- D C Dutta’s Textbook of Gynecology
- Garthwaite M, Harris N. Vesicovaginal fistulae. Indian J Urol. 2010 Apr-Jun; 26(2): 253–256. doi - (10.4103/0970-1591.65400)
- Stamatakos M, Sargedi C, Stasinou T, Kontzoglou K. Vesicovaginal Fistula: Diagnosis and Management. Indian J Surg. 2014 Apr; 76(2): 131–136 - (doi: 10.1007/s12262-012-0787-y)
- Vesico-vaginal fistula -- a major cause of unnecessary and avoidable suffering. Safe Mother. 1999; (27):1 - (doi: 10.1007/s12262-012-0787-y)
What is a Vesicovaginal Fistula?
A vesicovaginal fistula is an abnormal communication between the urinary bladder and the vagina in female patients that results in urine leaking out uncontrollably through the vagina (urinary incontinence). It commonly occurs in the developing countries due to complicated childbirth.
Successful management of the vesicovaginal fistula requires a quick and accurate diagnosis and timely repair as it causes devastating consequences and serious disability to the patient.
It poses not only physical but also psychological problems for the women as such patients are usually looked down upon or may be even abandoned by their husbands and society due to the smell and shame of urine leakage. For those who already have this condition, understanding, care and support of the husband and community is required to prevent the female from going into depression and restoring her to normal health.
What are the Causes of Vesicovaginal Fistula?
Vesicovaginal fistula usually occurs in underdeveloped countries which lack good obstetric care. Most cases of vesicovaginal fistula occur following childbirth. Causes of vesicovaginal fistula include the following:
Obstructed labor
Prolonged, obstructed labor is the leading cause of vesicovaginal fistula worldwide. Obstructed labor occurs when the uterus contracts normally during childbirth but the baby does not pass through the birth canal. It could occur in conditions like a big baby, an abnormally positioned baby or a small maternal pelvis or birth canal. Very young mothers are physically immature to have babies, and often suffer from obstructed labor. The head of the fetus may press against the maternal bones of the pelvis, thereby compressing the tissues of the anterior vaginal wall and the bladder. As a result, these tissues do not get enough blood supply and slough off, resulting in a fistula.
Traumatic cause
Trauma to the pelvic regions could damage tissues of the bladder and vagina and result in a vesicovaginal fistula. Such trauma could be due to:
- Instrumental delivery: Sometimes, when the delivery is prolonged, the fetus is brought out with the help of an instrument called a forceps. The use of forceps for delivery can cause trauma to the pelvic tissues
- Abdominal operations like a C-section delivery, surgical removal of uterus (hysterectomy), or operations on the urinary tract or lower gastrointestinal tract
- A fall on a pointed object, or use of a stick for criminal abortion
Cancer
Advanced cancer of cervix, vagina, or bladder may produce a vesicovaginal fistula by direct spread to the surrounding organs. In addition, radiation used for the treatment of cancer cervix might result in the development of a fistula. However, it usually takes a long time (1-2 years) to develop such a type of fistula.
Infective cause
Chronic infections such as vaginal tuberculosis, lymphogranuloma venereum, schistosomiasis or actinomycosis may also produce a vesicovaginal fistula.
What are the Symptoms and Signs of Vesicovaginal Fistula?
Most women with vesicovaginal fistula are young women who were pregnant for the first time and give a history of a difficult labor or the use of instrumental vaginal delivery to deliver the baby. Symptoms include the following:
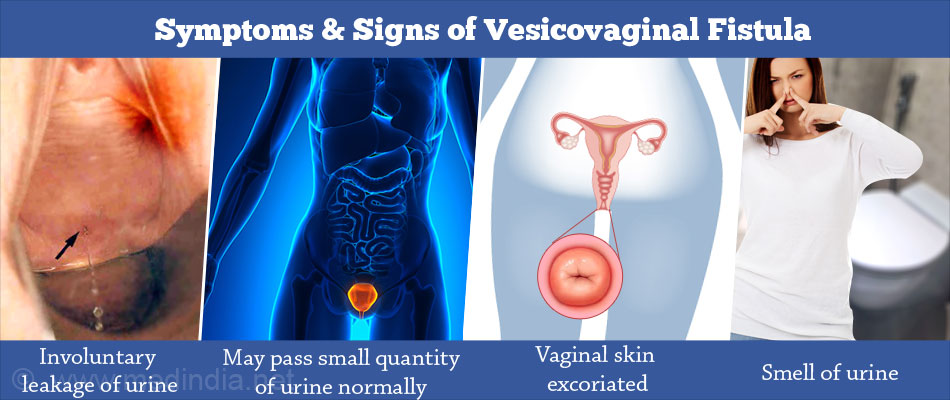
- Continuous leakage of urine occurs through the vagina during the day as well as the night (true incontinence), which is the characteristic feature.
- In a large fistula - There is no urge to empty the bladder, because the urine seldom stays in the bladder.
- In a Small Fistula - The patient may pass urine normally too and also leak urine through the vagina and sometimes only in certain positions. Leakage of urine following a difficult surgery occurs on first postoperative day itself or once the cathter is removed; however, fistula following obstructed labor may take three to five days to develop. Fitulas after radiation could develop several months or years following the treatment – this happened commonly after radiation after cervical cancer.
