- Prenatal Testing - (http://americanpregnancy.org/prenatal-testing)
- Handbook of prenatal diagnosis by Ronald J trent
- Journal of Prenatal Diagnosis and Therapy, by J Prenat Diagn Ther
- Cochrane Search - Second trimester serum tests for Down's Syndrome screening; Authors: S Kate Alldred, Jonathan J Deeks, Boliang Guo, James P Neilson, Zarko Alfirevic, Mary Pennant
- Prenatal Testing - (http://americanpregnancy.org/prenatal-testing)
- Spina Bifida - (http://americanpregnancy.org/birth-defects/spina-bifida/)
- Frequently Asked Questions about Prenatal Screening for Downs Syndrome and Neural Tube Defects - (http://library.nhsggc.org.uk/mediaAssets/Medical%20Genetics/Prenata%20Screening%20FAQ.pdf)
- Chorionic villus sampling and amniocentesis - (https://www.rcog.org.uk/globalassets/documents/patients/patient-information-leaflets/pregnancy/pi-chorionic-villus-sampling-and-amniocentesis.pdf)
- Prenatal screening and diagnostic tests - (http://www.health.wa.gov.au/docreg/Education/Prevention/Genetics/HP3131_prenatal.pdf)
Prenatal Screening - Introduction
Got your pregnancy test positive! It’s one of the most amazing feelings for couples. Here starts the nine months desperate wait to hold your baby in your arms. These nine months bring to you different experiences in and around you, including granny advice, doctor visits and multiple screenings.
Expectant mothers are advised several screening tests during their 40 weeks of pregnancy, even those whose chances of having a baby with a defect are low, to ensure no defect, good health and normal development of the fetus. A pregnant woman is advised multiple pre-natal screening tests in first and second trimester to check the health and development of the baby. These tests are absolutely safe and non-invasive.

The major objective of these tests is to rule out the genetic and developmental abnormalities in the baby. Every woman stands a small chance of having a baby with chromosomal anomaly or neural tube defect. Some women may fall under high risk category. The routine screening tests that are usually done don’t give a definitive diagnosis. Therefore, women in high risk category are further advised to undergo advanced screening tests to confirm the chances of baby being born with a genetic disorder or a developmental birth defect.
It is completely the patient’s choice to undergo prenatal screening, or to undergo only selective tests under the screening umbrella. Nevertheless, it is advisable to undergo prenatal screening tests to ensure the health and well-being of the baby and have the opportunity to correct some of the defects in-utero if required.
Routine pre-natal screening tests involve a combination of blood test and ultrasound scans. Ultrasound scan helps detect risk of physical (developmental) abnormalities whereas blood tests helps detect risk of inherited disorders.
What is Pre Natal Screening?
Prenatal screening tests help detect the risk of inherited disorders including chromosomal abnormalities such as Down syndrome, neural tube defects, or birth defects like congenital heart disease in the unborn baby.
In routine first trimester screening, levels of hCG (Human chorionic gonadotropin) and PAPP-A (pregnancy-associated plasma protein A) in maternal serum are detected, combined with the measurement of nuchal translucency (NT).
Second trimester screening is done by estimating the levels of AFP (alpha feto-protein) inhibin-A, estriol, and hCG in the woman's blood.
If the results of first and/or second trimester prenatal screening falls under high risk category, further advanced tests will be advised by the doctor like Chorionic villus sampling, amniocentesis, and cell free fetal DNA to reach a definitive diagnosis.
Who Should Undergo Mandatory Prenatal Screening?
While all pregnant women must undergo prenatal screening, there are certain women who fall under high risk category and must mandatorily undergo screening. They are women who:
- Are over 35 years of age
- Have been exposed since conception to a substance or substances like alcohol that might be harmful to the developing baby
- Have a family history of genetic disease or have been the carriers of a disease or have a genetic disorder themselves
- Have been exposed to infections such as rubella or toxoplasmosis that can cause a birth defect
- Have had previous babies with inherited defects
- History of multiple miscarriages
- Having twin or multiple pregnancy
- Racial origin - For instance cystic fibrosis is more common in Caucasians of North European origin
- Intermarriage or marriage between first cousins increase the baby’s risk of genetic disorders
What are the Routine Prenatal Screening Tests in First Trimester?
