- What is peripheral neuropathy? - (https://www.ninds.nih.gov/disorders/patient-caregiver-education/fact-sheets/peripheral-neuropathy-fact-sheet)
- Mononeuritis Multiplex - (https://www.ncbi.nlm.nih.gov/pmc/articles/pmc3193641/)
- Carpal tunnel syndrome - (http://www.mayoclinic.org/diseases-conditions/carpal-tunnel-syndrome/basics/definition/con-20030332)
- Compressive neuropathy in the upper limb - (http://www.aanem.org/patients/disorders/mononeuritis-multiplex)
- Peripheral Nerve System - (http://www.hopkinsmedicine.org/neurology_neurosurgery/centers_clinics/peripheral_nerve_surgery/conditions/peripheral_nerve_system.html)
- Overview - Peripheral Neuropathy - (http://www.mayoclinic.org/diseases-conditions/peripheral-neuropathy/home/ovc-20204944)
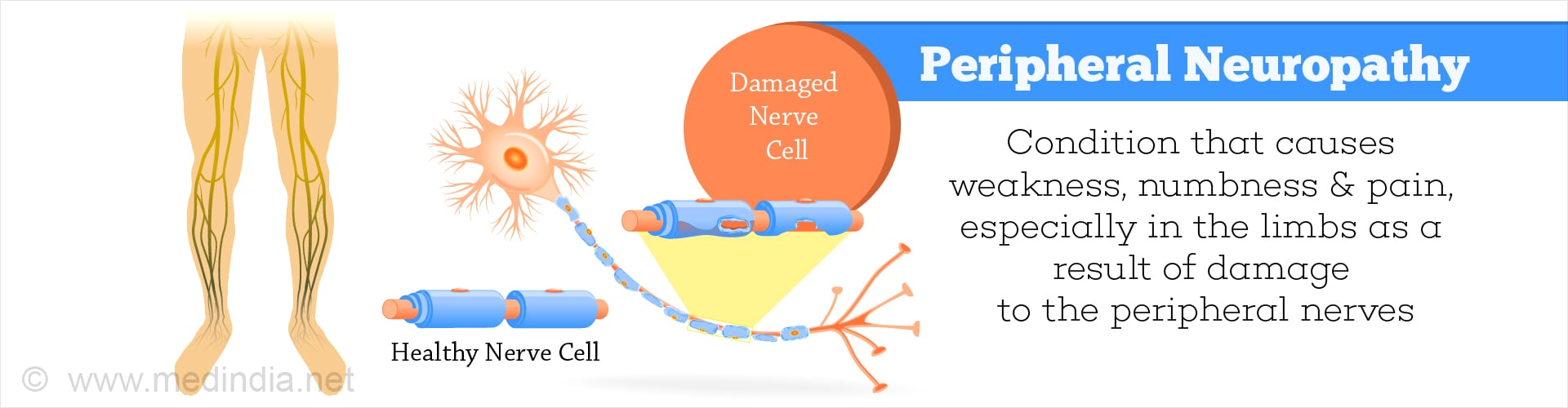
What is Peripheral Neuropathy?
Neuropathy means nerve disease or damage. Specific damage to one or more of the peripheral nerves, that can cause weakness, numbness, pain and a pricking sensation, especially in the extremities is known as peripheral neuropathy.
Since the peripheral nerves are involved in sending messages or signals transmitted from the central nervous system to different parts of the body, damage to any of these nerves interferes with the vital connections between the brain and spinal cord and rest of the body; in other words the signaling processes are affected.
Around 20 million people in the United States of America have some form of peripheral neuropathy.
In the U.K, 1 in 10 people aged 55 years and older are affected by some form of peripheral neuropathy.
Diabetic neuropathy accounts for 60% to 70% of all peripheral neuropathies.
What are the Types of Peripheral Neuropathy?
Classified on the basis of the onset of the disease there is:
- Acute peripheral neuropathy which is a sudden or rapid onset of neuropathy.
- Chronic peripheral neuropathy which develops more gradually and persists for a longer time.
Classified on the basis of the number of nerves that are involved there is:
- Mononeuropathy when only one nerve or nerve group is damaged.
