- Meningitis Symptoms and Causes - (http://www.mayoclinic.org/diseases-conditions/meningitis/symptoms-causes/dxc-20169522)
- Van de Beek D et al. Clinical features and prognostic factors in adults with bacterial meningitis. N Engl J Med. 2004;351:1849-1859. - (https://www.cdc.gov/meningitis/bacterial.html)
- Bacterial Meningitis - (https://www.cdc.gov/meningitis/bacterial.html)
- Scheld WM et al. Pathophysiology of bacterial meningitis: mechanism(s) of neuronal injury. J Infect Dis. 2002;186(S2):S225-S233. - (https://www.cdc.gov/meningitis/bacterial.html)
- Van de Beek D et al. ESCMID guideline: diagnosis and treatment of acute bacterial meningitis. Clin Microbiol Infect. 2016;Ie1-Ie26. - (https://www.cdc.gov/meningitis/bacterial.html)
- Hoffman O, Weber RJ. Pathophysiology and Treatment of Bacterial Meningitis. Therapeutic Advances in Neurological Disorders. 2009;2(6):1-7 - (doi:10.1177/1756285609337975.)
- Brouwer MC, Tunkel AR, van de Beek D. Epidemiology, diagnosis, and antimicrobial treatment of acute bacterial meningitis. Clin Microb Rev. 2010;23(3):467-492. - (doi:10.1177/1756285609337975.)
- Tunkel AR et al. Practice guidelines for the management of bacterial meningitis. Clin Infect Dis. 2004;39(9):1267-1284. - (doi:10.1177/1756285609337975.)
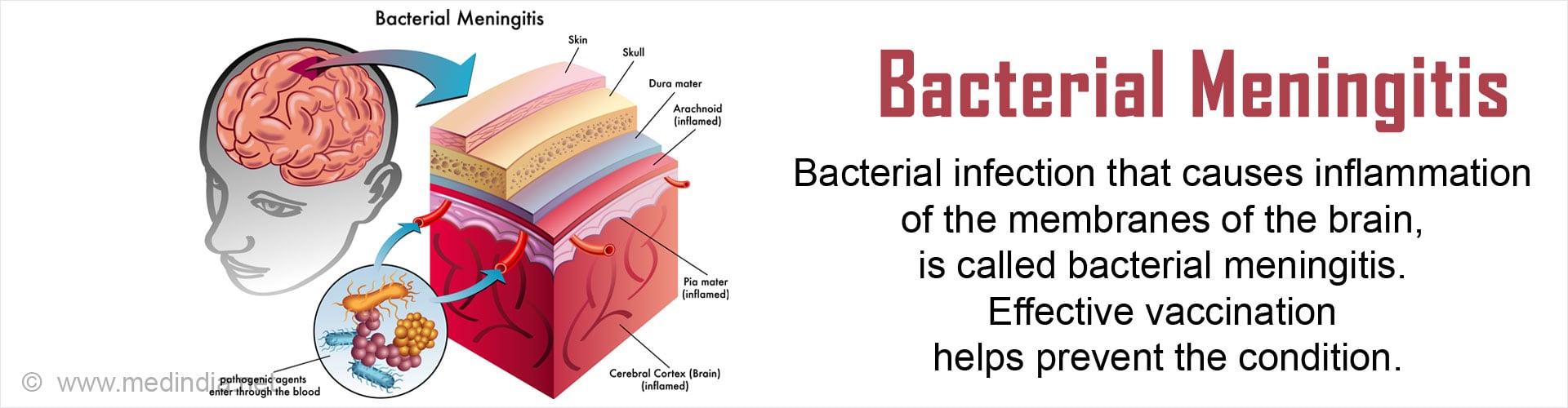
What is Meningitis?
The meninges are the membranes covering the spinal cord and the brain. When the meninges become swollen or inflamed, it results in meningitis.
Bacterial meningitis occurs in infants, children, and adults. Fever, stiffness of the neck, headache, and changes in mental capacity are the main symptoms.
What is Bacterial Meningitis?
In 1806, Vieusseux identified the organism causing the almost fatal condition of meningococcal meningitis. Bacterial meningitis is a bacterial infection of the meninges, resulting in swelling within the central nervous system (CNS).
An individual can die in as little as a few hours. However, most cases recover although they may be left with long-lasting handicaps, such as hearing impairment, learning difficulties, and damage to the brain.
What are the Causes of Bacterial Meningitis?
The etiology varies according to the age of the patient.
