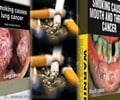
Alcoholic people may die from more of tobacco related infections. However, a new study by the researchers of Mayo Clinic Nicotine Dependence Center had found that it is possible to help cured alcoholics to get over their addictions of tobacco by using individualized nicotine patch therapy.
The findings were published in the July issue of Journal of Studies on Alcohol.The findings show that nicotine patch dosage can be adjusted to provide more effective treatment for smokers with a history of alcoholism. This is good news for recovering alcoholic smokers who have had difficulty stopping smoking after successfully dealing with their drinking.
Alcoholics are statistically heavier smokers and traditionally have had much more trouble stopping smoking using standard-dose nicotine patch therapy. This is the first study to use serum cotinine (a meta-bolic byproduct of nicotine) concentration in smokers with sustained remission from alcohol dependence (greater than 12 months with no relapse for drug or alcohol abuse) to determine the nicotine patch dosages. Investigators hoped to show that maintaining a more consistent level of serum cotinine through customized nicotine replacement therapy would enable more smokers to quit for good, and results from this initial study are positive in this group of smokers.
Investigators individualized the nicotine patch dose based on patients’ serum cotinine levels taken while the patients smoked their usual number of cigarettes. These levels were measured again in mid-study to assist in customization of patch dosage as well as comparison between levels of serum cotinine and ability to abstain from smoking. The study also examined other predictors of treatment response including history of depression, marital status and presence or absence of other smokers in the household. At the end of patch therapy the tobacco abstinence rate was 51 percent. This was comparable to non-alcoholic quit rates but considerably higher than anticipated, since previous studies of recovering alcoholics showed end-of-treatment abstinence levels at about half that.
Source: Newswise