- Autoimmune Hepatitis: A Review of Current Diagnosis and Treatment - (http://dx.doi.org/10.1155/2011/390916)
- Autoimmune Hepatitis - (https://www.niddk.nih.gov/health-information/liver-disease/autoimmune-hepatitis)
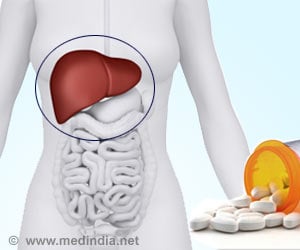
What is Autoimmune Hepatitis?
Autoimmune hepatitis is an inflammatory disease of the liver that arises due to a problem with the immune system. Hepatitis refers to inflammation of the liver, while autoimmune refers to a seemingly protective but inappropriate immune response that the body launches against its own tissues.
An autoimmune disease is one where the body’s defense mechanisms perceive one’s own tissues as foreign and launch an immune attack against them. This results in damage and destruction of the cells and tissues leading to disease. Autoimmune disease can affect any organ of the body.
Autoimmune hepatitis is a very rare condition. Like most other autoimmune disorders, it is more common in women as compared to men.
What are the Causes of Autoimmune Hepatitis?
Autoimmune hepatitis occurs when the white blood cells of the body produce an inappropriate immune response against the liver cells, thereby causing inflammation and damage. The exact cause of autoimmune hepatitis is not known. Affected people may have a genetic predisposition for the condition, which may be triggered by an environmental factor. Around 20% patients suffering from a genetic condition called autoimmune polyendocrinopathy-candidiasis-ectodermal dystrophy (APECED) syndrome suffer from autoimmune hepatitis.
The environmental trigger could be:
- Drugs like infliximab, minocycline, atorvastatin, diclofenac, isoniazid, methyldopa, nitrofurantoin, and propylthiouracil, the hepatitis A vaccine, and herbal agents like black cohosh and dai-saiko-to. The autoimmune hepatitis may improve after stopping the medication
- Viruses such as hepatitis A, B, or C, or measles virus
What are the Types of Autoimmune Hepatitis?
Autoimmune hepatitis is of two main types, type 1 and type 2
- Type 1 autoimmune hepatitis usually first manifests in adolescence or young adults. Females are most commonly affected.
- Type 2 autoimmune hepatitis is less common than type 1 and usually first manifests in children. Its prognosis or outcome is often worse than type 1 disease.
What are the Risk Factors for Autoimmune Hepatitis?
People who suffer from other autoimmune diseases are also at a risk of autoimmune hepatitis. These include autoimmune diseases that primarily affect:
- The liver like primary sclerosing cholangitis
- The pancreas like type 1 diabetes
- The digestive tract like celiac disease, Crohn’s disease and ulcerative colitis
- The thyroid like Grave’s disease and Hashimoto’s thyroiditis
- The kidney like proliferative glomerulonephritis or lupus nephritis
- The joints like rheumatoid arthritis
- The salivary glands like Sjogren’s syndrome