In newborn infants, bacterial meningitis is caused most often by:
- Escherichia coli
- Streptococcus agalactiae (group B Streptococcus)
- Streptococcus pneumoniae (by chance)
In children, bacterial meningitis results from:
- Streptococcus pneumoniae
- Neisseria meningitides
- Haemophilus influenzae (only in non-vaccinated children)
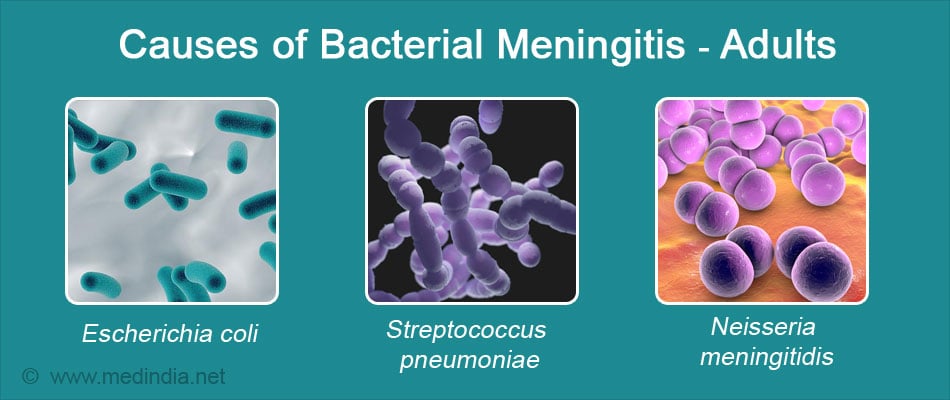
In adults, bacterial meningitis is caused by:
- Neisseria meningitides
- Listeria monocytogenes (immunocompromised individuals; old age)
- Streptococcus pneumonia
- Staphylococcus aureus (endocarditis) & Haemophilus influenzae (sinusitis, otitis)
What are the Risk Factors for Bacterial Meningitis?
The following factors increase the risk of contracting meningitis infection:
- Presence of sinus or middle ear infection
- Age (< 5 or > 60)
- Persons who have undergone spleen removal – since spleen is a major immune organ
- Co-morbidities (HIV, sickle cell disease, diabetes, cancer)
- Malnutrition
- Alcoholism
- Missing routine vaccinations
- Pregnancy – increases the risk of Listeria infection
- Persons living away from home accommodations such as college hostels, military bases boarding school or foster care facilities where the infection can easily spread.
What are the Symptoms and Signs of Bacterial Meningitis?
The main symptoms of bacterial meningitis in 95% of adults are:
- Fever
- Headache
- Changes in mental function
- Neck stiffness

There may also be
- Swelling of the brain parenchyma (meningoencephalitis)
- Swelling of the spinal cord
- Swelling of the ventricles in the brain (ventriculitis)
- Vomiting, heightened sensitivity to light (photophobia) and sound (phonophobia) (signs of meningeal irritation)
- Seizures
- Consciousness is altered
- Coma
A few of the adults will exhibit neck stiffness, changes in mental function, and fever together but this is frequently observed in pneumococcal meningitis rather than in meningococcal meningitis.
In infants, the symptoms are not very specific. They may present with one of the following symptoms:
- Feeding poorly
- Irritability
- Fever
- Lethargy
- Vomiting
- Bulging fontanelles may be present in the presence of raised intracranial pressure
The symptoms present in older children are:
- Neck stiffness with feeling of resistance when the doctor tries to bend the neck forward
- Meningeal irritation accompanied by vomiting
- Increased sensitivity to light (photophobia)
- Headache
- Seizures have been reported in children especially in pneumococcal or Haemophilus influenzae meningitis.
- Rashes aremainly observed in meningococcal infections.
What are the Complications of Bacterial Meningitis?
Complications aremore likely to occur in untreated cases or when treatment is delayed. These include the following:
- Blindness
- Deafness
- Seizures
- Impairment of memory
- Learning difficulties
- Difficulty in walking
- Weakness or paralysis of limbs
- Kidney failure
- Shock
- Death
How do you Diagnose Bacterial Meningitis?
To diagnose bacterial meningitis, the following tests are recommended.
