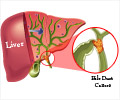
Laparoscopic cholecystectomy (LC) has rapidly substituted traditional cholecystectomy, and represents the gold standard for surgical treatment of cholelithiasis. Bile duct injury (BDI) remains the most serious complication of cholecystectomy. According to a recent survey, published in the October issue of the journal Archives of Surgery, the incidence of BDI has become more frequent with LC. The study verifies the current incidence, mechanism, presentation, and treatment of BDI occurring during LC in general surgical practice. The authors report the results of a recently performed multicenter national survey to provide an up-to-date assessment of the rate, causes, clinical manifestations, and treatment of BDI in 56, 591 patients who underwent LC between January 1, 1998, and December 31, 2000, in 184 hospitals in Italy. Out of these, 235 BDIs were reported, with an overall incidence of 0.42%. There were no risk factors in 80.0% of the patients.
Poor identification of the anatomical features of the hepatic pedicle was the most frequently reported cause (36.8%), and technical problems accounted for 27.0% of causes. The incidence of BDI was higher during cholecystitis (P<.001) and decreased with increasing number of LCs performed by the surgical teams (P<.01). There was no difference in incidence according to technique (French or US) or to routine or selective intraoperative cholangiography.One hundred eight BDIs (46.0%) were recognized intraoperatively and immediately repaired in 89.8% of patients. One hundred twenty-seven BDIs (54.0%) were diagnosed postoperatively, the dominant manifestation being biliary fistula (44.1%).
This study confirms a higher incidence of BDI during LC. It highlights the relevance of the number of previously performed LCs and of the correct surgical technique to avoid BDI. The need for correct procedures, adequate expertise of the repairing surgeon in BDI repairs, and a multidisciplinary approach in the management of BDI is emphasized.