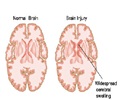
‘The analysis identified four 'clusters', or subtypes, of symptoms of mild traumatic brain injury. Researchers also validated a new tool for assessing the quality-of-life impact of traumatic brain injury.’
Tweet it Now
In print and online, the special issue presents 13 original research studies on TBI in the military, including a special focus on how TBI affects quality of life (QOL). Jason M. Bailie, of the Defense and Veterans Brain Injury Center (DVBIC) and colleagues analyzed patterns of neurobehavioral and psychiatric symptoms in more than 1,300 veterans who had sustained combat-related mild TBI within the past two years. The goal was to develop a classification, or 'taxonomy', of symptoms after mild TBI in military personnel.
The analysis identified four 'clusters', or subtypes, of symptoms. The largest group of veterans - about 38% - had good recovery, with relatively low rates of behavioral and mental health symptoms.
About 22% of veterans had primarily psychiatric symptoms. This included mood symptoms associated with post traumatic stress disorder (PTSD), such as hyperarousal and dissociation or depression. But they were less likely to have cognitive (thinking) difficulties or headaches.
Another 22% had primarily cognitive symptoms and headaches, with few mood problems. The remaining 19% of veterans fell into a 'mixed' subtype, with a combination of mood problems, cognitive complaints, and headaches.
Advertisement
Rael T. Lange, of the DVBIC and colleagues report an evaluation of the 'TBI-QOL' - a new questionnaire for assessing health-related quality of life after TBI. The TBI-QOL evaluates 20 subscales in the areas of physical and emotional health, cognition, and social participation.
Advertisement
Veterans with TBI scored worse than the other groups on ten out of 14 subscales. The differences were largest in areas reflecting cognitive function, grief and loss, pain interfering with daily activities, and headache. Somewhat surprisingly, the differences were not as great for symptoms of anxiety and depression.
Source-Eurekalert