- Zaganjor I, Sekkarie A, Tsang BL, et al. Describing the Prevalence of Neural Tube Defects Worldwide: A Systematic Literature Review. Cruz-Martinez R, ed. PLoS ONE. 2016;11(4):e0151586 - (doi:10.1371/journal.pone.0151586.)
- Know About Neural tube defect - (https://en.wikipedia.org/wiki/Neural_tube_defect
#Anencephaly) - Werhagen L1, Hultling C, Borg K. Pain, especially neuropathic pain, in adults with spina bifida, and its relation to age, neurological level, completeness, gender and hydrocephalus. J Rehabil Med. 2010 Apr;42(4):374-6 - (doi:10.1371/journal.pone.0151586.)
- Neural tube defects - (http://www.marchofdimes.org/baby/neural-tube-defects.aspx)
- What are neural tube defects? - (https://www.nichd.nih.gov/health/topics/ntds/conditioninfo/Pages/default.aspx)
What are Birth Defects?
Birth defects, that is anomalies that are present at the birth of the baby, can be structural, functional or metabolic; they can be detected during pregnancy or at birth; they can cause physical or physiological problems; they can also be fatal in some circumstances.
Also known as congenital anomalies and congenital disorders, the most common birth defects are Down’s syndrome, neural tube defects and congenital heart defects.
- Structural birth defects are those that affect the development of body parts like the skeleton and certain organs. They usually develop during the first few weeks of pregnancy when the organs develop. The major ones can be identified at birth. Common structural birth defects are neural tube defects, congenital heart defects, orofacial defects and musculoskeletal defects.
- Functional or Developmental Birth Defects affect the functioning of a particular body part. They often lead to intellectual and developmental disability (IDD). They include Down’s syndrome, sensory problems, metabolic disorders and degenerative disorders.
The babies of women of all age groups, races, education levels and socio-economic backgrounds can get affected.
Educating people about the causes of birth defects along with vaccinations, fortification of foods with folic acid and iodine (especially in vegetarian and vegan pregnant women) and adequate antenatal care are some methods to prevent birth defects.
This article focuses only on neural tube defects, its diagnosis and treatment.
What are Neural Tube Defects?
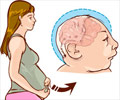
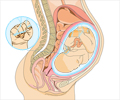
Neural tube defects (NTDs) refer to structural defects of the nervous system that occur during the developmental process. They are abnormalities that affect the brain, spine and spinal column of the developing embryo when the mother is still in the first month of pregnancy.
By about the first month of fetal life, the primitive structure that gives rise to the brain and spinal cord folds upon itself to give rise to a tube-like structure, the neural tube. The cells that form the neural tube in the developing embryo later on specialize to form the brain in the upper part and the spinal cord and the vertebral column in the remaining lower part. In some cases, the neural tube closure does not occur completely, giving rise to neural tube defects.
Neural tube defects are usually diagnosed before the infant is born, through blood or amniotic fluid tests, or imaging tests. There is no cure for neural tube defects. The nerve damage and loss of function that are present at birth are usually permanent. However, a variety of treatments can sometimes prevent further damage and help with complications.
What are the Types of Neural Tube Defects?
NTDs can be of two kinds - the common ‘open’ kind and the rarer ‘closed’ kind.
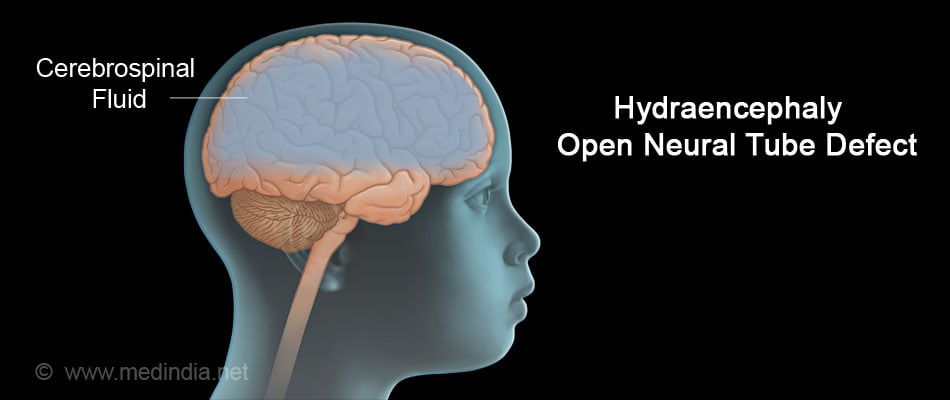
- When the brain and /or the spinal cord are exposed and seen out of the skull or the vertebrae, the defect is considered an open defect. Examples are spina bifida, anencephaly, encephaloceles, hydraencephaly, iniencephaly, and schizencephaly. Babies with open NTDs may suffer from meningitis.