- Polyneuropathy when all the nerves are damaged. This is the most common type of neuropathy. It starts by affecting the longest nerves and so usually the feet are first affected. It then starts spreading to the shorter nerves and gradually affecting the arms.
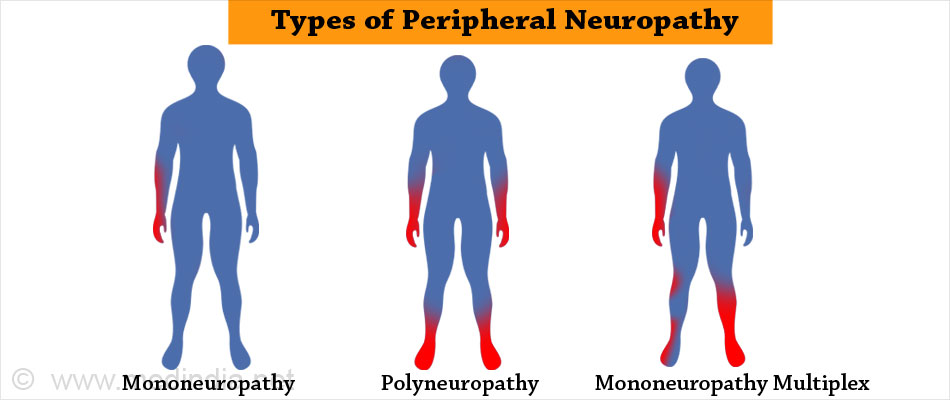
Another type of peripheral neuropathy is mononeuritis multiplex, also known as mononeuropathy multiplex or multifocal neuropathy.
It occurs as a result of damage to isolated nerves in two or more nerve areas. Mononeuritis multiplex is actually a group of symptoms. It affects people with diabetes mellitus or connective tissue diseases.
The symptoms of this condition include numbness, tingling, abnormal sensation, or restricted movement of the affected part of the body.
What are the Causes of Peripheral Neuropathy?
Peripheral neuropathy can either be inherited or acquired through a disease or trauma.
1. Diabetes Mellitus (DM), characterized by high and uncontrolled blood sugar is the most important cause of peripheral neuropathy. This condition is called diabetic polyneuropathy.
Diabetes mellitus leads to hormonal imbalances and disrupts the normal metabolic processes. It impairs the body’s ability to transform nutrients into energy and process waste products. In the long run, uncontrolled diabetes (after at least 25 years) can lead to the damage of nerves and polyneuropathy. In the United States, 60%-70% suffering from DM have some form of nerve damage.
2. Physical injury is the most common cause of acquired nerve injury. Injury or trauma from accidents, falls, sports-related activities, and surgical procedures can cause partial or complete damage to nerves. Broken or dislocated bones can exert pressure on neighboring nerves and cause damage.
Compression or entrapment neuropathy affects mostly the upper limbs and occurs as a result of compression on a nerve at some point over its course. The most common type of this injury is carpal tunnel syndrome followed by ulnar neuropathy. Sometimes it can be due to a compression bandage or a plaster of Paris cast.
Carpal tunnel syndrome occurs when the nerve passing through the wrist gets compressed. It causes numbness, tingling and hand weakness.
3. Autoimmune diseases are conditions in which the body's immune system attacks its own tissues. This can lead to nerve damage. Some autoimmune conditions that cause peripheral neuropathy are Sjogren’s syndrome, lupus, and rheumatoid arthritis.
Chronic autoimmune conditions can destroy joints, organs, and connective tissues, making nerve fibers more vulnerable to compression injuries and entrapment.
Chronic inflammatory demyelinating polyneuropathy (CIDP) is a condition that usually damages sensory and motor nerves, leaving autonomic nerves intact.
Multifocal motor neuropathy is a form of inflammatory neuropathy that affects motor nerves exclusively. It may be chronic or acute.
4. Kidney dysfunction can lead to the build up of toxic chemicals in the blood, affect the nerves and cause polyneuropathies.