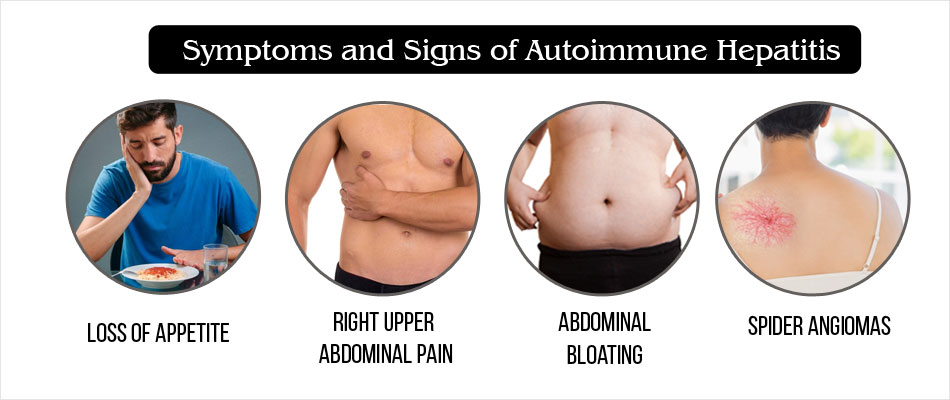
What are the Symptoms and Signs of Autoimmune Hepatitis?
Some people with autoimmune hepatitis do not suffer any symptoms, and an abnormality in liver enzymes may be detected when the test is done for some other purpose or as a part of a routine health checkup. The symptoms of autoimmune hepatitis are very much similar to other forms of hepatitis.
Symptoms and signs of milder forms of autoimmune hepatitis include:
- Nausea, loss of appetite, fatigue, joint pain
- Jaundice, which is characterized by yellowish discoloration of the skin and eyes, along with dark yellow urine and light-colored stools
- Pain or discomfort over the liver in the right upper abdomen
- Skin rashes
As autoimmune hepatitis progresses, the following symptoms and signs of cirrhosis and liver failure may be noted
- Abdominal bloating due to enlarged liver and fluid accumulation. Fluid accumulation in the abdomen is called ascites
- Easy bruising and prolonged bleeding time
- Generalized itching
- Esophageal varices (swellings of blood vessels at the base of the food pipe) which could bleed
- Presence of spiderlike blood vessels called spider angiomas on the skin
- Drowsiness, confusion and coma
What are the Complications of Autoimmune Hepatitis?
Some patients with autoimmune hepatitis progress to
- Cirrhosis,
- Liver failure and even Liver cancer
How to Diagnose Autoimmune Hepatitis?
It is difficult to suspect autoimmune hepatitis only based on the symptoms since several liver diseases cause similar symptoms. It is therefore important to rule out other causes of liver disease like viral hepatitis, alcoholic hepatitis and drug-induced hepatitis while making the diagnosis of autoimmune hepatitis. Diagnosis of autoimmune hepatitis is based on the following:
- Medical history of the patient where the patient will complain of the symptoms mentioned above. The patient may also give a history of suffering from another autoimmune disease
- Physical examination may reveal the presence of jaundice, pain over the liver, an enlarged liver, and other signs of liver disease as mentioned above.
- Blood tests: Blood tests done for autoimmune hepatitis include liver function tests and tests for autoantibodies
- Liver function tests will indicate high bilirubin levels, increase in liver enzymes, and prolonged bleeding and clotting times

- The blood will be positive for the presence of certain antibodies. Antibodies are proteins produced by the white blood cells that normally participate in the immune response:
- Hypergammaglobulinemia (An increase in IgG antibodies is noted, which is referred to as hypergammaglobulinemia) in the absence of cirrhosis is an important diagnostic criteria for autoimmune hepatitis. The IgA and IgM antibody levels are normal.
- Patients with type 1 autoimmune hepatitis are usually positive for antinuclear antibody (ANA), anti-smooth muscle antibody (SMA), or both
- Patients with type 2 disease are usually positive for anti-liver kidney microsomal (LKM) 1 and/or anti-LKM3 and/or anti-liver cytosol 1 (LC1) antibodies
- Liver biopsy: A liver biopsy is an outpatient procedure where a small piece of the liver is obtained with the help of a special needle that is inserted into the liver. The piece is then sent for pathological examination, which gives an accurate diagnosis of the type of liver disease. The biopsy also helps to understand the severity of the liver disease.
- Imaging tests: An ultrasound will help to detect changes in the liver like cirrhosis (liver inflammation) and liver cancer, that could occur during the course of the disease
How do you Treat Autoimmune Hepatitis?
Treatment of autoimmune hepatitis is based on the following:
- Medications are given to reduce immunity as the disease is primarily caused by an inappropriate immune response launched by the body against its own tissues.
- Corticosteroids like prednisone reduce immunity and can even bring about a remission of autoimmune hepatitis. Long-term intake of corticosteroids can cause side effects like increased risk of infection, thinning of muscles, bone, skin and hair, redistribution of fat, stomach ulcers, glaucoma, cataract, and predisposition to diabetes and hypertension. Therefore, prednisone is initially given at a higher dose, but is later reduced to the minimum necessary dose.
- Drugs like azathioprine may be used along with prednisone. The addition of azathioprine helps to reduce the corticosteroid dose. Azathioprine also reduces immunity, and can predispose to certain cancers
- Other immunosuppressant drugs like mycophenolate mofetil, cyclosporine or tacrolimus may be used

Patients in the very early stage of the disease may go into remission without any treatment. These patients have to be carefully followed up to look for signs of reappearance of the disease. Patients in whom treatment is started often respond dramatically to immunosuppressive medications, and sometimes even go into remission with the treatment. Signs of remission include absence of symptoms, normalization of liver enzymes and serum IgG levels, and an improvement demonstrated in liver biopsy. Treatment can be completely withdrawn in such patients and reinstated if the disease reappears.
Liver transplant. A liver transplant is the only option for patients who have progressed to liver failure.