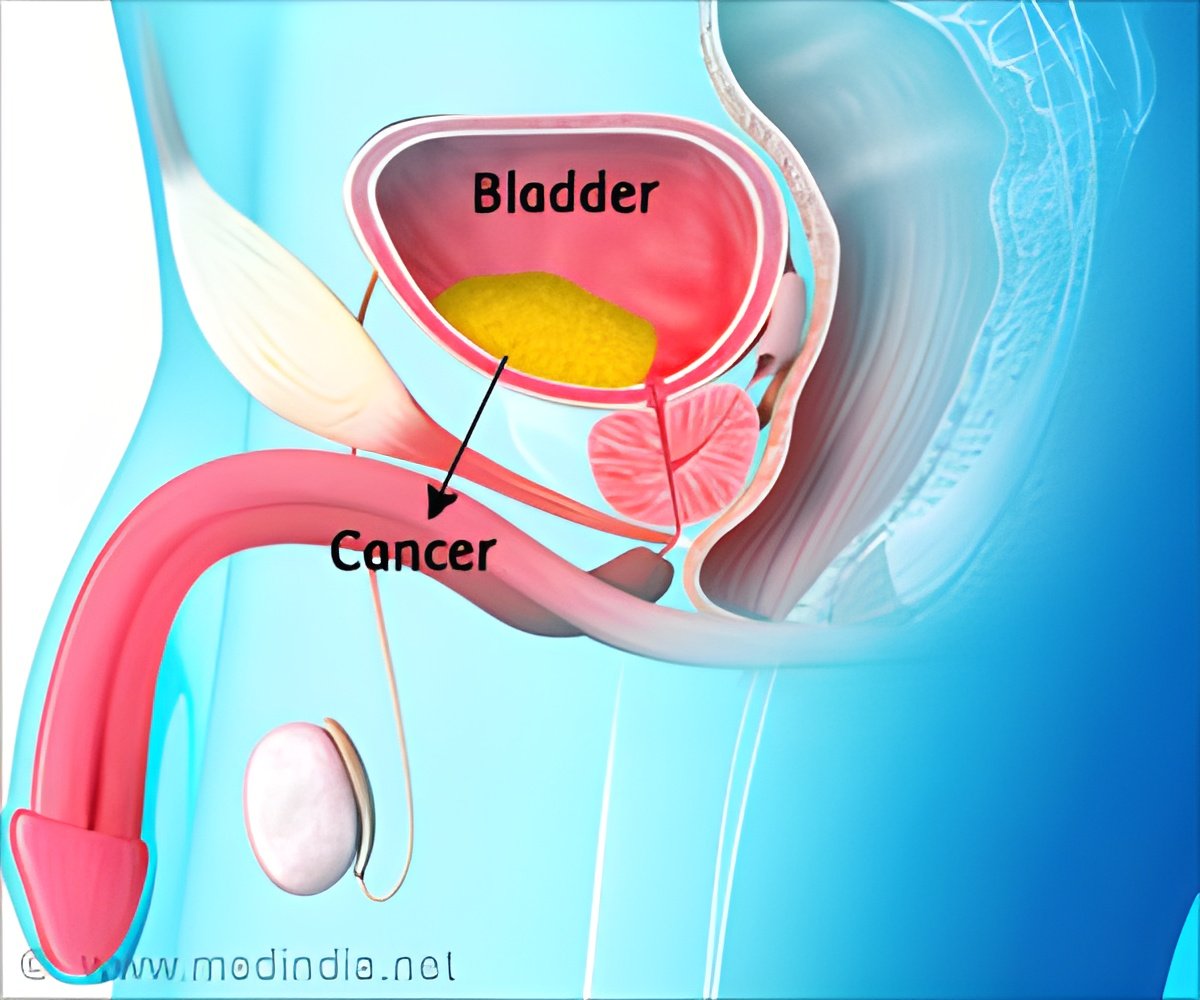
‘The combination of cystoscopy and renal ultrasound was the most cost-effective with an incremental cost of $53,810 per bladder cancer detected.’
Tweet it Now
A new article published by JAMA Internal Medicine explores the cost-effectiveness of four initial diagnostic protocols for these patients.Joshua A. Halpern, M.D., M.S., of Weill Cornell Medicine, New York, and his coauthors analyzed the cost-effectiveness of: computed tomography (CT) alone, cystoscopy (using a scope to examine the urinary tract) alone, CT and cystoscopy combined, and renal (kidney) ultrasound and cystoscopy combined.
The combination of cystoscopy and renal ultrasound was the most cost-effective with an incremental cost of $53,810 per cancer detected, according to the results.
"The use of ultrasound in lieu of CT as the first-line diagnostic strategy will reduce the cost, morbidity and national expenditures associated with evaluation of AMH [asymptomatic microscopic hematuria]. Clinicians and policy makers should consider changing future guidelines in accordance with this finding," the article concludes.
Source-Eurekalert