5. Cancerous tumors can either arise from nerve tissues or exert damaging compression forces on nerve fibers. Chemotherapy induced toxicity can also cause peripheral neuropathy. Around 30%-40% of people who undergo chemotherapy develop peripheral neuropathy and it is a leading reason why people with cancer stop chemotherapy early.
The severity of chemotherapy induced peripheral neuropathy (CIPN) varies from person to person. Lowering doses of chemotherapy may help patients to ease their symptoms. In some cases, symptoms of neuropathy persist ling after stopping chemotherapy.
6. Infections can cause peripheral neuropathy. Certain viruses and bacteria like varicella-zoster (shingles), Epstein-Barr virus, West Nile virus, cytomegalovirus, and herpes simplex attack the nerves.
These infections can severely damage sensory nerves, causing attacks of sharp, lightning-like pain.
The human immunodeficiency virus (HIV) that causes AIDS is associated with several different forms of neuropathy, depending on the specific stage of active immunodeficiency disease. An estimated 30% of people who are HIV positive develop peripheral neuropathy.
7. Medications like antiretroviral drugs used to treat HIV, anticonvulsants used to treat epilepsy and certain heart and blood pressure medications can cause peripheral neuropathies.
8. Heavy alcohol consumption leads to nerve damage. Long term alcohol consumption leads to nutritional deficiencies, especially of vitamins including B12, thiamine, and folate and leads to peripheral neuropathies.

What are the Symptoms and Signs of Peripheral Neuropathy?
Symptoms of peripheral neuropathy depend on the nerves affected.
1. Motor nerves help carry electrical impulses from the brain and spinal cord to the muscles. These help in the voluntary movement of muscles. These impulses allow people to engage in walking, catching a baseball, or moving the fingers to pick something up.
Damage to motor nerves (motor neuropathy) can lead to
- Muscle weakness
- Difficulty walking or moving the arms
- Uncontrolled muscle twitching visible under the skin
- Muscle atrophy or severe shrinkage of muscle size
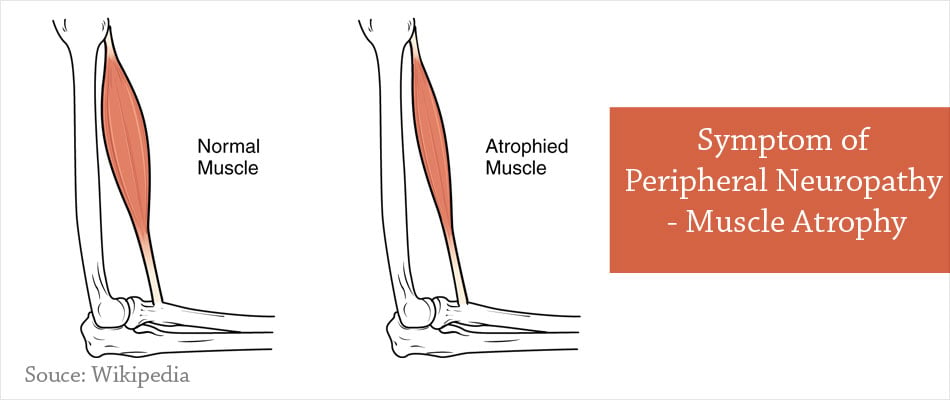
- Decreased reflexes
- Painful cramps and spasms
2. Sensory nerves are areas of the body that may become abnormally sensitive and help carry electrical impulses back to the brain and spinal cord. These signals helps in the sensation of cold, heat and pain.
Damage to sensory nerves (sensory neuropathy) can lead to
- Neuropathic pain which issevere pain (allodynia) from stimuli due to over-sensitization of pain receptors in the skin. This creates an exaggerated, intense experience of touch that would normally be painless. For example, bed sheets draped lightly over the body can also pain in people suffering from this condition.
- General decrease in the sensation of touch (tingling, numbness) and loss of reflexes (due to damage to large sensory nerves).
- Inability to feel pain of change in temperature (due to damage to smaller sensory nerves).
- Loss of pain sensation in people with diabetes; this contributes to a high rate of lower limb amputations among this population.
