- What Is Breast Cancer? - (https://www.cancer.org/cancer/breast-cancer/about/what-is-breast-cancer.html)
- Breast Cancer Facts - (https://www.nationalbreastcancer.org/breast-cancer-facts)
- Breast Anatomy - (https://www.nationalbreastcancer.org/breast-anatomy)
- Breast Cancer Risk Factors - (https://www.breastcancer.org/risk/factors)
- What Are the Symptoms of Breast Cancer? - (https://www.cdc.gov/cancer/breast/basic_info/symptoms.htm)
- Breast Cancer Symptoms: What You Need to Know - (https://www.cancer.org/latest-news/breast-cancer-symptoms-what-you-need-to-know.html)
- Breast Cancer Screening and Diagnosis - (https://www2.tri-kobe.org/nccn/guideline/breast/english/breast-screening.pdf)
- TNM Staging - Breast Cancer - (https://www.cancerresearchuk.org/about-cancer/breast-cancer/stages-types-grades/tnm-staging)
- Breast Cancer Treatment - (https://www.cancer.gov/types/breast/patient/breast-treatment-pdq)
- Various Types and Management of Breast Cancer: An Overview - (https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3255438/)
- 8 Ways to Prevent Breast Cancer - (https://siteman.wustl.edu/prevention/take-proactive-control/8-ways-to-prevent-breast-cancer/)
What is Breast Cancer?
Breast cancer is a cancer that affects the breasts or mammary glands. Early detection and lifestyle changes help in controlling breast cancer.
On a global scale breast cancer is the most common cancer amongst women. According to estimates, in 2004 alone breast cancer caused 519,000 deaths worldwide.
It is the second most commonly occurring cancer after lung cancer and is the fifth most common cause of
Breast cancer incidence increases with age; the older the woman, the more aggressive the evaluation techniques employed. Nevertheless, younger women with Breast lumps are at a far greater risk for breast cancer in comparison to asymptomatic women of the same age group, and to older women.(1✔ ✔Trusted Source
What Is Breast Cancer?
Go to source)
Breast cancer mostly occurs in women over the age of 50, and the risk is especially high for women over age 60.
Contrary to popular belief that it is a woman’s affliction, it can affect both men and women.
A combination of environmental factors and genes are responsible for this cancer. In familial breast cancers, a mutation in the genes BRCA1 and BRCA2 play a major role in the disease onset.
Breast cancer can be inherited from either a female or a male relative who may have had the disease or who acts as a carrier of the mutant gene(s).
Breast cancer incidence varies vastly worldwide. It is significantly higher in the developed countries of the world in comparison to the less-developed ones. There has been a surge in the number of affected individuals since the 1970s and experts are of the opinion that the indulgent lifestyles of the western world could be largely responsible.
Breast cancer is also found to occur more often in white women than African American or Asian women. Several studies have revealed that the breast cancer scenario in the US is quite different for a black woman in comparison to her white counterpart. The former is more likely to die from the disease although it is the latter who is more frequently diagnosed with the disease. The experts say it is a reflection of the socio-economic and cultural disparity that exists among the races and that it is highly likely that the black woman has less access to screening and treatment facilities.
Breast lumps need to be taken seriously because the vast majority of breast cancers are detected as palpable lesions sometimes by the clinician during a regular check or by the patient herself. It can also present as non-palpable lesions during a routine mammography. It must be noted that the palpable lesions are assessed quite differently from the non-palpable lesions.
Breast cancer is one of the oldest cancers known to man. However, it is only with the modern understanding of the systemic nature of the disease that has given rise to effective treatments.
A pink ribbon denotes the struggle of the sufferers when fighting the cancer. In 1996 the pink and blue ribbon were designed to create awareness of the fact that "Men Get Breast Cancer Too!”
