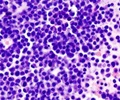
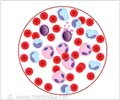
The improvements made in diagnoses and treatment of the fatal childhood cancer acute lymphoblastic leukemia (ALL) will result in a cure rate of 90%, according to researchers belonging to the St. Jude Children's Research Hospital.
The progressive improvement in the cure rate since 1962, when only 4% of children with ALL survived, reflects in large part the more effective use of existing drugs and the incorporation of sophisticated genetic technologies to personalize treatments. Research findings at St. Jude have enabled clinicians to identify patients for whom standard treatment is most likely to fail, and who should therefore be treated more aggressively. These findings have also allowed clinicians to choose the optimal drugs and drug dosages for individual patients.The improvements in ALL treatment are also helping to reduce the long-term toxic side effects of the therapy by enabling clinicians to reduce or avoid the use of certain drugs or radiation that can damage major organs or cause secondary cancers.
A 90% cure rate for ALL is quite possible in the near future if we continue to incorporate the breakthroughs of past decades and successfully overcome the remaining challenges. This reflects the ability of St. Jude to provide free treatment to all children regardless of their ethnic or racial backgrounds or their ability to pay, and to tailor the treatment according to their specific needs.
That success is based to a large extent on the work done at St. Jude and elsewhere in identifying specific mutations in leukemic cells that strongly suggest the likelihood that treatment will fail the child, the authors reported. Adding to the complexity of the patient's response to treatment are differences in how quickly the body activates, breaks down or eliminates specific cancer drugs.
Pharmacogenomics is the study of the effects of different genes on the response to drugs. Such studies often include the analysis of the roles of hundreds or even thousands of genes.
Another significant contribution made by St. Jude researchers is the measurement of minimal residual disease (MRD), that is the small populations of leukemic cells that survive initial treatment (induction therapy). These cells can replenish the population of leukemic cells and cause the patient to relapse.
Advertisement