3. Autonomic nerves- These nerves carries signals to the organs and glands. These nerves helps to control involuntary or semi-involuntary functions that are not consciously directed, such as breathing, regular beating of heart, salivation, sweating, bladder control, digestion and blood pressure.
Damage to autonomic nerves (autonomic neuropathy) affects the involuntary functions and can cause
- Heat intolerance as it affects the ability to sweat normally.
- Bladder function control due to urine incontinence.
- Sudden drop in blood pressure that may result in dizziness, feeling light headed, or feeling faint.
- Intestinal muscle contractions that can lead to diarrhea, constipation, or incontinence. Some people may experience eating or swallowing difficulties.
- Irregular heartbeat.
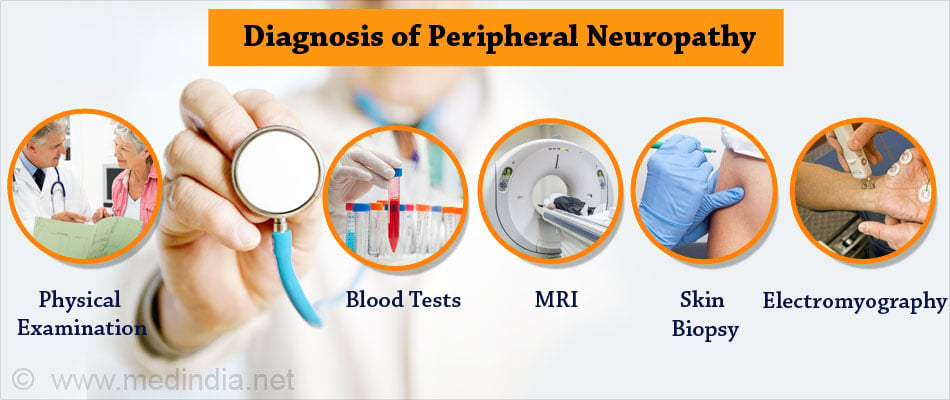
How do you Diagnose Peripheral Neuropathy?
1. History & Physical examination Includes taking a medical and family history and finding about their lifestyle such as drinking habits and any infection in the past.
A neurological examination which includes checking the reflexes, muscle tone and strength, evidence of cramps or spasms, posture, coordination and ability to feel sensations like pain and temperature is also done.
Other tests are suggested based on the results of neurological and physical examination and history.
2. Blood tests can detect diabetes, vitamin deficiencies, liver or kidney dysfunction, other metabolic disorders, signs of abnormal immune system activity or any other condition that can indicate peripheral neuropathy.
3. Imaging tests like computed tomograpy (CT) or magnetic resonance imaging (MRI) can help rule out tumors, herniated discs, or other abnormalities that may be causing the neuropathy.
4. Nerve biopsy involves removing a small portion of a nerve, usually a sensory nerve, often from the lower leg to look for abnormalities. It is an invasive procedure that is difficult to perform and causes neuropathic side-effects.
5. Skin biopsy - A small portion of skin is removed to look for a reduction in nerve endings. It helps to reveal damage present in smaller fibers. It is less invasive than nerve biopsy, is easier to perform and has lesser side-effects.
6. Electromyography (EMG) involves inserting a fine needle into a muscle torecord electrical activity in the muscles. It detects abnormal electrical activity in motor neuropathy and can help differentiate between muscle and nerve disorders.
7. Nerve conduction velocity (NCV) test measures the speed at which electrical signals pass through the nerves. Special electrodes are placed on the skin over the nerve being tested. These electrodes give off very small electrical impulses or shocks to the nerves which responds by generating its own electrical impulse. In peripheral neuropathy, this speed and strength of the impulses is reduced and impulses are blocked.
How do you Treat and Manage Peripheral Neuropathy?
Treating peripheral neuropathy aims at:
- Treating underlying condition or cause
- Managing pain and other symptoms
- Finding methods to achieve maximum independence
1. Treating underlying conditions:
It is important to identify any underlying condition causing peripheral neuropathy, such as diabetes or vitamin B12 deficiency, certain injuries, toxins, alcohol related neuropathy or certain medications.