Facts on Breast Cancer
- In 2012, nearly 1.7 million new cases were diagnosed worldwide, making it the second most common cancer overall
- Breast cancer is 100 times more frequent in women in comparison to men. Prognosis is the same in both
- It is also the most common cancer in women - the incidence rate among females is twice as much as that of colorectal cancer and cervical cancer and approximately three times that of lung cancer
- Globally, the incidence of breast cancer is highest among American women
- 16% of women between the age of 40-60 years have breast-related problems. Of these 40% complain of breast lumps
- In women over 40 years, these breast lumps may carry a risk of breast cancer
- However, the majority of breast-related complaints may be due to benign breast disease(2✔ ✔Trusted Source
Breast Cancer Facts
Go to source)
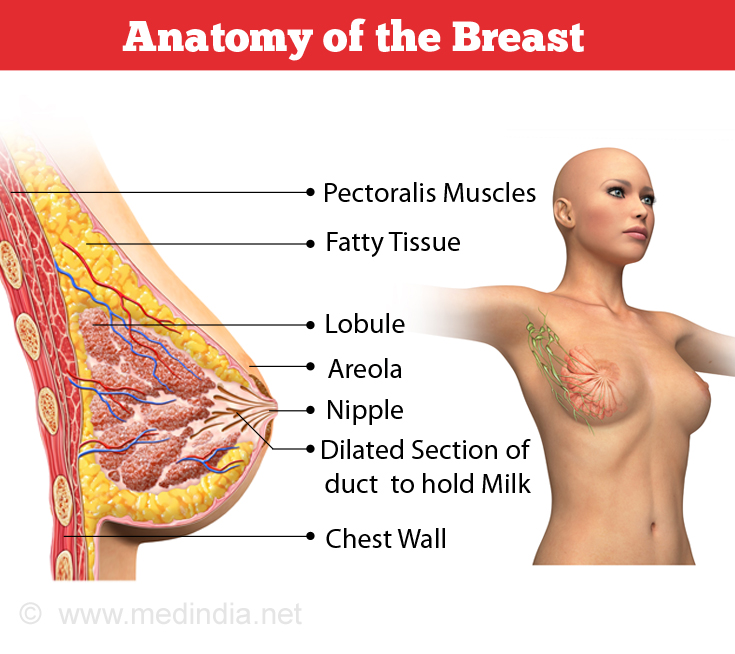
Breast Anatomy
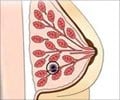
Each breast has 15 to 20 sections called lobes. Within each lobe are many smaller lobules (milk-producing glands). Lobules end in dozens of tiny bulbs that can produce milk. The lobes, lobules and bulbs are all linked by thin tubes called ducts (milk passages that connect the lobules and the nipple). Fat surrounds the lobules and ducts. These ducts lead to the nipple in the center of a dark area of skin called the areola. There are no muscles in the breast, but muscles lie under each breast and cover the ribs.
Each breast also contains blood vessels and lymph vessels. The lymph vessels carry colorless fluid called lymph, and lead to small bean-shaped organs called lymph nodes. Clusters of lymph nodes are found near the breast in the axilla (under the arm), above the collarbone, and in the chest. Lymph nodes are also found in many other parts of the body.
Cancer cells may enter lymph vessels and spread out along these vessels to reach lymph nodes. Cancer cells may also enter blood vessels and spread through the blood stream to other parts of the body, bypassing lymph nodes. When breast cancer cells reach the lymph nodes, they continue to grow, often causing swelling of the lymph nodes. These swollen lymph nodes sometimes can be felt, especially in the armpit. If breast cancer cells have spread to the lymph nodes in the armpit, there is a greater chance that cancer cells have spread to other organs of the body as well.(3✔ ✔Trusted Source
Breast Anatomy
Go to source)
What are the Causes and Risk Factors of Breast Cancer?
Breast cancer, like other forms of cancer, is considered to be the final outcome of a legion of environmental and hereditary factors. However, the exact cause is not known. It is suspected that more than one factor is involved. Also the risk of breast cancer increases as a woman gets older.
