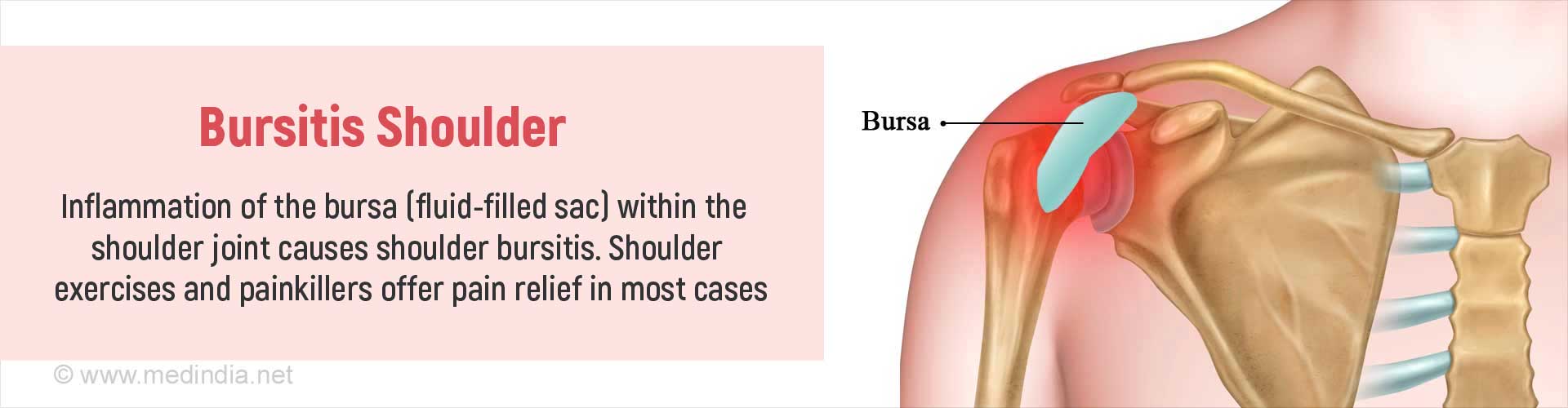
How do you Diagnose Bursitis Shoulder?
Diagnosis involves taking a clinical history, physical examination and analyzing the results of medical imaging.
When you visit the doctor to complain about shoulder pain, your shoulder will be carefully examined and your medical history will be taken. The doctor will get a sense of the cause of the pain based on the events that occur in your life, for example, a fall or any kind of accident or other injury.
Physical examination: It is important to examine the neck and shoulder to test the strength of the neck and the related muscles. Shoulder rotation is also examined with different tests (e.g. lift-off test). For an accurate diagnosis, a combination of tests is recommended. In general, a combination of Neer’s test and Hawkins-Kennedy test provides a reasonably accurate diagnosis of shoulder impingement. A painful shoulder arc test is another diagnostic test. To exclude other conditions that exhibit similar symptoms as shoulder impingement, the apprehension test and O’Brien’s test are used. (For test procedure kindly refer glossary).
Imaging tests: The results of imaging tests should be used in conjunction with the clinical history and the results from the physical examination tests.
Ultrasonography: An ultrasound scan (USS) shows a high degree of diagnostic accuracy in detecting shoulder impingement.
Magnetic resonance imaging (MRI): This imaging test is equally accurate as USS in diagnosing shoulder impingement. The sensitivity and specificity of the technique is nearly 90%. Magnetic resonance arthrogram (MRA) is an invasive test that is diagnostically accurate. However, it can be avoided due to its invasiveness.
How do you Treat Bursitis Shoulder?
Bursitis shoulder is treated with appropriate exercises (physiotherapy), corticosteroid injections, and nonsteroidal anti-inflammatory drugs (NSAIDs). Surgery is recommended when all the other treatment options fail.
Physiotherapy: Physical therapy has shown to be beneficial in reducing the pain associated with shoulder pain. However, physiotherapy does not improve the strength of shoulder muscles.
Corticosteroid injections: Combined treatment of corticosteroid injections along with physiotherapy has shown to greatly improve shoulder pain. In most cases, surgery is not required after 2 years since the pain is resolved, though, in some of these cases, there is some residual pain.
Orthobiologics: Biological substances that help to repair injured muscle and skeletal tissue, e.g. hyaluronic acid (HA), platelet-rich plasma (PRP), and growth factors, have shown some benefits in shoulder pain.
Nonsteroidal anti-inflammatory drugs (NSAIDs): Oral NSAIDs such as naproxen, celecoxib are prescribed initially to temporarily relieve the intense pain but they are not a cure for the pain.
Surgery: As mentioned above, surgery is the last treatment option after all other treatments fail to improve the pain in the shoulder. Acromioplasty, arthroscopic subacromial decompression (ASAD), and bursectomy are some of the surgical techniques used to repair rotator cuff muscles in the shoulder. While most people show a favourable resolution of their pain, there are some who continue to have residual pain despite the surgery.
The general recovery rate for acute cases ranges from half a year to a year. Chronic cases take almost one and a half years to recover. However, there is a small percentage of cases that still suffer from residual pain.
How to Prevent Bursitis Shoulder?
Based on the causes, some caution can be exercised in certain cases, for example:
- Avoid actions where you have to stretch out your hand overhead.
- Maintain a good posture when performing different activities
- A good warm up helps before beginning any sports activity and always take regular breaks.
- Begin practising new sports at a slow pace before increasing the strain on the body. You should immediately stop when you experience any pain.
- Use knee and/or elbow pads to avoid irritation to the affected area.