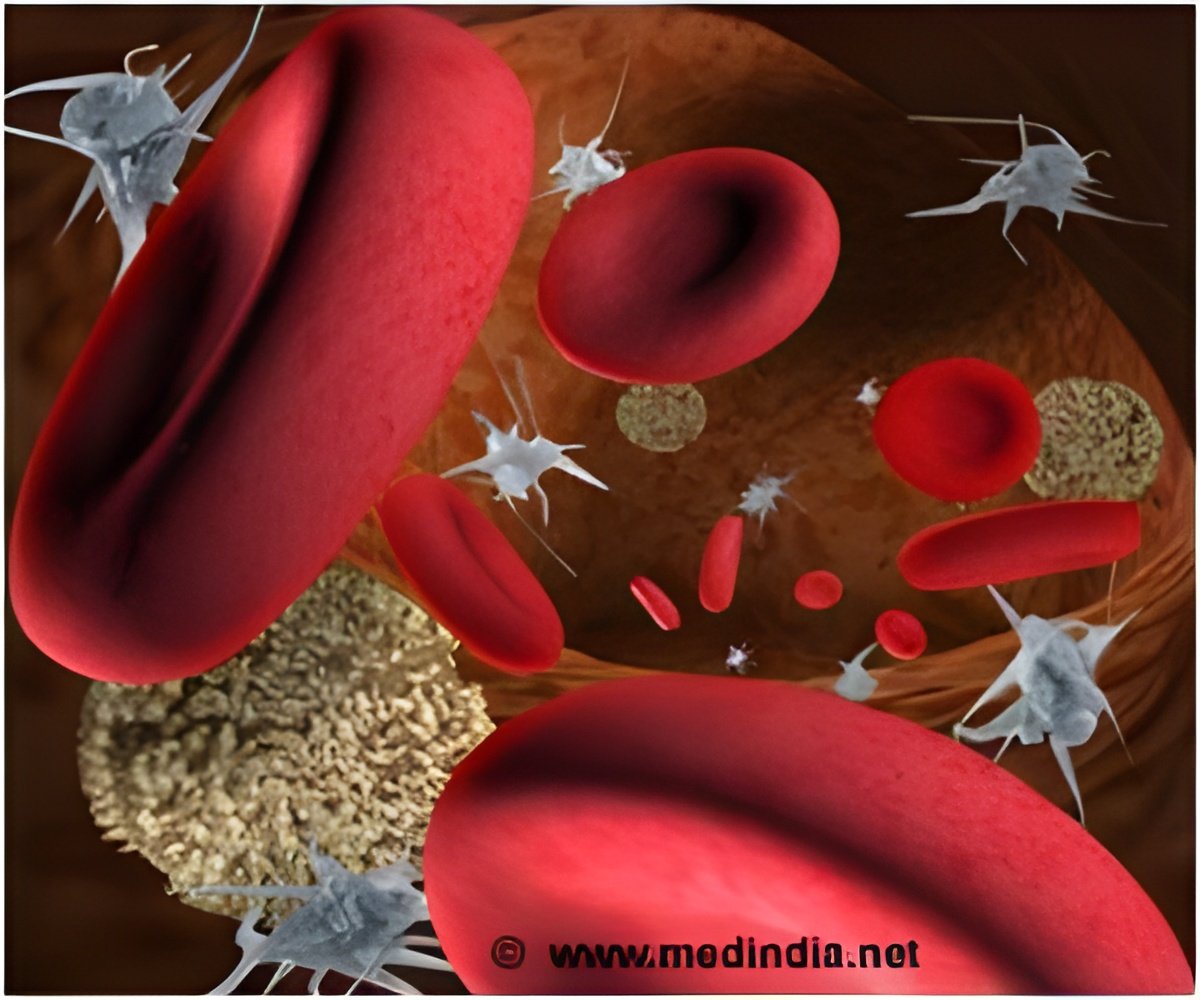
‘In atherosclerosis, the injury signal is triggered by the deposition of cholesterol, which induces the migration of patrolling monocytes to the site. Once in the vessel wall, the monocytes differentiate to macrophages, which are specialized in 'engulfing' injurious material, such as the accumulated cholesterol.
’
Tweet it Now
Our immune system involves circulating leukocytes (white blood cells) with specialized functions. One population consists of inflammatory monocytes that are released rapidly to the circulation in response to injury and generate an immune response at the injury site. But there is another monocyte population tasked with "the surveillance of the blood-vessel interior, giving rise to the name blood-patrolling monocytes," explained Dr. Arroyo. These monocytes rarely migrate to sites of tissue injury, and therefore their role in inflammation is less known.
Now, in the Nature Communications study, the CNIC team has conducted an in-depth analysis of the function of patrolling monocytes in inflammatory disease and the mechanisms that regulate their vascular surveillance activity. As a model, the researchers studied the inflammatory process of atherosclerosis. In atherosclerosis, the injury signal is triggered by the deposition of cholesterol, which induces the migration of inflammatory monocytes and, to a lesser extent, patrolling monocytes. Once in the vessel wall, the monocytes differentiate to macrophages, which are specialized in 'engulfing' injurious material, such as the accumulated cholesterol.
First author Cristina Clemente explained that "The first things we observed were that early atherosclerotic plaque in mice lacking MT4-MMP (a member of the matrix metalloprotease family) accumulated more macrophages and that atherosclerosis was accelerated when these mice were fed a high-fat diet." The researcher also observed that early lesions in mice lacking MT4-MMP selectively accumulated more patrolling monocytes, whereas inflammatory monocytes were recruited as normal.
Clemente added that "Macrophages derived from the patrolling monocytes incorporated more fat and showed better survival than those derived from inflammatory monocytes." But when the MT4-MMP-deficient mice were treated with the CCR5 inhibitor Maraviroc, used to treat patients with HIV, the migration of patrolling monocytes to atherosclerotic plaques was blocked, preventing the macrophage accumulation and accelerated atherosclerosis.
Advertisement
The authors also identified that MT4-MMP can cut integrin £\M, a crucial leukocyte adhesion receptor. Thus, in the absence of the protease, this receptor accumulates on the surface of patrolling monocytes. Through collaboration with CNIC colleague Cristina Rus, the research team used intravital microscopy to visualize the surveillance activity of patrolling monocytes, detecting increased numbers of these cells in inflamed vessels of mice lacking MT4-MMP.
Advertisement