- Personal history of breast cancer: Women who have had breast cancer face an increased risk of getting breast cancer in their other breast
- Family history: A woman's risk of developing breast cancer increases if her mother, sister, or daughter had breast cancer, especially at a young age
- Late childbearing: Women who have their first child late (after about age 30) have a greater chance of developing breast cancer than women who have had a child at a younger age
- Early menstruation and late menopause: Women who started their menstrual periods early (before age 12) or go through menopause late (after age 55) are at a higher risk
- Breast density: Breasts that have a high proportion of lobular and ductal tissue appear dense on mammograms making it more difficult for doctors to see abnormal areas on a mammogram. Breast cancers nearly always develop in lobular or ductal tissue (not fatty tissue). That's why cancer is more likely to occur in breasts that have more lobular and ductal tissue (that is, dense tissue) than in breasts with more fatty tissue
- Obesity is a controversial risk factor: Some studies report obese individuals have a higher risk of breast cancer, possibly associated with higher levels of estrogen production in them
- Radiation therapy: Women whose breasts were exposed to radiation before age 30, especially those who were treated with radiation for Hodgkin's disease, are at an increased risk of developing breast cancer. Studies show that the younger a woman is, while receiving radiation treatment, the higher her risk for developing breast cancer later in life
- Factors such as ionizing radiations and viruses are believed to play a major role in bringing about these mutations
- Alcohol: Some studies suggest a slightly higher risk of breast cancer among women who drink alcohol (more than 3 drinks a day)
- Oral contraceptives (birth control pills): Birth control pills may slightly increase the risk for breast cancer, depending on age, length of use, and other factors
- Hormone replacement therapy: Undergoing HRT for more than 5 years added with longer periods of usage has been shown to slightly increase the risk of breast cancer
- Estrogen pills: Women consuming diethylstilbestrol (DES) to prevent miscarriage may have an increased risk of breast cancer
- Chemicals: Some studies have pointed to exposure to estrogen-like chemicals that are found in pesticides and other industrial products as a possible increased risk of breast cancer
- Gene mutations are believed to play a vital role in causing breast cancer. Mutations in the tumor suppressor genes (TSG) BRCA 1 and BRCA2 are implicated in 95% of familial breast cancers. These mutations increase a person’s risk of developing breast and/or ovarian cancer diet high in saturated fat by 30-40%
- Another TSG, p53, is also implicated in breast cancer
- Abnormal growth factors and faulty immune surveillance are also known to cause breast cancer
- Environmental / lifestyle factors implicated are:
- a diet high in saturated fat alcohol intake and dairy products
- obesity
- alcohol intake / tobacco usage
- change in workshift patterns(4✔ ✔Trusted Source
Breast Cancer Risk Factors
Go to source)

What are the Signs and Symptoms of Breast Cancer?
Detection of a breast lump Lumps in the armpits that feels different from the surrounding tissue could often be the first sign of breast cancer.
But, almost 90% of all breast masses are caused by benign lesions (non-cancerous) and not due to malignancy.
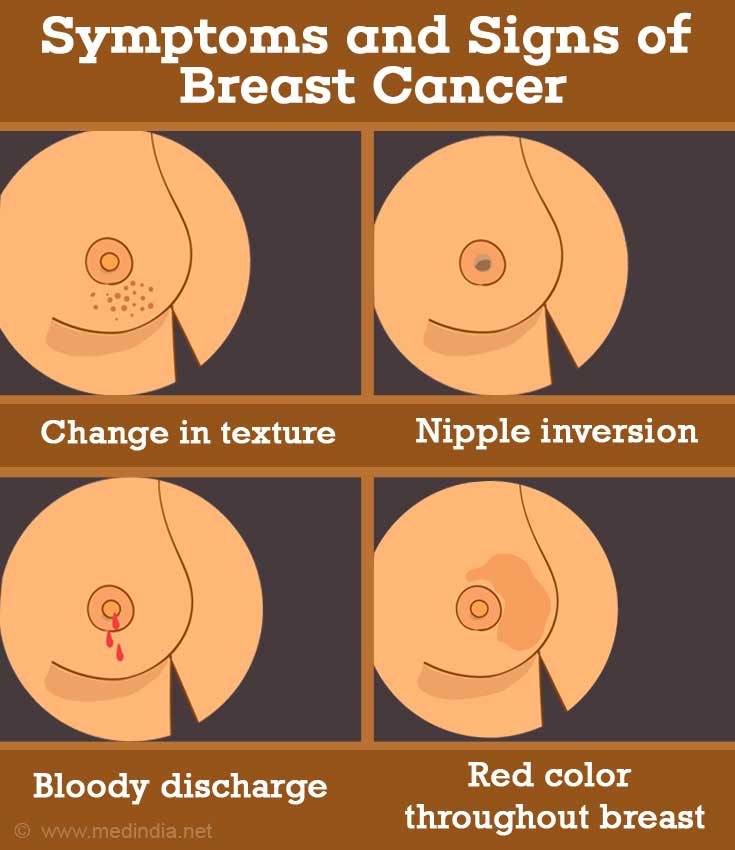
Some of the other symptoms of breast cancer include:
- Lumps in the armpits/collar bone
- Change in texture of the breast skin such as redness, dimpling, crusting or puckering
- Change in size / shape of breast
- Nipple inversion
- Bloody discharge (unilateral) from the nipple
Paget’s disease of the breast
Pain is not a reliable symptom as it could also indicate other health conditions.(5✔ ✔Trusted Source
What Are the Symptoms of Breast Cancer?
