and duration of this therapy is determined by the patient’s risk/prognostic factors. Children with average-risk ALL are usually treated with the following drugs during consolidation therapy:
- Methotrexate
- 6-Mercaptopurine
- 6-Thioguanine
- Vincristine
- Prednisone
Children with high- risk leukemia are treated differently. They may receive extra drugs such as the following:
- L-asparaginase
- Doxorubicin (Adriamycin),
- Etoposide,
- Cyclophosphamide,
- Cytarabine
- Dexamethasone (substituted for prednisone)
In adults, methotrexate, anthracycline, podophyllotoxins and HD cytarabine are employed in consolidation therapy.
Consolidation therapy too requires hospitalization. The treatment protocols may differ for various people.
- Maintenance Therapy - This therapy is less intense than the other two and may last for 2-3 years. Once the patient enters remission it is important for the status to be maintained and this is done by maintenance therapy. Maintenance therapy is administered in an outpatient setting.
- Most treatment plans use the following drugs:
- Methotrexate
- 6-mercaptopurine pills, alongside vincristine, which is administered intravenously
- Steroids like prednisone / dexamethasone are given for short durations once in every 4 to 8 weeks.
- A drug, called imatinib (Gleevec), can kill leukemia cells that contain the Philadelphia chromosome.