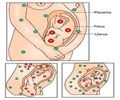
Most women who undergo surgery following an early pregnancy failure are often treated in an operating room, mostly under general anesthesia. However a new study has raised questions about whether women prefer that approach.
Early pregnancy failure - or EPF - occurs in 14 to 19 percent of recognized pregnancies. Cases treated with surgery typically haven't been performed in an office-based setting, even while many other procedures have moved from the OR to the office. Now, a study from the University of Michigan Health System suggests that many women would choose the option of having the procedure done in the relative privacy of an office, without general anesthesia."We found that managing an early pregnancy failure in the office is an acceptable option for many women," says Vanessa K. Dalton, M.D., MPH, lead author of the study, which appeared recently in the journal Obstetrics & Gynecology. "This is a real shift in the way we can approach the care of women with EPF. Many other procedures have moved from the operating room into an ambulatory setting, but for the most part, the management of EPF has not.
"This is a difficult experience for women, and we want to make sure that we are offering them the type of care that works best for them and which they prefer," Dalton says.
Studies indicate that sharp curettage (scraping) and general anesthesia are still common when performing this procedure in the operating room - despite evidence associating them with higher complication rates than suction removal without general anesthesia, says Dalton, assistant professor of obstetrics and gynecology at the U-M Medical School.
The study also found: Costs were more than twice as much in the operating room compared to the office procedures, and the procedure was 80 percent longer. Physician reimbursement did not differ between the two groups.
While the study did not demonstrate that office-based procedures are safer than traditional operating room management, the authors said they are concerned about the four-fold increase in bleeding-related complications in the operating room group in this study. The most likely explanation for this finding was that all but one of the operating room procedures were done under general anesthesia, which may contribute to increased blood loss.
Advertisement
There were no major complications in either group. Further, no office procedure was moved to the operating room or converted to general anesthesia for patient discomfort.
Advertisement
Participants completed a self-administered questionnaire at the time of enrollment. Immediately before discharge, they completed a second questionnaire addressing pain, bleeding and satisfaction with care.
The findings "dispute the notion that current practices are based on patient preferences," Dalton says. "Overall, our institution's experience has been that about half of women choose to have their procedures completed in the office. In the study group, only 25 percent of study participants reported that being asleep for the procedure was highly important. Instead, many participants opted for an office procedure that better meets other needs such as privacy and efficiency.
"It is important that we pay attention to their wishes and offer the services that best meet their needs," she says.
Source: Eurekalert