Go to source)
Inflammatory breast cancer (IBC) is a rare and aggressive form of breast cancer. Symptoms of inflammatory breast cancer include:
- Pain
- Swelling
- Warm feeling
- Red color throughout breast
- Orange-peel texture of the skin on the breasts (peau d'orange)(6✔ ✔Trusted Source
Breast Cancer Symptoms: What You Need to Know
Go to source)
Sometimes the disease is metastatic and would spread across to other parts of the body such as bone, brain, liver, lung and brain via the lymphatic system or blood vessels. The symptoms would then include:
- Weight loss
- Chills / fever
- Joint / bone pain
Metastasis mostly involves bones, especially the vertebrae and the long bones of the ribs, arms and legs. When cancer spreads to the bones, it eats its way into the healthy bones to cause weak spots where the bones can easily break. Hence aching or weak bones are common in breast cancer patients and it is common for many of them to use a wheel chair.
Many of the symptoms of breast cancer are non-specific and can also present in other breast diseases such as fibroadenoma, mastitis and benign breast disease.
High-Risk Groups
Breast cancer patients are categorized into various groups depending on their risk status.
Highest Risk (RR>4)
- Older patients who are North Americans
- Two first degree relatives with breast cancer at an early age
- History of cancer in one breast
Intermediate risk (RR 2.1-4.0)
- Nodular densities seen in a mammogram that occupy 75% of breast volume
- One first degree relative with breast cancer
- Atypical hyperplasia on breast biopsy
- High dose radiation to chest
Increased risk (RR 1.1-2.0)
- Urban residence
- First pregnancy after age 30
- Menarche at age < 12 years / menopause at age > 53
- Obesity
- Nulliparous – female who has not borne an offspring
- Use of hormonal contraceptives / HRT
- History of primary endometrial, ovarian and colonic cancer
- Use of alcohol
What is the Diagnosis for Breast Cancer?
- Clinical breast exam: A thorough clinical exam can reveal any lumps, if formed. A self breast examination can also be done on a regular basis
- Mammograms: A low radiation X-ray called screening mammogram is the best tool available for detecting breast cancer early, before symptoms appear. Mammograms can often detect a breast lump before it can be felt. It also shows small deposits of calcium in the breast. Although most calcium deposits are benign, a cluster of very specks of calcium (called microcalcifications) may be an early sign of cancer
- Ultrasonography: Using high-frequency sound waves, ultrasonography can often show whether a lump is a fluid-filled cyst (not cancer) or a solid mass (which may or may not be cancer)
- Magnetic Resonance Imaging (MRI): MRI is used to define the size and extent of cancer within the breast tissue. It is mostly used in women whose dense breast tissue makes it more difficult to find tumors with a mammogram
- Digital Mammography: Digital mammography is similar to standard mammography and it uses radiographs to image the breast. The advantage of digital mammography is that images are stored digitally and can be enhanced by modifying the brightness or contrast. These images can be transmitted by telephone lines for remote consultation
- Biopsy: This procedure takes a tissue sample to be examined under the microscope
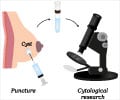
- Fine needle aspiration cytology (FNAC): A thin needle is used to remove fluid and/or cells from a breast lump. If the fluid is clear, it may not need to be checked by a lab
- Needle biopsy: Using special techniques, tissue can be removed with a needle from an area that looks suspicious on a mammogram but cannot be felt. Tissue removed in a needle biopsy goes to a lab to be checked by a pathologist for cancer cells
- Stereotactic needle biopsy: This procedure uses a mammogram-directed technique using computerized mammogram breast images which helps to map the exact location of the breast lump
- Surgical biopsy: In an incisional biopsy, the surgeon cuts out a sample of a lump or suspicious area. In an excisional biopsy, the surgeon removes all of a lump or suspicious area and an area of healthy tissue around the edges. A pathologist then examines the tissue under a microscope to check for cancer cells
- In February 2007 the FDA formally approved the Mamma Print test that has the ability to predict breast cancer recurrence in women with early-stage breast cancer. This determines how aggressively the initial tumor needs to be treated.