Prenatal screening in first trimester is done in three parts:
Nuchal Translucency Scan (NT Scan)
An ultrasound scan is done to measure the space at the back of the fetal neck for increasing fluid or thickening. In addition to this ultrasound also examines the presence of fetal nasal bone. An increased nuchal thickening or an absence of the nasal bone increases the risk of a baby with Down syndrome. It must be done in 11th – 14th week of pregnancy because till the fourteenth week base of fetal neck is transparent. The thicker the Nuchal Translucency, the higher the chance of developing genetic abnormality at this gestational age. Timing is very crucial since nuchal fold becomes less and less transparent as the pregnancy progresses. This test also helps detect congenital heart defect. Increased NT measurement may also be linked to high risk of preterm labor.
The report would read the result as e.g. 1 in 4000,1 in 100 etc. This interprets that out of every 100 women with this result, one will have Down syndrome. The higher the denominator, lower the risk.
Blood Test –Blood test is taken when pregnancy is at 9-11th week.
- Pregnancy associated plasma protein screening (PAPP-A) - It measures a protein which is produced by placenta and passed into the mothers blood stream. Lower levels indicate higher risk of developing either of the trisomies namely Trisomy 21, 18 and 13.
- Human Chorionic Gonadotrophin (HCG Screening) - It measuresa hormone produced by the placenta in early pregnancy and passed into maternal bloodstream. High levels of. β hCG is associated with an increased risk of Trisomy 21, while lower levels of β hCG is associated with an increased risk of Trisomy 18 and 13.
The doctor would want to see both the reports. They help in determining the risk of chromosomal defects like Down syndrome, Trisomy 13 and Trisomy-18. This is called combined screening. An abnormal result doesn’t mean that the baby has chromosomal problem, just that there is increased risk of developing the same. Most of such women go on to have a normal baby with no defect.
Therefore, if the result falls under high risk category, one might be advised to go in for an advanced prenatal screening test like Chorionic villus sampling, amniocentesis, cell free fetal DNA to reach a definitive diagnosis. This would further help make an informed decision on whether to continue with the pregnancy or not. First trimester screening is more important since it is still an early stage of pregnancy. Detecting a fetal disease at this stage provides an opportunity to decide on possible termination of pregnancy.
What are the Prenatal Screening Tests in Second Trimester?
Second trimester prenatal screening may include several blood tests, called multiple markers, also called as quad screening. Quad screening measures the levels of four substances produced by fetus or placenta and passed in mother’s bloodstream; alpha – fetoprotein (AFP), hCG, estriol and inhibin-A.
Screening is done between 14th and 22nd weeks of pregnancy, by drawing a blood sample of expectant mother. Abnormal results of AFP and other markers may indicate the need for additional testing.
Integrated screening combines the results of test conducted in first and second trimester. The accuracy level of detecting an abnormality is greater through integrated screening rather than using just one screening independently.
High AFP may mean
- More than one fetus or multiple pregnancy
- Baby is much older than the gestation age given by the doctor.
- Neural tube defect such as Spina bifida
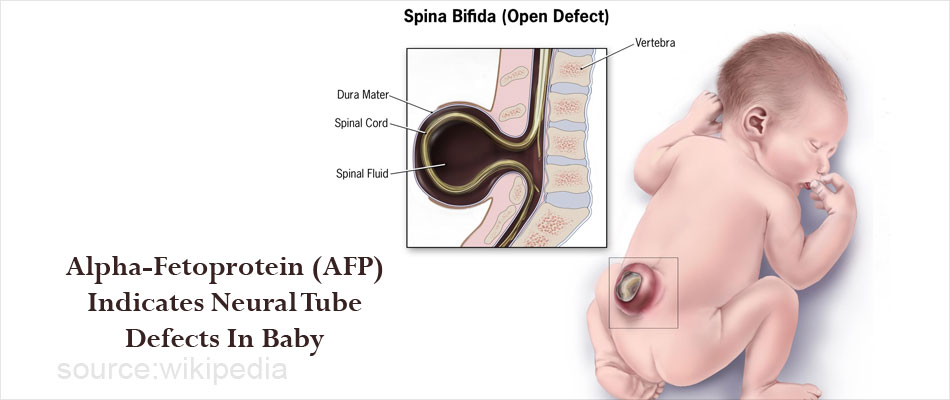
- Abnormality in the baby's esophagus
- Abnormal opening in baby’s head or abdominal wall.