- In the rarer closed form, the neural tissue is not exposed and the defect is covered by skin, which may show changes like a hairy or a light or dark colored patch. The spinal cord is tethered to the tissues of the back and the goal of treatment in this defect is to separate the two so that there is no stretching of the spinal cord as the child grows. Examples are lipomyelomeningocele and lipomeningocele, where a lump appears in the back, and tethered cord.
Among all the NTDs, spina bifida and anencephaly are the two most common forms.
Some of the neural tube defects are described below:
Spina Bifida:
When the closure defect is lower down in the neural tube, it gives rise to a condition commonly referred to as spina bifida. The bones of the vertebrae do not close completely, and a part of the spinal cord could poke out of the spine. There is usually nerve damage that causes at least some paralysis of the legs below the level of the defect and very poor control of their bowel and bladder habits.
Spina bifida affects around 1500 newborn babies in the United States every year. It is of different types; the severity of the condition depends on the extent of the defect. Some patients with less severe types of spina bifida may have normal intelligence, can be treated with surgery and may live for many years with mild disabilities.
The common types of spina bifida are:
- Spina bifida occulta whichis the mildest form where there is a small gap in the spine but the opening cannot be seen in the back. Brain and spinal cord functions are normal and there is no disability.
- Meningocele is a sac of fluid not involving the spinal cord that comes out through an opening in the back. The sac is lined by the meninges, the tissue that surrounds the brain and the spinal cord.
- Myelomeningocele is one of the most common and most severe form of spina bifida. The spinal cord and the tissues covering it protrude out of an opening in the back. Since it occurs because the bones of the vertebral column are not formed completely, the person has partial or complete paralysis in the regions below the affected part. Thus, movements of limbs, as well as bowel and bladder functions are affected. Children with this disorder can develop hydrocephalus, a condition where excessive fluid accumulates in the brain, which might cause mild-to-severe intellectual and learning disabilities.

Anencephaly:
When the closure failure occurs close to the upper end of the neural tube in the developing fetus, it gives rise to a condition called ‘anencephaly’ meaning ‘no brain’. It affects around 3 out of 10,000 pregnancies in the US.
The baby is born without the forebrain and may also lack a part of the skull with the brain and the associated structures lying exposed and highly disorganized. The affected babies are usually stillborn. Sometimes, they are born unconscious and lack the ability to hear, see and feel pain. Reflex actions like breathing and sensation of touch might be present. In such cases, death occurs within the first few days of birth.
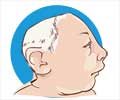
Encephalocele:
Encephalocele is a kind of neural tube defect that results in a sac-like protrusion of the brain and its surrounding membranes through an opening in the skull.
The opening occurs because the neural tube does not fold and close completely as expected during the third and fourth weeks of pregnancy to form the brain and the spinal cord.
The opening mostly occurs at a point through the center of the head in between the forehead and the nose, or at the base of the skull or the top of the head.
Other conditions like hydrocephalus, developmental and intellectual disabilities, structural abnormalities of the head, face and skull, paralysis of upper and lower limbs, and neurological problems like seizures and uncontrolled movements may occur. Some children may have normal intelligence.
This condition occurs in 1 in 12,200 babies born every year in the US.

Iniencephaly:
Rare but severe, this neural tube defect manifests itself as a severe bending of the infant’s head backward. Other associated features are distortion of the spine and lack of a neck, with the skin of the face connected to the chest and that of the scalp connected to the back. Other defects that may also be seen are cleft lip and palate, and cardiovascular and intestinal malformations. Infants survive only for a few hours after birth.
What are the Causes and Risk Factors of NTDs?
Genetic factors alone or in combination with the mother’s exposure to certain environmental factors including the consumption of certain foods and medicines during pregnancy have been linked to bearing children with NTDs.
Deficiency in folic acid has been linked to NTDs. NTDs are preventable if a woman of child-bearing age takes 400 micrograms of folic acid (or more if their first pregnancy was affected with spina bifida) before and during the first few months of pregnancy. Folic acid is a B vitamin that is vital for the growth and development of the nervous system of the fetus.
The risk of NTDs also increases with other factors like excessive weight, uncontrolled diabetes, and intake of anti-seizure medicines.
How do you Detect Neural Tube Defects?