- If diabetes is diagnosed, it can be controlled by making certain lifestyle changes like exercising and having a healthy diet. It is crucial to control blood sugar levels to avoid any further nerve damage.
- If injury is the cause of peripheral neuropathy, this may need physiotherapy, surgery or other treatment to relieve the pressure on the nerve caused by the injury.
- Deficiency of vitamins can be reversed by taking supplements or injections.
- Alcoholic neuropathy can be controlled by reducing and stopping alcohol intake.
2. Symptomatic Management:
Neuropathic pain is the main symptom associated with peripheral neuropathy and can be often difficult to treat. Various medicines are available to manage the pain.
Mild pain can be alleviated by certain common analgesics such as non-steroidal anti-inflammatory drugs (NSAIDs).
Chronic and discomforting pain can be managed by medicines like:
Anticonvulsant medicines that are commonly used to treat epilepsy such as gabapentin, pregabalin,topiramate, and carbamazepine.
Antidepressant medicines called tricyclic antidepressants such as amitriptyline or newer serotonin-norepinephrine reuptake inhibitors such as duloxetine hydrochloride or venlafaxine and Antiarrythmic medications like mexiletine.

These medications modulate pain through their mechanism of action on the peripheral nerves, spinal cord, or brain and tend to be the most effective types of medications to control neuropathic pain.
Approved narcotic drugs can be used as a last resort. One such drug is tapentadol approved for treating diabetes.
Topical application with lidocaine, an anesthetic agent, and capsaicin, a substance found in hot peppers will also help in relieving neuropathic pain.
Surgical intervention can be considered for some types of neuropathies especially in the case of compression or entrapment injuries as in the case of carpal tunnel of the wrist.
A non-invasive intervention used for pain relief is transcutaneous electrical nerve stimulation (TENS). It can be used in a range of conditions. The therapy involves attaching electrodes to the skin at the site of pain or near associated nerves and then stimulating the nerve using gentle electrical current. TENS is especially beneficial for peripheral neuropathy symptoms associated with diabetes.
Complementary approaches like acupuncture, massage, and herbal medications.
Certain mechanical aids like hand or foot braces help to reduce nerve compression and pain and aid in movement. To improve gait disturbances and help prevent foot injuries in people with a loss of pain sensation, orthopedic shoes can be used.
Other problems associated with peripheral neuropathy include erectile dysfunction, constipation, slow movement of food through your stomach (gastroparesis), erratic heart beat, blood pressure variations and loss of bladder control. These conditions can be managed using medications.
If bladder function gets affected manual expression of urine or self-catheterization may help.
3. Methods to Achieve Independence:
Depending on the severity of the condition, help with day-to-day activities may be needed. Taking the help of a physiotherapist who may offer advise to help improve muscle strength or the help of an occupational therapist who may be able to advise about special utensils and home adaptations to help with muscle weaknesses are some means to improve quality of life.
How to Prevent Peripheral Neuropathy
The best way to prevent peripheral neuropathy is to manage underlying medical conditions that increases the risk of peripheral neuropathy.
Other factors that help prevent peripheral neuropathy are making healthy lifestyle choices like:
- Including a diet rich in fruits, vegetables, lean meat and whole grains
- Taking care of deficiencies especially vitamin B12 deficiency by eating meats, fish, eggs, low-fat dairy foods and fortified cereals
- Engaging in regular exercise will help improve muscle strength
- Avoid smoking and alcohol intake as they interfere with circulation and affect nerves
- Regular monitoring of blood glucose levels

Health Tips
Monitor and maintain blood glucose levels- By keeping the blood glucose under control the effects of neuropathy can be controlled. Diabetics should especially take care of their feet by checking for blisters, cuts or calluses.
Avoid cigarettes and alcohol- Smoking and drinking can affect the circulation increasing the complications associated with neuropathy.
Healthy and balanced diet- Including lots of green vegetables, fresh fruits, lean meat and whole grains and ensuring an adequate supply of vitamins and minerals is essential.
Physical activity- Regular exercise can control neuropathic pain, improve muscle strength and help control blood sugar levels.