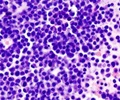
According to the research conducted by the scientists at St. Jude Children’s Research Hospital it was found that mutation and loss of tumor suppressor gene resulted in aggressive leukemias. Researchers have used mouse models to determine the reason behind aggressive nature and drug resistant nature of the acute lymphoblastic leukemia (ALL). The investigators found that the combination of a mutation called Bcr-Abl and the loss of both copies of the tumor suppressor gene Arf in bone marrow cells triggers an aggressive form of ALL. Loss or inactivation of both Arf genes resulted in the multiplication of leukemic cells. These cells later did not respond to the drug imatinib. Imatinib is used to treat chronic myelogenous leukemia (CML), another blood cell cancer caused by the Bcr-Abl mutation.
Hence the St. Jude study provided evidence that imatinib resistance in mouse models of ALL did not depend on the presence of Bcr-Abl and the loss of Arf genes in the cancer cells. But depends on the interaction of the tumor cells with specific growth-promoting factors produced in the mice. When the leukemic cells from mice that had failed imatinib therapy were removed JAK kinases, which inhibits enzymes restored the cells’ imatinib sensitivity. The study’s findings were published in the journal of Proceedings of the National Academy of Sciences. The Bcr-Abl oncogene is formed when a fragment of the Bcr gene from one chromosome switches over to fuse with a portion of the Abl gene from the other chromosome. Bcr-Abl encodes for an enzyme called a tyrosine Kinase. This causes the abnormal, uncontrolled multiplication of leukemic cells. It was also shown that by inhibiting the Bcr-Abl kinase with imatinib durable remissions of cancer with minimal side effects in patients with CML was possible.But imatinib has proven less effective in treating ALL patients with the Bcr-Abl mutation, and the basis of drug resistance in this disease is not clearly understood. But Charles J. Sherr, M.D., Ph.D., a Howard Hughes Medical Institute investigator and co-chair of the St. Jude Department of Genetics and Tumor Cell Biology said that Arf acts as a safeguard against the cancer-causing effects of Bcr-Abl. The St. Jude team found that Arf is not inactivated in CML patients who respond to imatinib. But in case of ALL Arf gene is lost frequently and imatinib treatment is far less effective. This inactivation of Arf in ALL cells expressing the Bcr-Abl enzyme gives these cells a strong proliferative nature which might contribute to imatinib resistance. So the researchers used a virus-like piece of DNA to carry the Bcr-Abl oncogene into bone marrow-derived lymphocytes obtained from mice that either retained Arf or were previously engineered to lack this gene. These pre-B lymphocytes represent one type of white blood cell that can become cancerous and cause ALL.
The researchers then transplanted these transformed cells carrying Bcr-Abl back into normal mice. Animals that received transformed pre-B cells that had both copies of the Arf gene intact were highly resistant to disease development. However, mice injected with cells that carried Bcr-Abl and lacked Arf rapidly developed an aggressive form of ALL that could not be cured with high doses of imatinib. Richard T. Williams, M.D., Ph.D., a fellow in Sherr’s laboratory and the paper’s lead author said that tumor cells when removed from these resistant mice and treated with imatinib in cell cultures they were still very sensitive to this drug. Hence he said that the failure of imatinib to cure the mice depended on some substance in the animal that stimulated tumor cell replication or survival.
They soon found that it might be the B lymphocyte stimulating protein IL-7. It is produced in the bone marrow enhancing the proliferation of cultured leukemic cells removed from the mice and made the cells resistant to imatinib’s growth inhibitory effects. It binds to receptors on the surface of lymphocytes, which triggers the activity of the JAK kinases. This later stimulates cell growth through a signaling pathway that operates alongside the one controlled by the Bcr-Abl kinase. The investigators used a chemical inhibitor of JAK kinases to block the effect of IL-7 on leukemic cells in culture which restored the ALL cells’ sensitivity to imatinib. In conclusion the team said that the study has provided unexpected insights into how factors in the mice and potentially in humans might contribute to imatinib resistance.