- The vaginal skin appears red or inflammed and excoriated.
- The smell of urine may be noted.
How do you Diagnose Vesicovaginal Fistula?
Diagnosis of vesicovaginal fistula is easily made based on the medical history of the patient and local examination. Tests may be required in cases where the diagnosis is not clear.
- Physical examination- The patient is placed in knee chest position and while examining the anterior vaginal wall; bubbles of air can be seen through the small tiny fistula, while the patient is asked to cough.
- Dye test-A speculum is introduced into the anterior vaginal wall, which is dried with the help of a swab. Meanwhile, methylene blue dye is introduced into the bladder through a catheter, and soon the dye is seen coming out of the vaginal opening if a vesicovaginal fistula is present.
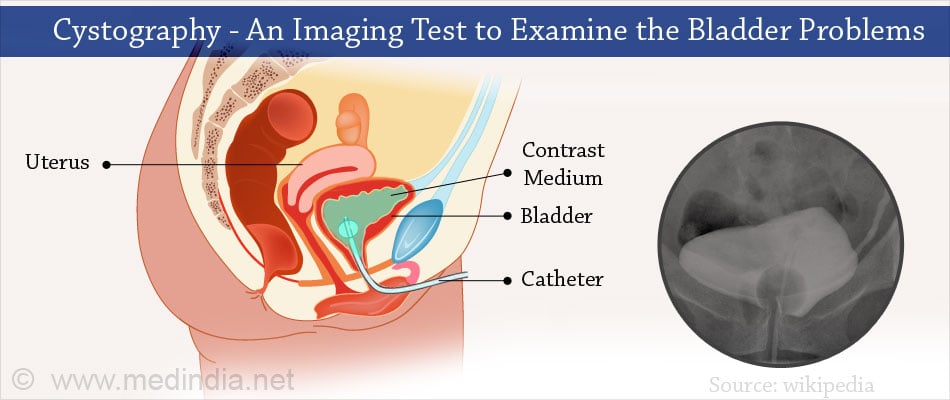
- Other investigations- Other tests like cystography, intravenous urography, retrograde ureterogram, and rarely hysterosalpingography may be required. Cystoscopy may also be done to confirm the diagnosis.
- Occasionally ultrasound, CT scan or MRI may be employed if the diagnosis is not clear or an injury to another part is suspected.
How do you Treat Vesicovaginal Fistula?
Conservative management for small fistulas:
Fistuals under 0.5 cms can be managed conservatively
Indwelling catheter:Once the diagnosis is made and if the fistula is small and the patient leaks urine occasionally, a catheter is introduced into the bladder and is kept there for 6-8 weeks. This minor procedure could result in the spontaneous closure of fistula tract..
Electrocoagulation of the fistula tract with a negligible coagulation current delivered through a small electrode introduced either through the vagina or the urethra has been utilized effectively in a few patients with fistulas under three millimeter in diameter.
Definitive management: Larger fistulas are best managed surgically.
Preoperative management: Women with vesicovaginal fistula usually belong to poor socioeconomic strata where health services are inadequate and the general health conditions are poor. Improvement of the general health condition is mandatory prior to surgery so that the patient is fit for surgery. Local infection of vulva is treated by application of silicone barrier cream or glycerin. Urinary antiseptics must be started 3-5 days prior to surgery.
Surgery
The ideal time for surgery of vesicovaginal fistula due to obstructed labor is after three months following delivery. By this time, the general condition of the woman improves and the local tissues are likely to be free from infection. The repair is done through either the vagina or the abdomen, or through a combined approach depending upon the choice and expertise of surgeon. Laparoscopic surgery is also sometimes used.
Postoperative advice
Continuous bladder drainage with a urethral catheter is mandatory following the surgery. This guarantees that the repaired area is kept pressure free and allows the tissues to heal. If the surgery was done through an abdominal approach, another catheter called the suprapubic catheter is introduced into the urinary bladder through the lower abdomen. All catheters must be checked routinely to guarantee that they stay patent.
While being discharged from the hospital, the patient is advised
- To pass urine more frequently
- To avoid intercourse for at least three months
- To delay pregnancy for at least one year. In cases the woman does get pregnant before that, she should receive adequate check-ups during the pregnancy and the delivery should be conducted via a cesarean section.
Failure of surgical repair: If the initial surgical repair fails, local repair should again be done after 3 months. The fistula becomes smaller after the successful second attempt.
In case of repeated failures and if no other options are available, a procedure called as urinary diversion can be done as a last resort. In this procedure, the ureters are diverted into the lower intestines, thereby creating a bypass for the urine stream that is coming out of the vagina.
How do you Prevent Vesicovaginal Fistula?
Some of the ways to prevent a vesicovaginal fistula are:
- Adequate antenatal care should be extended to at risk mothers who are likely to develop obstructed labor. A cesarean section should be planned for those who need it.
- In case of a long-standing obstructed labor, the urinary bladder should be drained continuously for a period of 5-7 days following the delivery of the baby.
- Care must be taken to avoid injury to the urinary bladder during any pelvic surgery.