Among infants, hypoxic–ischemic encephalopathy due to acute perinatal asphyxia remains an important cause of neurodevelopmental deficits in childhood.
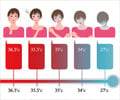
Infants with moderate encephalopathy have a 10% risk of death, and those who survive have a 30% risk of disabilities. 60% of infants with severe encephalopathy die, and many, if not all, survivors are handicapped. Treatment is currently limited to supportive intensive care. Hypothermia has previously been found to be protective against brain injury after asphyxiation in animal models.With a background study on the feasibility of whole-body cooling in a pilot study of neonates with encephalopathy, Dr. Shankaran from Wayne State University and colleagues conducted a randomized, controlled trial to evaluate whether whole-body cooling initiated before 6 hours of age and continued for 72 hours in term infants with encephalopathy would reduce death or disability at 18 to 22 months of age as compared with infants given usual care. The study, funded by the National Institute of Child Health and Human Development (NICHD) and conducted by investigators with the Neonatal Research Network, was published in October 13 issue of the New England Journal of Medicine.
A total of 239 babies with a gestational age of 36 weeks or more were enrolled in the study, and 102 were assigned to hypothermia. Infants were randomized within 6 hours of birth and all had either severe acidosis, or perinatal complications and resuscitation at birth. All had moderate to severe encephalopathy.
During the study, infants were randomly assigned to usual care (control group) or whole-body cooling to an esophageal temperature of 33.5°C for 72 hours, followed by slow re-warming (hypothermia group). Neurodevelopmental outcome was assessed at 18 to 22 months of age. The primary outcome was a combined end point of death or moderate or severe disability.
Infants assigned to the hypothermia group were initially placed on an infant-sized cooling blanket that was pre-cooled to 5° C. An esophageal probe was placed and the infant was covered with a second cooling blanket. Esophageal and skin temperatures were monitored every 15 min for four hours, then every hour for next eight hours, and finally every four hours for the remainder of the cooling period. Infants in the control group were cared for with overhead radiant warmers and had skin temperature maintained between 36.5° C and 37.0° C.
After the study, 44% percent of infants randomized to hypothermia died or had disability compared with 62% of infants in the control group. Twenty-four infants died in the hypothermia group, compared with 38 among the controls, but this was not significant. There was no increase in major disability among survivors; the rate of cerebral palsy was 19% in the hypothermia group as compared with 30% in the control group.
Advertisement