- Arthrogryposis Multiplex Congenita - (https://rarediseases.org/rare-diseases/arthrogryposis-multiplex-congenita/)
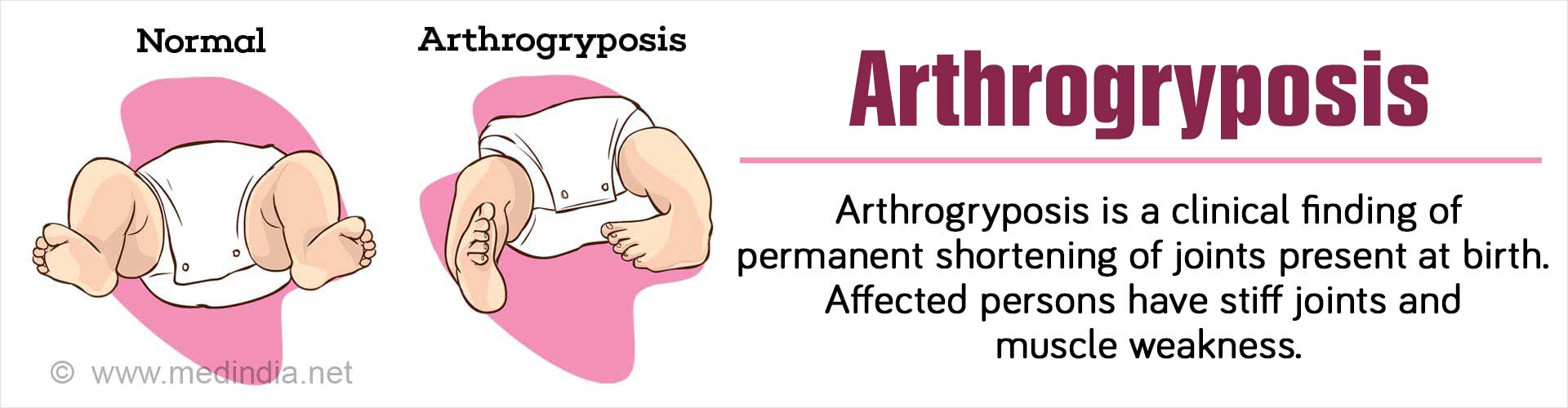
What is Arthrogryposis?
Arthrogryposis or Arthrogryposis multiplex congenita (AMC) is a general term for non-progressive congenital joint contractures affecting two or more joints in the body. When a joint is fixed with limited or total loss of function, it is called contracture.
The term is used to describe approximately 300 different conditions causing multiple short and stiff joints in different parts of the body.
In contrast, when contracture is limited to only one body part it is called isolated congenital contracture. For example, clubfoot is an isolated congenital contracture.
AMC is a non-progressive condition meaning that the stiffness or lack of movement, does not get worse with time, however, it is advisable that affected persons seek medical advice to potentially prevent further complications of the joints.
AMC is congenital (present at birth). Its distribution among the males and females is same. It is more prevalent among Asians, Africans and Europeans. Arthrogryposis is seen in about 1 in 3000 to 1 in 5000 live births.
What are the Different Types of Arthrogryposis?
There are more than 300 conditions included under the Arthrogryposis ‘umbrella’. These can be further subdivided into three groups namely
1. Disorder involving mainly limbs - Amyoplasia or classical arthrogryposis
- Involves mainly limbs – usually all four limbs
- Incidence is about 1 in 10,000 births and represents a third of all cases
- It is not an inherited condition, but parents of a baby with amyoplasia are advised to seek genetic counselling for their child as they approach adolescence
2. Disorder involving limb and another body part - such as heart defects, intestinal anomalies, cleft palate. Examples include multiple pterygium syndromes, Freeman-Sheldon syndrome, distal arthrogryposis types IIB, IIC, IID and IIE
3. Disorder involving limbs and the nervous system
Sadly, babies born with this type tend to do very poorly and may not live. The condition is usually quite obvious in the neonatal (first 28 days) period.
What are the Causes of Arthrogryposis?
Arthrogryposis is a clinical finding due to various underlying causes (some inherited), but not a diagnosis per se. Its presentation is diverse. The cause is not identified in most of the cases.
Arthrogryposis Multiplex Congenita (AMC) is not due to a defect in the formation of the joints, but a defect involving the development of the connective tissues around them. This occurs after 8-10 weeks of pregnancy. The connective tissue disorder fuses the joint in a specific position. As a result, the tendons around the involved joint are unable to stretch to their normal length. When this persists, contractures result.
The following factors have been associated with different forms of arthrogryposis.
1. Internal factors:
- About 350 genes are identified to be associated with arthrogryposis. Distal arthrogryposis is usually inherited in autosomal dominant fashion.
