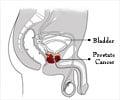
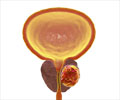
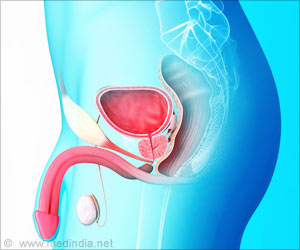
‘Fewer men are being screened, diagnosed and treat for prostate cancer.’
Tweet it Now
To examine the use of diagnostics and treatments for prostate cancer in the years surrounding the USPSTF recommendation, James Kearns, MD, of the University of Washington School of Medicine in Seattle, and his colleagues analyzed MarketScan claims, which capture more than 30 million privately insured patients in the United States. The team looked specifically at information related to PSA testing, prostate biopsy, prostate cancer diagnosis, and definitive local treatment in men aged 40-64 years for the years 2008-2014. Men under age 65 years may benefit most from radiation or surgery for their prostate cancer because prostate cancer tends to cause problems for men many years after diagnosis.In the analysis of approximately 6 million men with a full year of data, PSA testing, prostate biopsy, and prostate cancer detection declined significantly between 2009 and 2014, most notably after 2011. The prostate biopsy rate per 100 patients with a PSA test decreased over the study period from 1.95 to 1.52. Prostate cancer incidence per prostate biopsy increased over the study period from 0.36 to 0.39. Of new prostate cancer diagnoses, the proportion managed with definitive local treatment decreased from 69 percent to 54 percent. Both PSA testing and prostate cancer incidence decreased significantly after 2011.
"In addition to finding decreased prostate cancer screening, we found that fewer men were being diagnosed with prostate cancer, and even fewer men were being treated with surgery or radiation for their prostate cancer. This means that that they are likely choosing active surveillance for low risk prostate cancer," said Dr. Kearns. "This is important because active surveillance has been shown to be safe in many men, and it avoids problems associated with prostate cancer treatment, such as urinary incontinence and erectile dysfunction. Part of the controversy surrounding prostate cancer screening was that men who didn't need surgery or radiation for their prostate cancer were still undergoing those treatments. If those men are instead undergoing active surveillance of their low risk prostate cancer, then the harms of screening will be lower."
In an accompanying editorial, Christopher Filson, MD, MS, of Emory University School of Medicine notes that additional research is needed to determine which men will gain the most value from screening and to identify and correct gaps in the delivery of prostate cancer care to minimize overtreatment while abrogating the incidence of metastatic prostate cancer in the future. "The key will be performing PSA screening--in addition to biopsies and prostate cancer treatment--more intelligently, not more frequently," he writes.
Advertisement


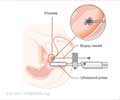
![Prostate Specific Antigen [PSA] & Prostate Cancer Diagnosis Prostate Specific Antigen [PSA] & Prostate Cancer Diagnosis](https://www.medindia.net/images/common/patientinfo/120_100/prostate-specific-antigen.jpg)