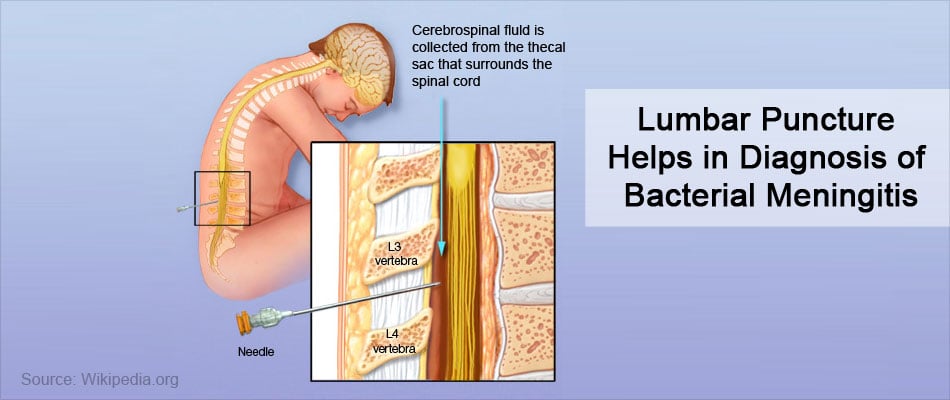
Lumbar puncture to obtain cerebrospinal fluid (CSF) for analysis and Gram-staining
CSF cultures, is recommended.
In bacterial meningitis, CSF biochemical analysis reveals
- A high white blood cell count (<500 cells/ml)
- High protein content
- Increased neutrophils (80% - 95%)
- Reduced glucose content
- Increased lactate content
A Gram stain of the CSF and culture reveals the organism in most cases.
A primary source of infection should be ruled out such as sinus inflammation, ear infection and a chest x-ray to rule out lung infection.
Blood cultures are also performed especially when there is a delay in obtaining CSF
However, Gram-staining CSF cultures, is nearly 90% accurate as compared with just 50% accuracy in blood cultures.
Serum C-reactive protein (CRP) – This test is useful to distinguish between bacterial and viral meningitis. A normal CRP excludes the diagnosis of bacterial meningitis with 99% accuracy.
Diagnostic imaging
A CT scan of the brain should be done before attempting a lumbar puncture in cases of altered sensorium, swelling of the optic discs, new onset seizures, focal neurological deficits or immunocompromised persons to rule out brain abscess or swelling of the brain.
Brain imaging may also reveal any underlying complications such as death of brain tissue, brain swelling or hydrocephalus (increased CSF in the brain).
How do you Treat Bacterial Meningitis?
In cases of suspected meningitis, the person is admitted to the hospital for further investigations and for administering intravenous antibiotics.
The person may be kept in a darkened room as there may be light sensitivity in meningitis.
Intravenous fluids are administered to prevent dehydration and shock.
Until the results of the diagnostic tests come in, patients are administered medications (empirical) based on suspected meningitis. Corticosteroids and antibiotics are administered in the treatment of bacterial meningitis.

1. Corticosteroids – Dexamethasone is the prescribed treatment for children (0.15 mg/kg for 2 to 4 days every 6 hours) and adults (10 mg for 4 days every 6 hours). Dexamethasone should be administered at least 10 to 20 minutes prior to the start of antibiotic therapy. It is not recommended giving dexamethasone later as it is ineffective. Infants are not prescribed dexamethasone.
2. Analgesics – Headaches are treated with analgesics, such as opioids.
3. Antibiotics – Antibiotics need to be prescribed immediately even before the diagnostic tests are verified. Antibiotics should be given based on the medical history of the patient (e.g. Age and any prior medical condition).
A patient suspected with meningococcus should be isolated in the first 24 hours of treatment. If the condition does not improve, then a CT scan and lumbar puncture should be repeated.
The antibiotic course varies depending on the type of bacterial infection.
- Uncomplicated meningococcal meningitis – 5 days to a week
- Enterobacteriaceae, Listeria monocytogenes – 3 to 4 weeks
4. Anti-epileptic treatments are administered for seizures.
How do you Prevent Bacterial Meningitis?
- Haemophilus influenzae is no longer a risk in developed countries due to effective vaccination programs. Pneumococci infections have also been controlled with effective vaccination. However, pneumococcal strains have developed resistance to beta-lactam antibiotics.
- Neisseria meningitidis is now the main infecting organism of bacterial meningitis in developing countries as well as in Europe and the US. There are vaccines for N. meningitidis to prevent infections.

- Pregnant women should get themselves tested for group B Streptococcus and take the required antibiotics during labor to prevent transmission to the baby.
- Persons at risk who should be vaccinated include infants, the elderly, those with a weak immune system and persons who have undergone splenectomy.
- Avoid contact with -
- People who are infected with meningitis
- Cigarette smoke or smoking
- Antibiotic prophylaxis of family members in close contact with someone who has meningitis.
What is the Prognosis of Bacterial meningitis?
With prompt attention and if the condition is treated in its early stages, most people recover. However, it is estimated that there is a 10% mortality rate. Some persons who recover may have residual neurological deficits such as loss of vision or hearing, onset of seizures, and weakness or paralysis of limbs.