- Vesicoureteral Reflux Vur and Reflux Nephropathy - (http://www.infokid.org.uk/vesicoureteral-reflux-vur-and-reflux-nephropathy)
- Vesicoureteral Reflux - (https://www.niddk.nih.gov/health-information/urologic-diseases/urine-blockage-newborns/vesicoureteral-reflux)
- Reflux nephropathy - (https://medlineplus.gov/ency/article/000459.htm)
What is Reflux Nephropathy?
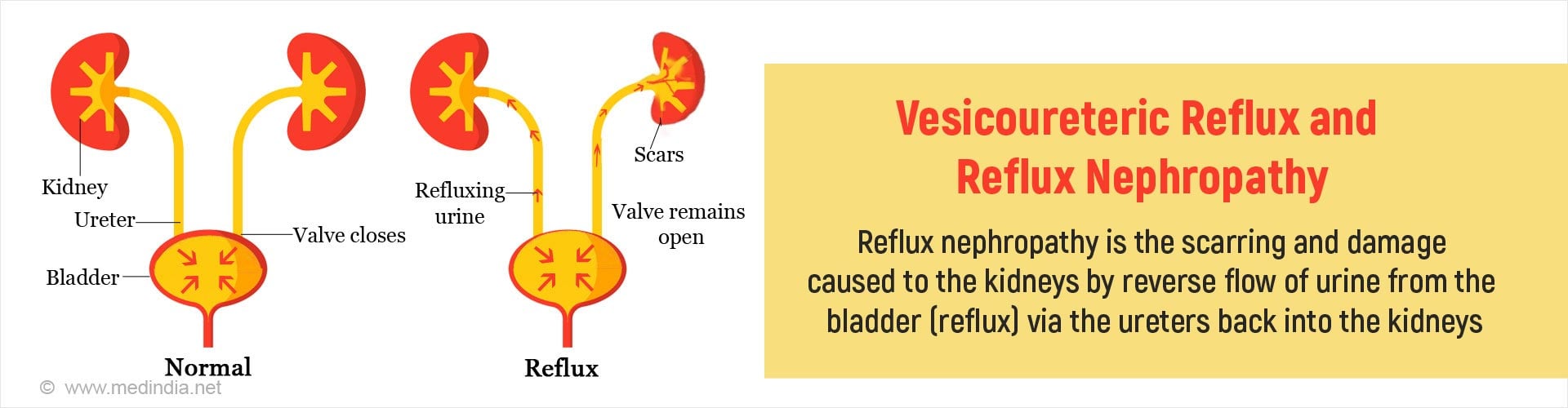
Normally urine is formed in the kidneys and flows in the downward direction into the ureters and then into the urinary bladder where it remains until the person voids the urine via the urethra. The urine in the bladder will not flow backwards into the ureters as this is prevented by a special mechanism at the junction of the ureters and the bladder. The ureters enter the muscular bladder through a tunnel at an angle. When the bladder contracts, the openings of the ureters close thereby preventing backflow of the urine.
Reflux refers to something which passes or flows backwards. In reflux nephropathy, the urine flows in the reverse direction from the bladder back into the ureter and then up into the kidneys. The phenomenon of the backward flow of urine from the bladder into the ureter is termed “vesicoureteric reflux”, vesico referring to the urinary bladder. It can occur on one or both sides.
The term reflux nephropathy was coined in 1973 by Bailey to describe the coarse renal scarring occurring in one or both kidneys in relation to a primary vesicoureteric reflux (VUR) and urinary tract infection (UTI). It replaced the older terminology of “chronic atrophic pyelonephritis” which had been in use since several years and erroneously implied that there was a persistent low-grade infection/inflammation occurring in the affected kidneys.
What are the Causes of Vesicourethral Reflux / Reflux Nephropathy?
As stated earlier, renal scarring secondary to vesicoureteric reflux (VUR) is referred to as reflux nephropathy. Vesicoureteric reflux can be primary or secondary.