- Neural diseases of the fetus: Fetuses with Myelomeningocele, anencephaly, holoprosencephaly or spinal muscular atrophy are associated with AMC. These occur due to multifactorial causes.
- Muscular diseases of the fetus: Muscular dystrophy can cause decreased fetal movement and may be associated with AMC.
- Connective tissue disorders of the fetus: They can cause limited fetal movement and contractures.
- Vascular compromise – Impaired blood circulation which affects the nerves that supply the muscles and bones of the joint during fetal development
2. External factors:
Limited fetal movement in utero can cause arthrogryposis. Joint movement in utero is necessary for a proper joint development. A limited joint movement leads to excess connective tissue deposition near the joint and causes contractures. The following are the causes of limited fetal movement
- Limited space
- Oligohydramnios
- Multiple pregnancy
- Uterine anomalies
- Maternal illness
- Maternal drug use
- Maternal viral infections
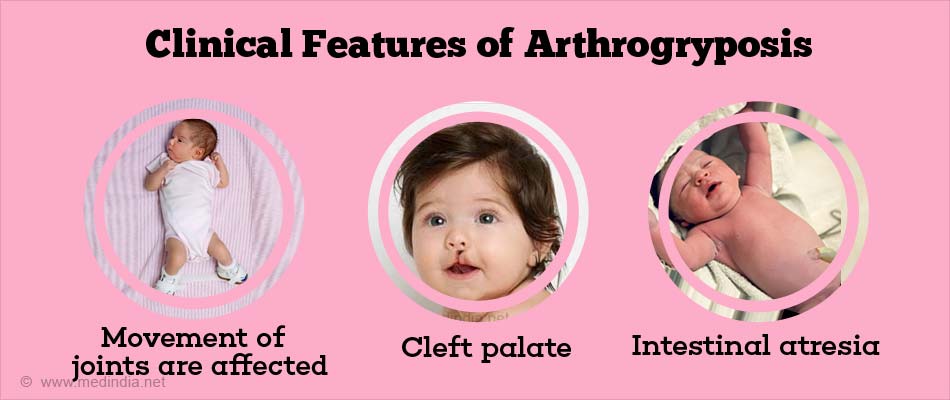
What are the Clinical Features of Arthrogryposis?
The severity and diversity of arthrogryposis depend upon the underlying cause.
- The main symptom in AMC is occurrence of congenital contractures involving 2 or more joints. The movement of the affected joint is partially or completely lost. The muscles may be less developed in the affected limb. Skin creases are characteristically absent and subcutaneous tissue is thin.
- Other associated conditions with AMC are the cleft palate, cryptorchidism and fragile bones, craniofacial deformities, skeletal urinary tract or nervous system defects.
- Amyoplasia: Patients with amyoplasia have multiple and severe joint contractures. In most patients with amyoplasia, there is adduction of the shoulder, elbows are extended, the wrist is flexed and fingers are flexed and stiff. The distal joints are more affected than proximal. Hip dislocation may be present. A birthmark on face called stork mark may be seen. 10% patients have gastroschisis or intestinal atresia usually associated with a severe clubfoot.
- Distal arthrogryposis mostly involves distal joints. The symptoms are highly variable. Distal arthrogryposis like Freeman-Sheldon syndrome, Gordon syndrome may have associated craniofacial anomalies.
How do you Diagnose Arthrogryposis?
1. Maternal History, Patient Examination
The clinical presentation, patient history (family history, antenatal history of maternal illness, drug intake), birth history (type of birth and duration of labor) and physical examination findings speak for themselves and help to identify the condition.
2. Miscellaneous Tests To Identify Possible Cause
- Electromyography: To assess electrical activity in muscle.
- Nerve conduction studies: Test to assess the transmission of electrical impulse in nerve.
- Muscle biopsy: A small portion of a muscle is removed and studied under the microscope. It helps to identify muscular disorders.
- Imaging tests - CT scan and MRI of the brain and spinal cord may help in finding the cause.
How do you Treat Arthrogryposis?
- Physical therapy: Physical therapy in newborns helps to prevent muscle atrophy and improves joint function. Passive stretching and gentle joint manipulation can help.
- Passive enhancement: Several assistive devices are available which enable the muscle movement and exercise.
- Surgery: Surgeries help to improve the joint function. Osteotomy tendon transfer, soft tissue release or skin flaps may be required.
- Psychosocial treatment – Counseling and support for patient and family is an integral part of management of this condition
- Genetic counselling: It may be beneficial in families with heritable AMC.
Prognosis of Arthrogryposis
- In patients with arthrogryposis, it looks the worst at birth. It is non-progressive and improves with treatment. But, there is no complete cure.
- Treating the contractures to improve the mobility of the joints enables the patient to do their daily normal activities and live a near normal life.