- What are spermatoceles: Urology Care Foundation - (https://www.urologyhealth.org/urologic-conditions/spermatoceles)
- Spermatocele - (https://www.mayoclinic.org/diseases-conditions/spermatocele/symptoms-causes/syc-20377829)
- Bhatt S, Jafri SZ, Wasserman N, Dogra VS. Imaging of non-neoplastic intratesticular masses. Diagn Interv Radiol. 2011 Mar; 17(1): 52-63. doi: 10.4261/1305-3825.DIR.3116-09.0.
- Ghaznavi AM, Nakamura M, Tepper D. An analysis of 72% chromated glycerin used for sclerotherapy: sterility, potency, and cost after extended shelf life. Dermatol Surg. 2015 Jan; 41(1): 121-5. doi: 10.1097/DSS.0000000000000239.
- Rioja J, Sánchez-Margallo FM, Usón J, Rioja LA. Adult hydrocele and spermatocele. BJU Int. 2011 Jun; 107(11): 1852-64. doi: 10.1111/j.1464-410X.2011.10353.x.
What is Spermatocele?
Spermatocele, also known as an epididymal cyst, is a sperm (semen) filled cyst that is present in the upper part at the backside of the testes. The cyst is present in the epididymis, the convoluted tubule that originates in the testes and carries sperms to the outside. The spermatocele is usually a painless, benign (non-cancerous) mass that contain sperms. It is not a serious medical problem but may be bothersome and a nuisance for the patient. It usually occurs in the age group 20-50 years.
Anatomy & Physiology of the Male Reproductive System in Brief
The male reproductive system consists structures that facilitate the transfer of sperms to the female for the purpose of reproduction.
The testes are oval bodies and are the primary site where the sperms develop and mature. The testes also produce testosterone, the male sex hormone. There are two testes, one on either side and are placed within a sac called scrotum, which provides protection to the testes. Another function of the scrotum is to provide the optimal temperature for sperm development. When the temperature is high it hangs down more to provide a cooler environment and if the temperature is low, the scrotal muscles contract and bring the testes closer to the body to provide warmth.
The epididymis is a long, highly convoluted tubule that provides the environment for the sperms to mature and develop the ability to swim. This opens into the next part – the vas deferens.
The vas deferens transports the sperms to the urethra. One vas deferens from either side passes behind the prostate gland and joins with the seminal vesicles. The vas deferens is intertwined with muscles, nerves and blood vessels, collectively forming the spermatic cord.
The secretions from the prostate and seminal vesicles nourish the sperms and form the major volume of semen, the fluid (containing the sperms) that is ejaculated into the female genital tract. Besides this, an alkaline mucus secretion produced by the Cowper’s glands is also added to the semen.
The urethra has a dual role since it is a part of the urinary system as well as the reproductive system. It carries urine from the urinary bladder to the outside, as well as the semen during ejaculation. The urethra is continuous with the penis that is the external structure that transfers the sperms into the female genital tract.
What are the Causes of Spermatocele?
The exact cause of a spermatocele is not known. It occurs due to blockage in the epididymal ducts that carry sperms from the testes. Infections and inflammation of the epididymis (epididymitis), physical injury, and vasectomy can also play a role in the pathogenesis of spermatoceles. Research into the possible etiology of spermatoceles is ongoing.
What are the Symptoms and Signs of Spermatocele?
The condition does not usually exhibit any symptoms and signs. However, the following symptoms can be observed if the spermatocele becomes large in size:
- A lump in the affected testis, located at the upper and rear end.
- The affected testis may be heavier and cause discomfort.
- Mild pain may occur in the affected testis.
It should be noted that the symptoms of a spermatocele can mask other possible underlying conditions such as cancer, varicoceles, hematoceles, as well as testicular torsion resulting from rotation and twisting of the testes within the scrotal sac.

How do you Diagnose Spermatocele?
A spermatocele can be discovered by self-examination or during a health check-up. The doctor usually uses the following approaches for the diagnosis of a spermatocele:
- Physical Examination: A thorough physical exam of the testes and associated structures is usually sufficient for locating a spermatocele. The doctor will feel the area for any lumps, tenderness or pain.
- Transillumination: A torch is usually used to illuminate the scrotal sac from one side and the doctor looks from the opposite side. This method can clearly spot any cysts within the scrotal sac.
- Ultrasonography: If all else fails, a scrotal ultrasound can reveal the presence of a spermatocele.
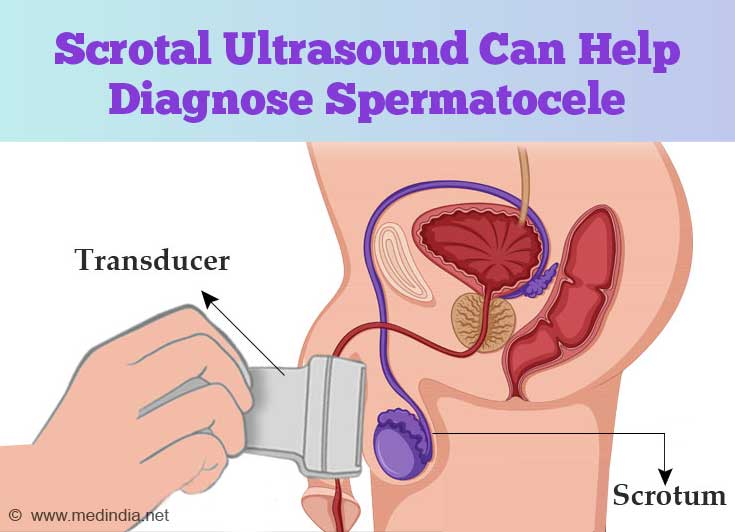
How do you Treat Spermatocele?
Spermatoceles are better left alone if the size is stable. However, if the lump continuously increases in size and is symptomatic to the patient then various treatment approaches may be adopted.
Medications: For pain and inflammation, the patient is usually prescribed painkillers like paracetamol and non-steroidal anti-inflammatory drugs (NSAIDs) like ibuprofen. These two drugs are also available as a combination.
Invasive Techniques: The invasive techniques include aspiration, sclerotherapy, and spermatocelectomy.
- Aspiration: A sterile injection needle is aseptically inserted through the scrotal sac, into the spermatocele and the accumulated fluid is aspirated out.
- Sclerotherapy: In this therapy, irritant agents such as hypertonic saline, sodium tetradecyl sulfate, polidocanol, and chromated glycerine are aseptically injected into the spermatocele. These cause irritation and scarring that prevents the fluid from accumulating, resulting in shrinkage of the cyst.
- Spermatocelectomy: This surgery is done when the spermatocele shows symptoms that may be a nuisance or a major cause of embarrassment for the patient. The aim of the surgery is to excise the cyst while keeping the other structures intact. However, sometimes a portion of the epididymis may have to be removed along with the cyst. This is usually an outpatient procedure done under local or general anesthesia so that the patient is discharged the same day. The procedure takes less than an hour to complete. There are usually no complications, but there is a chance of recurrence of the spermatocele.
How do you Prevent Spermatocele?
There is generally no way to prevent a spermatocele from occurring. However, regular self-exams can detect the condition at an early stage so that treatment measures can be instituted as soon as possible