The accuracy of diagnosis is said to reach 100% if the results from clinical examination, mammography and FNAC are combined. This is known as the triple diagnosis method or the “Triple Test”.(7✔ ✔Trusted Source
Breast Cancer Screening and Diagnosis
Go to source)
What is the Staging / Classification for Breast Cancer?
Today the accepted staging for breast cancer is the TNM classification which takes into consideration the tumor itself, the involvement of the lymph nodes and the metastasis to other body parts. The mode of treatment best suited for each patient and the prognosis is closely linked to the stage of the tumor.
- STAGE 0: In Situ ("in place") disease in which the cancerous cells are in their original location within normal breast tissue
- STAGE I: Tumor that is less than 2 cm in diameter with no spread beyond the breast
- STAGE II: Tumor that is 2 to 5 cm in size without spread to lymph nodes of axilla or tumor less than 2 cm in size with spread to axillary lymph nodes
- STAGE III: Tumor that is smaller than 5 cm in size with spread to axillary lymph nodes which are attached to each other or other structures
- STAGE IV: A tumor that is of any size, with spread beyond the region of the breast and chest wall, such as to liver, bone, or lungs
Each tumor is classified histologically into the following:
- Well-differentiated tumors (low grade) - resembles normal tissue
- Poorly differentiated tumors (high grade) - composed of disorganized cells, does not resemble normal tissue
- Moderately differentiated tumors (intermediate grade) – has characteristics that resemble both of the above(8✔ ✔Trusted Source
TNM Staging - Breast Cancer
Go to source)
What is the Treatment for Breast Cancer?
There are three paths that can be followed after the triple diagnosis.
- Women in whom the triple diagnosis suggests benign disease are closely monitored (physical exam every 3 to 6 months for at least a year) to ensure that the breast mass is stable
- Women in whom the diagnosis suggest malignancy are referred for treatment
- Women in whom any one of the triple tests suggests malignancy need to undergo excisional biopsy
The choice of treatment is based upon many factors that depend upon the extent to which the cancer has spread, characteristics of the cancer, and the general health of the patient.
The treatment of breast cancer involves local and systematic treatment. Treatment to the whole body involves systematic treatment, and local treatment involves treatment of breast area and the lymph nodes near it. Sometimes treatment may include more than one type of local or systematic treatment. Both systematic and local treatment is given in patients where the cancer has spread to other places beyond the breast.
Surgery
The main mode of treatment for breast cancer is surgery, especially so, when the tumor is localized.
As mentioned earlier, breast cancer is thought of as a cancer that affects the breast. It must be noted that this cancer can spread to other body parts via the lymphatic system, which is why breast cancer treatment almost always involves surgery for the underarm glands that may involve either axillary clearance, sampling, or sentinel node biopsy.
There are several types of surgery.
