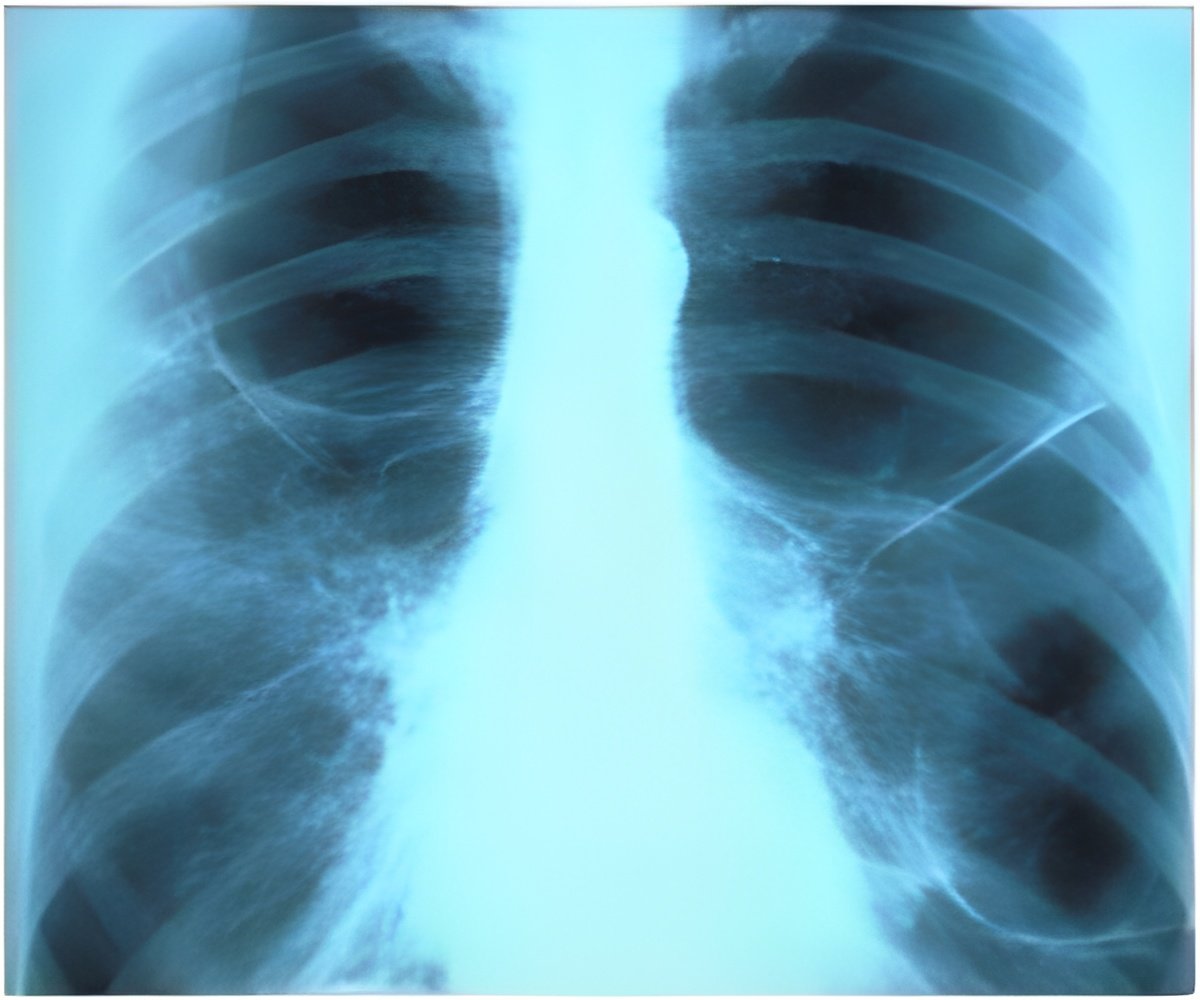
The researchers added isoniazid and a "reducing agent" known as cysteine to the TB in a test tube, expecting the bacteria to develop drug resistance.
Instead, the team "ended up killing off the culture", according to the study's senior author William Jacobs, who said the result was "totally unexpected".
Reducing agents chemically reduce other substances.
The team then replaced the cysteine in the experiment with another reducing agent -- Vitamin C.
It, too, killed the bacteria.
Advertisement
"Even more surprisingly... when we left out the TB drug isoniazid and just had Vitamin C alone, we discovered that Vitamin C kills tuberculosis."
Advertisement
In the lab tests, the bacteria never developed resistance to Vitamin C -- "almost like the dream drug", Jacobs said in a video released by the college.
He stressed the effect had only been demonstrated in a test tube so far, and "we don't know if it will work in humans", or which dose might be useful.
"But in fact before this study we wouldn't have even thought about trying this study in humans."
In March, disease experts warned of a "very real" risk of an untreatable TB strain emerging as more and more people develop drug resistance.
In 2011, there were believed to be some 12 million TB cases in total -- 630,000 of them of the multi-drug resistant (MDR) variety which does not respond to the most potent drugs -- isoniazid and rifampin.
Extensively drug resistant (XDR) TB, does not respond to an even wider range of drugs.
TB was declared a global health emergency by the World Health Organisation (WHO) 20 years ago, but remains a leading cause of death by an infectious disease despite a 41-percent drop in the death rate from 1990 to 2011.
In 2011, 8.7 million people fell ill with TB and 1.4 million died, said the WHO.
Over 95 percent of TB deaths occur in low- and middle-income countries, and it is a leading killer of people with HIV.
An airborne disease of the lungs, tuberculosis is usually treatable with a six-month course of antibiotics.
Resistance to TB drugs develops when treatment fails to kill the bacteria that causes it -- either because the patient fails to follow their prescribed dosages or the drug doesn't work.
It can also be contracted through rare forms of the disease that are directly transmissible from person to person.
MDR TB in the United States can cost as much as $250,000 (200,000 euros) per patient to treat.
XDR TB requires about two years of treatment with even more expensive drugs that cause side-effects and offer no guarantee of a cure.
The authors of the new study urged further research into the potential uses of Vitamin C in TB treatment, stressing it was "inexpensive, widely available and very safe to use."
"This would be a great study to consider because we have strains of tuberculosis that we don't have drugs for, and I know in the laboratory that we can kill those strains with Vitamin C," said Jacobs.
Source-AFP