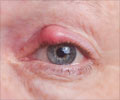
Sickle cell disease is an inherited blood disorder that affects the hemoglobin protein found in red blood cells. Visual loss has been reported in 10- 20% of eyes in patients with this disease, a high figure that may reflect ascertainment bias towards detecting patients with symptoms. Proliferative sickle cell retinopathy (PSR) is the principal contributor to visual loss, but the patients remain asymptomatic unless traumatic complications such as vitreous hemorrhage or retinal detachment (RD) occur.
A recent study, to be published in the November issue of Ophthalmology, details a longitudinal study done over 20 years to describe the incidence, prevalence, and natural history of proliferative sickle cell retinopathy (PSR) in a patient population free from the bias of symptomatic referral, followed from birth.This work, supported by the Wellcome Trust, London, United Kingdom, confirms a greater incidence and severity of PSR in sickle cell disease, and shows that spontaneous regression occurred in 32% of PSR-affected eyes. Permanent visual loss was uncommon in subjects observed up to the age of 26 years. The discrepancy between the frequency of PSR, which concerns the ophthalmologist, and that of visual loss, which concerns the patient, raises a note of caution. It calls into question the justification of routine screening and prophylactic treatment, particularly if it is directed towards prevention of permanent visual loss rather than transient loss from hemorrhage.
Knowledge of the natural history of PSR is essential because the prevention of this visual loss and eye trauma is dependent on the early detection and treatment of proliferative sickle cell retinopathy.