- Breast-conserving surgery: An operation to remove the cancer but not the breast is called breast-sparing surgery
- Lumpectomy: In lumpectomy, the surgeon removes the breast cancer and some normal tissue around it
- Segmental mastectomy: In segmental mastectomy, the surgeon removes the cancer and a larger area of normal breast tissue around it. Occasionally, some of the lining over the chest muscles below the tumor is removed as well. Some lymph nodes under the arm may also be removed
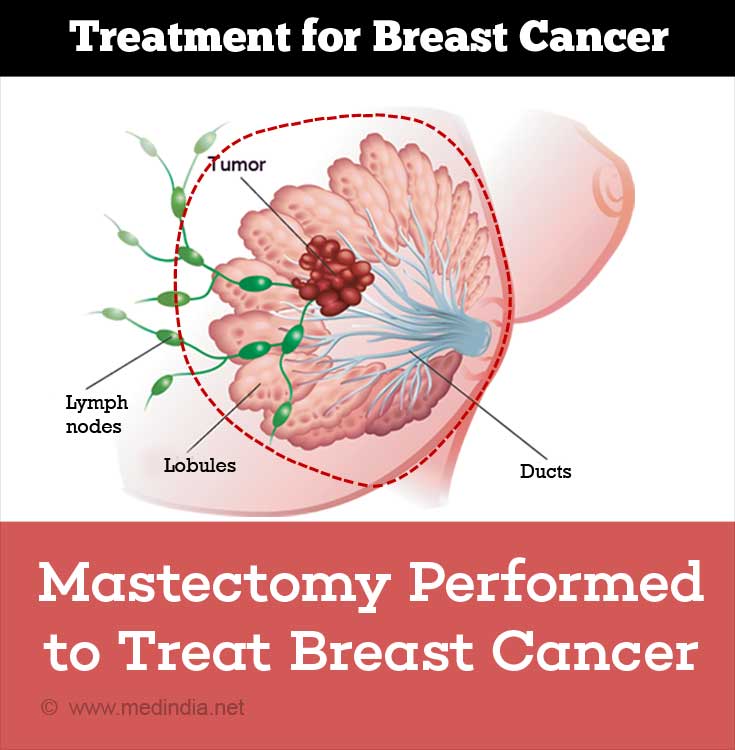
- Total mastectomy: In total mastectomy, the surgeon removes the whole breast. Some lymph nodes under the arm may also be removed
- Radical mastectomy: The surgeon removes the breast, both chest muscles, all of the lymph nodes under the arm, and some additional fat and skin. For many years, this operation was considered the standard one for women with breast cancer, but it is almost never used today. In rare cases, radical mastectomy may be suggested if the cancer has spread to the chest muscles
- Axillary lymph node dissection: Removing some or all of the lymph nodes in the armpit. Usually 10 to 20 lymph nodes in the arm pit are removed
Surgery is often followed up with any of the following treatments depending upon the patient’s risk status - low or high-risk. Age, type of cancer, size and metastasis of the disease decides the risk status of the patient.
Other treatment possibilities include chemotherapy, radiation therapy, hormone therapy, and immune therapy.
1) Chemotherapy is carried out in those who have undergone surgery. Chemotherapy can also be used as a primary treatment option once cancer cells are diagnosed in the body's circulation or to keep the cancer from spreading.
It is the use of drugs to kill cancer cells. Chemotherapy for breast cancer is usually a combination of drugs. Even in the primary stage of the disease the cancer cells can break away from the original site and metastasize to other areas as well. These cells may not be detected during imaging studies or physical exams. When left untreated, these cells have the potential to grow into malignant tumors. The aim of adjuvant chemotherapy is to kill these potentially dangerous, undetected cancer cells.
The drugs may be given as a pill or by injection. Either way, the drugs enter the bloodstream and travel throughout the body. Chemotherapy is preferred when the cancer is spread to the lymph nodes; that is when the cancer growth is more than a centimeter. Chemotherapy is not preferred for cancers with a low risk of spreading to other parts. Side effects of chemotherapy are nausea, vomiting, diarrhea, mouth sores, tiredness, susceptibility to infection, hair loss, aches and other discomforts.
Some of the drug combinations used in the treatment are:
- Cyclophosphamide methotrexate and 5-fluorouracil
- Cyclophosphamide, doxorubicin and 5-fluorouracil
- Doxorubicin and cyclophosphamide
- Epirubicin and cyclophosphamide
- Docetaxel, doxorubicin, and cyclophosphamide
Other chemotherapy drugs used in the treatment of women with breast cancer include carboplatin (Paraplatin), cisplatin (Platinol), vinorelbine (Navelbine) and capecitabine (Xeloda).
When breast cancer has spread to the bones, it can be treated but not cured. Drugs like Alpharadin (radium 223) are being developed to combat bone metastasis. This drug works by reducing estrogen levels, as estrogen provides the ambience for the tumors to grow. Clinical trial - phase II studies for this drug have shown good pain control and improved life quality.
Chemotherapy might not cure the cancer all together, but it can keep the cancer "in remission" for a period of time. Also, chemotherapy is used to prevent symptoms from occurring and is used to help one feel more "comfortable" although the cancer may still be in progress.
2) Interstitial laser therapy is a non-surgical, minimally invasive, innovative method of treating breast cancer employing laser for treatment. There are no adverse reports recorded for this procedure.