Neural tube defects are usually diagnosed through prenatal tests that are done before the infant is born. These include laboratory or imaging tests like blood tests, ultrasound and amniocentesis.
If there is positive history of a previous child with a neural tube defect, there is a greater possibility of the disorder occurring in subsequent child.
Screening tests:
These tests are routine tests to check for any abnormalities in the baby.
- A maternal serum screen is a simple blood test that tests the blood of the pregnant woman for neural tube and other defects during the second trimester (between the 15th and the 20th week of pregnancy). Depending on the number of proteins tested, it could also be called a “triple screen” (that tests for á-fetoprotein, hCG and estriol) or a “quad screen” (that tests the levels of á-fetoprotein, hCG, estriol, and inhibin-A).
- High levels of á-fetoprotein are associated with a higher risk of NTDs. Alpha-fetoprotein or á-fetoprotein or AFP is a chemical that is produced in the fetal liver but its function is unknown. It could be the fetal form of serum albumin.
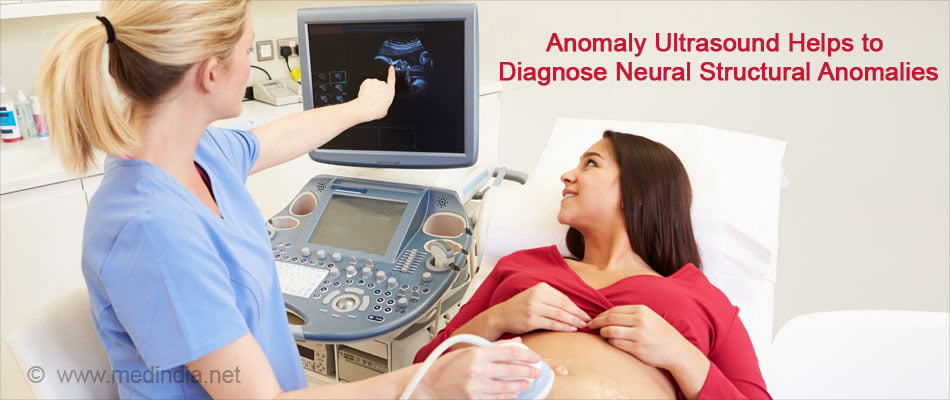
- An anomaly ultrasound done between the 15th and the 20th week of pregnancy is comprehensive and checks for structural anomalies including physical defects of the brain and spine, and the size of the baby.
Diagnostic Tests:
These tests are suggested when there are elevated levels of á-fetoprotein or other abnormal results that showed up on the screening tests. These might confirm the possible diagnosis of an NTD.
1. Amniocentesis: Done between the 15th and the 18th week of pregnancy, amniocentesis is done if the initial screening tests showed elevated á-fetoprotein levels. A sample of the amniotic fluid is taken for the analysis and is tested for the the presence of á-fetoprotein and acetylcholinesterase or AChe.
Small amounts of á-fetoprotein is present in the amniotic fluid of normal fetuses. Higher than normal levels in the amniotic fluid indicates an opening in the neural tissue, such as a neural tube defect (spina bifida or anencephaly).
However, a high level of á-fetoprotein does not always mean that the fetus is defective, because other reasons could be responsible for the same.
High levels of AChe in the amniotic fluid sample indicates an opening in the neural tube.
The amniotic fluid is also tested for chromosomal abnormalities since they too can cause –congenital defects.
2. A level 2 ultrasound done between the 18th and the 22nd week of pregnancy will help look for any birth defect signs that were indicated in the screening tests.
Once the baby is born, the doctor can check for suspected neural tube defect through a detailed neurological examination and using tests like x-rays, magnetic resonance imaging and computed tomography.
How are NTDs Treated?
There is no cure for neural tube defects.
Spina Bifida:
Treatment depends on the type and severity of spina bifida.
Most children with mild form of the disorder need no treatment, although some may require surgery as they grow. This prevents further damage to the nervous tissues and protects them against infections. The spinal cord and its nerve roots are put back into the spine and sealed up.
Some children with spina bifida need assistive devices (like braces, crutches, or wheelchairs) depending on the location of the malformation in the spine.
Anencephaly:
There is no cure for children with anencephaly. Children born with this condition are usually stillborn or die shortly after birth.
Encephalocele:
Treatment involves surgically placing the protruding part of the brain along with its membranes back inside the skull and closing the opening. Neurological problems will persist.
Depending on the child’s condition, the location of the opening and the affected parts of the head and face, long-term treatment or surgeries might be needed.
Babies who develop hydrocephalus may need a shunt to divert excess fluid from the brain.