Primary Reflux
The majority of cases of reflux are due a developmental abnormality occurring before birth. This is primary vesicoureteral reflux. One or both ureters enter the bladder at an abnormal angle. Consequently, when the bladder contracts to pass urine outwards, the opening of the ureter into the bladder does not close properly. As a result, some of the urine passes back up the ureters into the kidneys.
Primary VUR is ten times more common in Caucasian children than Blacks, and seen more commonly in girls than in boys. It is generally diagnosed in children under 5 years.
As the child grows, the ureters elongate and become straighter, which may improve valve function with spontaneous resolution of the reflux. Primary vesicoureteral reflux has a tendency to run in families, which indicates that it may be genetic, but the exact reason for the defect is unknown.
Secondary Reflux
Occasionally, reflux nephropathy can occur due to problems acquired after birth, (secondary reflux nephropathy) resulting in blockage of urine outflow out of the bladder or the ureters, or urinary system dysfunction. These include the following:
- Bladder calculi or stones that may block normal passage of urine
- Prostatic enlargement in men resulting in urine outflow obstruction
- Anterior or posterior urethral valves, which are anomalies present at birth
- Neurogenic bladder where person is unable to pass urine due to primary neurological condition such as spinal cord injury and multiple sclerosis
- Kidney transplant leading to swelling of ureters
- Radiation therapy that may cause scarring of the ureters
- Detrusor muscle instability, where the bladder muscle is unable to contract properly
What are the Risk Factors for Vesicoureteral Reflux / Reflux Nephropathy?
- Family history of reflux
- Girl child
- Caucasian children
- Recurrent urinary tract infections (inflammation leads to scarring and can cause obstruction)
What are the Signs and Symptoms of Vesicoureteric Reflux / Reflux Nephropathy?
- VUR in children is usually asymptomatic
- Some children may present with bedwetting (nocturnal enuresis)
- It is usually suspected when a child under 5 years has recurrent urinary tract infections (UTIs) with fever, abdominal pain, frequency and burning sensation while passing urine
- Untreated reflux in childhood may lead to chronic kidney disease during adolescence with hypertension, urine protein and evidence of deranged kidney function on blood tests
How do you Diagnose Vesicoureteral Reflux / Reflux Nephropathy?
When a diagnosis of reflux nephropathy is suspected, for example in a child with recurrent urinary infections or a strong family history is present, one or more of the following tests may be performed before a diagnosis of reflux nephropathy is made.
Testing is recommended in the following situations:
- Family history of VUR, including an affected sibling
- Babies diagnosed with urinary obstruction during pregnancy ultrasound scan
- UTI occurring in children less than 5 years
- Children with a UTI and fever, irrespective of their age
- UTI in boys who are not sexually active, regardless of their age or the presence of fever
Urine Test
The urine may be examined to look for presence of pus cells or other evidence of urinary infection and for presence of protein indicating kidney damage.
Blood Tests
Blood tests are done to measure kidney function and to look for other causes of kidney damage.
Abdominal Ultrasound
This is an imaging test using sound waves (the sound waves are too high pitched for humans to hear). A probe is pressed gently on the skin, with some jelly applied on the skin to make a good contact. Ultrasound is painless, non-invasive and harmless, and can easily be performed on babies as well as older people.
Ultrasound performed at 20 weeks of pregnancy may identify enlarged and swollen kidneys in the fetus. These babies may be investigated for VUR following birth.
The test can determine the size and shape of the kidneys, and reveal enlarged ureters (tubes from kidney to bladder). It can also detect if the bladder empties fully. However, ultrasound cannot say if VUR is present. Therefore other tests may be necessary.
Intravenous Urogram (IVU) / Intravenous Pyelogram (IVP)
In an IVU/IVP, images of the kidneys and ureters are captured by a series of x-ray pictures following injection of an x-ray contrast dye into the arm which will delineate the structures more clearly. This test also may not show presence of VU reflux with 100% certainty.
