Genome-wide association studies are a method employed by scientists to identify the genes contributing to human disease. The current Nature study is the first to demonstrate that integrating the information provided by genome-wide association studies with existing datasets of genomic and biological information, such as drug targets, can assist in the discovery of drugs to cure human disease.
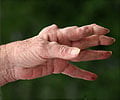
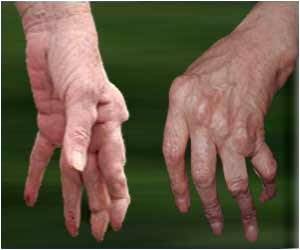
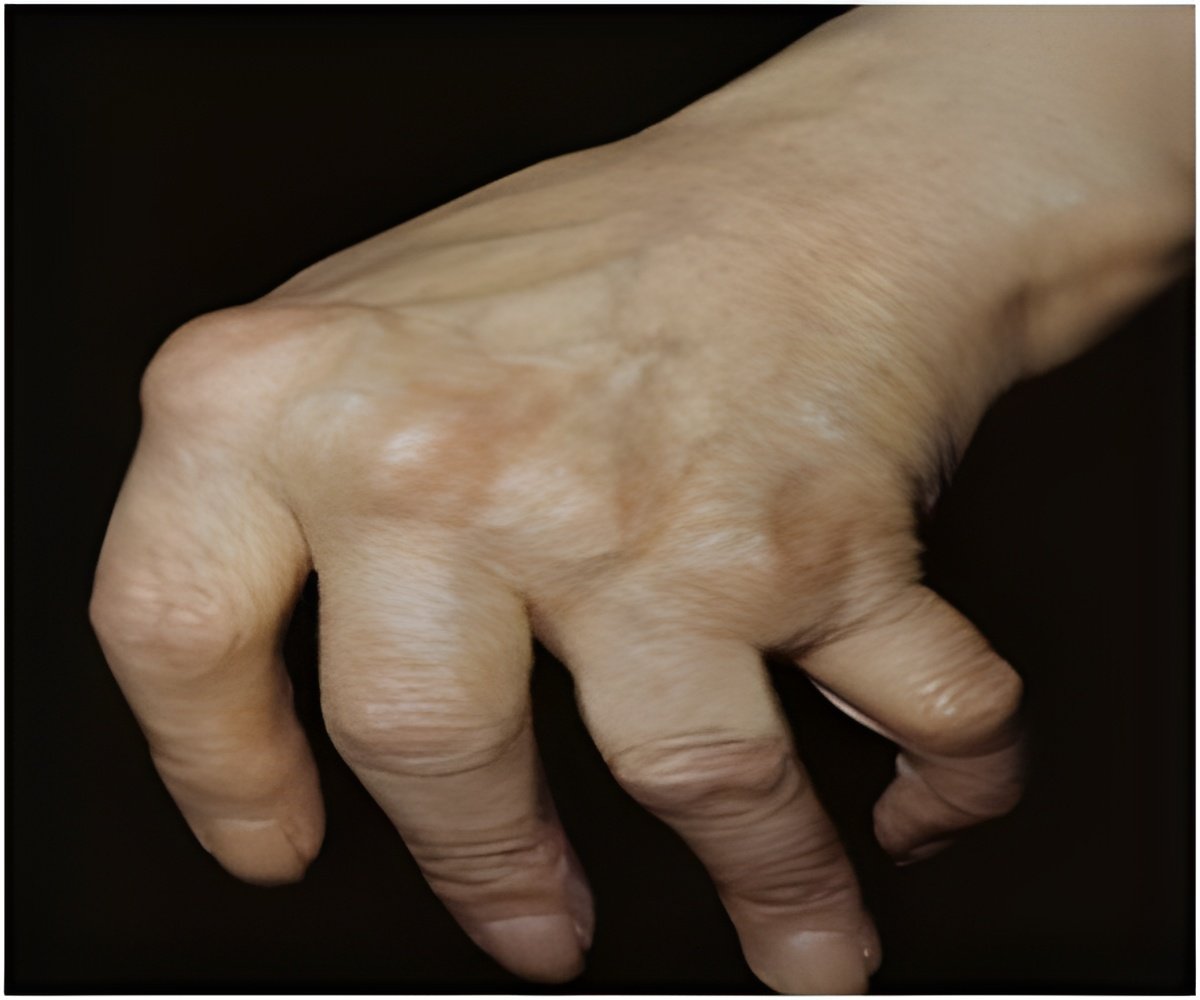
Rheumatoid arthritis is an autoimmune disease leading to inflammation of the joints and affecting 0.5-1% of adults in the developed world. The disease is thought to be caused by a complex combination of genetic and environmental factors and several genes have been shown to be associated with the disease. However, most of the findings were based on single population studies, and no large-scale trans-ethnic study had been carried out to date.
The international team performed a genome-wide association study meta-analysis on a total of over 100,000 subjects of European and Asian descent - 29,880 rheumatoid arthritis patients and 73,758 controls – by analysing around 10 million genetic variants called single nucleotide polymorphism (SNPs). They identified 42 new regions in the genome (loci) that are associated with rheumatoid arthritis, bringing the total number of known rheumatoid arthritis loci to 101.
By conducting bioinformatics studies integrating existing datasets with this new information, the researchers were able to pinpoint 98 genes in these 101 loci that could potentially contribute to the onset of rheumatoid arthritis. By integrating their findings with existing drug databases they demonstrate that these genes indeed possess many overlapping regions with the genes targeted by approved rheumatoid arthritis drugs – although this wasn't known when the drugs were developed. The team identify existing drugs used to treat cancer that also target rheumatoid arthritis genes and could potentially be used as therapy for the disease, such as CDK4/6 inhibitors.
The bioinformatics study also reveals that there is significant overlap between the genes involved in rheumatoid arthritis, human primary immunodeficiency disorders and blood cancers.
Advertisement
"While there are previous anecdotal examples, our study provides a systematic approach by which human genetic data can be efficiently integrated with other biological information to derive biological insights and drug discovery," they add.
Advertisement