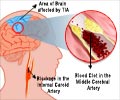
Carotid atherosclerosis is commonest in those with mild peripheral arterial disease in their legs, a condition known as claudication.
In this group the prevalence of silent carotid atherosclerosis is 15%. As they are already under the care of a vascular specialist, they are considered ideal candidates to test for silent carotid atherosclerosis.
But debate rages as to whether to screen for carotid atherosclerosis to stave off a stroke: the Royal College of Physicians does not currently recommend it, but the US Society for Vascular Surgery strongly backs testing in selected groups.
Those found to have severe (70-99%) carotid narrowing on screening are offered surgical treatment (endarterectomy).
But 133 people with claudication would need to be tested to pick up 20 patients eligible for surgery, and this would only prevent a single stroke, at a cost of around £76, 000, say the authors.
Advertisement
But all this effort would still only prevent 231 strokes, even in this high risk group, equivalent to around 0.2% of all 110,000 strokes sustained in 2010, say the authors.
Advertisement
Source-Eurekalert