Micturating or Voiding Cystogram (MCG)
Micturating’ means passing urine. Cystogram refers to imaging of the bladder. In micturating cystourethrogram (MCUG), a hollow tube (catheter) is passed into the bladder from the urethra and x ray contrast dye is injected into the bladder. While the person passes urine, images of the bladder are obtained. This test can determine the presence of reflux and assess the need for surgery.
Other tests:
Cystoscopy - In some cases, the interior of the bladder can be visualized using a specialised called cystoscope. During cystoscopy, performed by urologists, the doctor may be able to see abnormal ureters, or take pictures during the procedure which may show the presence of VUR.
Micturating radio-isotope scan - This is a specialized imaging scan performed by injecting a slightly radio-active fluid into the bladder though a tube. Similar to MCUG, images of the bladder are obtained when the patient is passing urine. Radiation exposure is equivalent to or less than in MCUG.
DMSA (dimercaptosuccinic acid) scan and MRI Urogram are other advanced imaging techniques that can be used if other tests come out as non-diagnostic.
How do you Treat Vesicoureteric Reflux / Reflux Nephropathy?
Primary Vesicoureteric Reflux
Vesicoureteric reflux (VUR) is divided into five grades. Grades 1 and 2 indicate mild disease whereas Grades 3,4 and 5 indicate more severe disease.
The treatment depends on the grade and severity of the VUR. Most children outgrow the VUR with spontaneous resolution by 5 years and treatment may be required only in their preschool years.
Children who have VUR should also be assessed for presence of bladder and bowel dysfunction (BBD). Children with BBD symptoms such as constipation, fecal incontinence, sudden urge to pass urine, daytime wetting, or pain in the genital area are at greater risk of kidney damage due to infection.
Mild VUR
Children with mild degree of VUR may be referred to a child specialist (pediatrician), who may prescribe antibiotics to treat urinary infections. These children should have regular urine tests to rule out urinary infections and ultrasound scans periodically to ensure the kidneys are normal and not getting damaged.
Severe VUR
Children with more severe VUR and presence of BBD may be given antibiotics at a low dose to prevent urinary infections, while simultaneously treating the BBD as well. They should undergo periodic urine examinations and ultrasound scans to monitor for scarring or damage to the kidneys.
Children who continue to have recurrent infections despite antibiotics or have reflux even after five years of age may be referred to the pediatric urologist who will assess the need for surgery. Surgery may be recommended to treat severe VUR and prevent kidney damage and scarring. The following types of surgery are usually performed:
Gel Injection
The initial procedure that is usually recommended is to inject a gel into the terminal portion of the ureter within the bladder. This reduces gap, preventing urine reflux out of the bladder into the ureters, without obstructing urine flowing into the bladder.
This is a quick procedure usually done as a day procedure. It can be done on babies and children of any age. The child will usually be discharged on the same day.
Ureteric reimplantation
Ureteric reimplantation is a more invasive procedure done under general anesthesia and requires a slightly longer hospital stay. The procedure involves disconnecting the ends of the ureters from the bladder and re-connecting them at the proper angle to create a valve mechanism.
Following either of the above procedures, there is a reduction in VUR with reduced risk of kidney damage. However, longterm followup is required to ensure that the kidneys are normal.
Secondary Vesicoureteric Reflux
Secondary VUR is treated by managing the blockage causing the reflux. Depending on the cause, treatment may be:
- Surgery - prostatectomy for enlarged prostate
- Antibiotics - to treat urinary repeated infections
- Intermittent catheterisation - draining the urine periodically by inserting a thin tube, called a catheter through the urethra into the bladder
What are the Complications of Reflux Nephropathy?
The scarring of the kidneys due to repeated infection and inflammation following VUR can result in the following complications:
- Kidney stones
- Hypertension
- Proteinuria (loss of protein in the urine)
- Chronic kidney disease