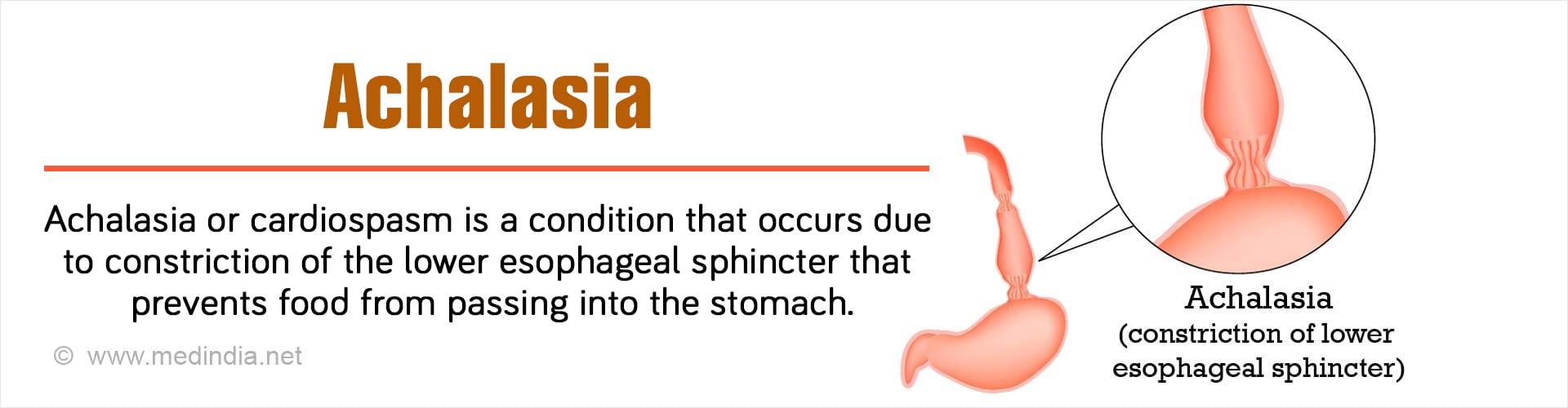
- Achalasia - Mayo Clinic - (https://www.mayoclinic.org/diseases-conditions/achalasia/symptoms-causes/syc-20352850)
- Swallowing Problems: Achalasia - (https://my.clevelandclinic.org/health/diseases/17534-swallowing-problems-achalasia)
- O'Neill OM, Johnston BT, Coleman HG. Achalasia: A review of clinical diagnosis, epidemiology, treatment and outcomes. World J Gastroenterol. 2013 Sep 21; 19 (35): 5806-12. DOI: 10.3748/wjg.v19.i35.5806 . PMID: 24124325.
Overview on Thyroid Function
The thyroid is a small gland located at the base of the neck, under the voice box. It produces two hormones thyroxine (T4), and triiodothyronine (T3). The numbers 3 and 4 denote the number of iodine atoms. T3 is the biologically active form of the hormone; T4 has to be converted to T3 to be active.Both T3 and T4 play an important role in metabolism, growth, and development of the body, and transportation of proteins. Hence their levels have to be maintained for the body cells to function smoothly.
If there is too much of T4 or T3 secreted, the cells overwork themselves leading to a condition called hyperthyroidism (overactive thyroid) and if there is too little of T4 or T3 secreted, the cells work at a less than average rate causing hypothyroidism (underactive thyroid).
The pituitary gland and hypothalamus both control the thyroid through a negative feedback loop, to make sure the right or normal amounts of T4 and T3 are manufactured and delivered into the blood stream. When the thyroid hormone levels drop, the hypothalamus secretes Thyroid Releasing Hormone (TRH), which causes the pituitary gland to release Thyroid Stimulating Hormone (TSH) which in turn controls the thyroid hormone levels.
Symptoms of hyperthyroidism include heat intolerance, rapid heartbeat, hand tremor, anxiety, frequent bowel movements, excessive eating, difficulty sleeping, muscle weakness, and weight loss.
Typical symptoms of hypothyroidism include fatigue, constipation, weight gain or obesity, heart disease, depression, impaired memory, abnormal thyroid growth, poor ability to tolerate cold, and thyroid cancer.
Can Drugs Alter Thyroid Hormone Levels?
Many different drugs and medications can affect thyroid function in patients with otherwise normally functioning thyroid gland and in those consuming exogenous levothyroxine.Drugs can alter thyroid hormone levels by affecting their synthesis and secretion from the thyroid gland, or affecting their metabolism through deiodination, sulfation and glucuronidation, by altering affinity of levels of thyroxine binding globulin, by affecting absorption of thyroid hormone in patients who are dependent on exogenous levothyroxine, and through suppression of TSH in the thyrotropes in the anterior pituitary gland or hypothalamus.
What is Drug-Induced Hyperthyroidism?
Drug-induced hyperthyroidism happens when drugs increase the levels of the thyroid hormones. Case in point is Hyperthyroidism due to iodine medications in patients with thyroid nodules.1. Some medications which cause hyperthyroidism by stimulation of thyroid hormone synthesis and/or release include:
- Amiodarone
- A drug used to treat cardiac arrhythmias. It contains iodine which is used by the thyroid gland to produce more quantity of hormones
- Iodine – Excess iodine intake in the form of dietary supplements, and contrast agents can lead to hyperthyroidism
- Lithium – It is used to treat bipolar disorder, can cause goitre (swelling of thyroid gland)
What is Drug-Induced Hypothyroidism?
Drug-induced hypothyroidism occurs when drugs are responsible for causing a decrease in the levels of the thyroid hormones.The drugs known to affect thyroid function in patients with normal hypothalamus and their mechanism of actions are listed below:
- Thionamides, propylthiouracil, methimazole, lithium, amiodarone, iodine and iodine-containing drugs through inhibition of synthesis and / or release of thyroid hormones
- Lenalidomide, interferon-alpha and interleukin-2 therapy through drug-induced thyroiditis
- Glucocorticoids, somatostatin analogs, rexinoids like bexarotene, and dopamine agonists through suppression of TSH in the hypothalamus.
- Iron, calcium, raloxifene, and sucralfate by inhibiting levothyroxine absorption
- Phenytoin, phenobarbital, and rifampin by increasing hepatic metabolism of T4
- Raloxifene, estrogen, and tamoxifen - increased thyroxine binding globulin levels
- Glucocorticoids and nicotinic acid - decreased thyroxine binding globulin levels
- Autoimmune disease (e.g. thyroiditis)
- Thyroidectomy (Thyroid surgery)
- Previous history of thyroid disease
- Female gender
- Pre-existing antithyroid antibodies
- Lithium
- Antacids - Most of the antacids contain aluminium hydroxide which is reported to reduce the body’s ability to absorb thyroxine.
- Statins - Cholesterol reducing drugs- A gap of about four to five hours should be maintained between administering these drugs and thyroid hormones, as these drugs are known to bind with thyroid hormones.
How do Herbal Supplements affect Thyroid Function?
Examples of herbal supplements which affect thyroid function are:- Guggul (made from the gum of the Commiphora mukul tree native to India) products are known to improve the uptake of iodine, thus able to reverse hypothyroidism
- Indian Ginseng is used to reduce anxiety and stress. It also helps improve thyroid function
- Ashwagandha herb (Winthania Somnifera) has anti-oxidizing properties and is known to reduce inflammation of thyroid
- Flaxseed prevents the occurrence of hypothyroidism by promoting the production of thyroid hormones. It contains high levels of omega-3 fatty acids