Low AFP, low estriol, high hCG, and high inhibin A indicate high risk for Down syndrome. Low levels of AFP, estriol and hCG means baby has a higher risk of having trisomy 18.
What are the Advanced Prenatal Tests for Detecting Genetic Disorders in Fetus?
Cell-free fetal DNA analysis– This test analyzes the fetal DNA circulating in mother's blood stream. Fetal DNA is the reflection of the genetic makeup of the developing baby. The mother's blood sample is tested after 10 weeks of gestation. If it indicates high risk of Down syndrome, a more invasive diagnostic test may be used to determine the risk further. Prenatal cell-free DNA screening is very sensitive and specific in identifying the risk of fetal abnormalities and to identify women in whom risk of miscarriage is high.
Chorionic villus sampling (CVS) - In this procedure, some cells are removed from the placenta and tested for chromosomal abnormalities, like Down syndrome, Cystic fibrosis, Tay-Sachs disease and Fragile X syndrome. CVS cannot test for neural tube defects or other anatomical defects. Placenta has same chromosomal makeup as the developing baby; therefore cells are taken from the finger like projections of placenta called chorionic villi, so the name chorionic villus sampling.
It is performed between 10th and 13th week of pregnancy. It has an advantage over amniocentesis. Since it is performed in first trimester, it gives results earlier then amniocentesis which are performed in 16th week. It is safe and reliable with very minimal miscarriage rate.
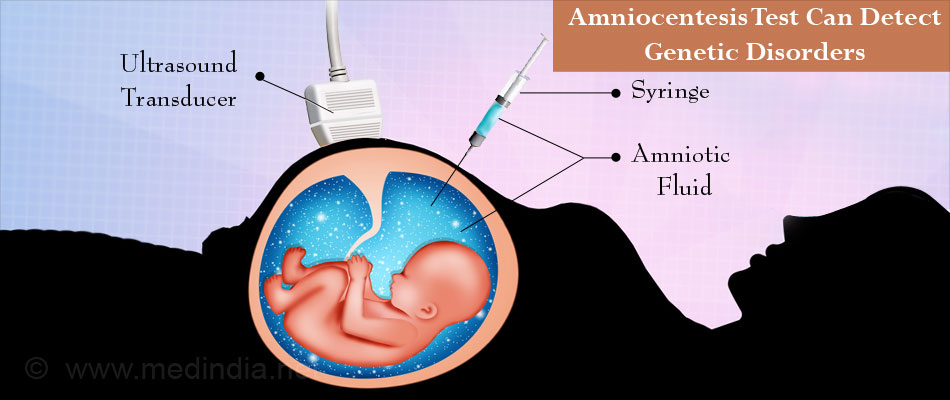
Amniocentesis – This test is performed between 15th and 18th week of pregnancy, 16th being most ideal. A sample of the amniotic fluid surrounding the fetus is withdrawn by inserting a needle through the abdomen into amniotic sac and withdrawing amniotic fluid sample. This sample is analyzed for the chromosomes of the fetus. This analysis can detect both neural tube defects and genetic disorders. It carries slight risk of miscarriage; risk becomes higher if performed before 16th week.
Cordocentesis – This test is also known as percutaneous umbilical blood sampling or PUBS. In this test, fetal blood is taken from a vein in the umbilical cord and examined for chromosomal defects. This test is done only after 18th week of pregnancy. An ultrasound scan is used to determine the location where umbilical cord inserts into the placenta. Ultrasound guided needle is inserted through the abdomen and uterine walls to the umbilical cord and a small sample of fetal blood is withdrawn. This test carries a significant risk of miscarriage as compared to other tests and therefore offered as the last option, when other tests fail to give clear results.