3) Radiotherapy is also used to kill malignant cells that have escaped surgery. Radiation, when applied correctly, can reduce the risk of recurrence by 50-66%.
- External radiation: Radiation may be directed at the breast by a machine
- Implant radiation: Radiation can also come from radioactive material placed in thin plastic tubes that are placed directly in the breast. Some women have both kinds of radiation therapy
There are three main kinds of systematic treatments used for the whole body.
- Hormonal therapy: Estrogen is a hormone that is required for cancer cells to grow. Estrogen binds to these cells and stimulates them to grow and divide. Anti-estrogens prevent the binding of estrogen. This stops the cells from growing and in doing so, prevents or delays breast cancer recurrence. Tamoxifen is the most commonly used Selective Estrogen Receptor Modulators (SERMs). You should take the drug as a pill once a day. Side effects of this therapy can be hot flashes, vaginal dryness or discharge, irregular periods, nausea and cataracts. Serious, but rare, side effects are endometrial cancer, and blood clots in the lung or brain
- Immune therapy: This treatment enhances the immune system of the body to fight cancer cells. Herceptin is the most commonly used immune treatment for advanced breast cancer. Herceptin works by attaching to HER 2 receptors on breast cancer cells. These receptors are involved in the signaling for growth and spread of cancer cells. Herceptin blocks and masks the HER 2 receptors which help in recognition of these cells for the immune system to detect and destroy them
- Biological therapy: is a treatment designed to enhance the body's natural defenses against cancer(9✔ ✔Trusted Source
Breast Cancer Treatment
Go to source, 10✔ ✔Trusted Source
Various Types and Management of Breast Cancer: An Overview
Go to source)
What is the Prognosis for Breast Cancer?
Breast cancer prognosis in a patient is determined by several factors such as staging, tumor size, its location, grade, metastasis, recurrence, and age of the patient.
Of these, staging is the most decisive factor, as it takes into consideration the size of the tumor, lymph node status, local involvement and the metastatic nature of the disease. The greater the stage at diagnosis, the poorer is the prognosis.
Younger women tend to have a poorer prognosis in comparison to post-menopausal women as they are usually at a far advanced stage when diagnosed. This may be due to several factors such as nursing or a normal menstrual cycle, which causes them to be ignorant of the changes associated with their breasts.
The presence of certain markers such as estrogen and progesterone receptors in the cancer cells act as indicators that predict the response of the patient to treatment. Those who test negative for these receptors are known not to respond to hormone therapy.
Likewise, HER2/neu positive patients have a more aggressive form of disease that may respond well to trastuzumab, a monoclonal antibody.
The presence of elevated levels of alkaline phosphatase and the tumor marker CA 15-3 indicate early recurrence.
How to Prevent Breast Cancer?
There are some methods that can be used as measures to prevent the development of breast cancer. In general, leading a healthy lifestyle will help in some way to prevent breast cancer.
- Breast self exam may not be a very specific method for diagnosing breast cancer but it would familiarize you with your breasts and could well be the first step towards detecting changes in them. Ask your doctor to tell you how a breast exam is done. It is good to do regular selfbreast examinations after the age of 30
- It should be mandatory for women above the age of 40 to undergo breast cancer screening, as this would enable early detection. Regular check up by a health professional between ages 20 and 39 should be done at least every 3 years; women above the age of 40 should have a check up by a health professional every year. If there is a strong family history of breast cancer, one should have a regular mammogram after the age of 35.
- Avoid alcohol and if that is not possible drink in moderation
- Exercise everyday for at least 1 hour
- Limit the use of Hormone Replacement Therapy (HRT) drugs as far as possible as they increase the risk of breast cancer. Find out more about these drugs including their pros and cons from your doctor. Control weight gain as obesity is a high-risk factor
- For those in the high-risk category, preventive (estrogen–blocking) medications and preventive mastectomy are sensible options(11✔ ✔Trusted Source
8 Ways to Prevent Breast Cancer
Go to source)

Many risk factors cannot be controlled. Some experts in the field of diet and cancer agree that changes in diet and lifestyle may reduce the incidence of cancer generally. Efforts have focused on early detection since breast cancer is more easily treated and often curable if it is found early.