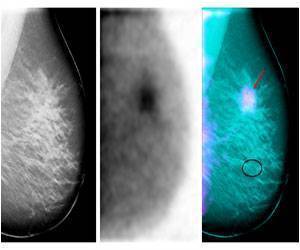
Prof. Emiel J. Rutgers of The Netherlands Cancer Institute-Antoni Van Leeuwenhoekziekenhuis in Amsterdam, the EORTC Breast Cancer Group, and principal investigator of this study says, "Sentinel node biopsy has become the standard procedure for assessing axillary lymph node status for cN0 breast cancer patients. At the start of this trial the question was whether axillary lymph node dissection should remain the standard treatment in case of a tumor positive sentinel node."
From 2001 to 2010, 4806 patients who were diagnosed with invasive breast cancer were enrolled in this phase III non-inferiority trial, and randomized for their axillary treatment in case the sentinel node biopsy was positive. Of these, 3131 patients had negative biopsies and 250 patients had a different sentinel node outcome. Thus, out of 1425 patients with positive node, axillary lymph node dissection was to be used in 744 patients, and axillary radiotherapy in 681 patients.
Dr. Geertjan van Tienhoven of the Academisch Medisch Centrum - Universiteit van Amsterdam and principal investigator on behalf of the EORTC Radiation Oncology Group says, "Although axillary lymph node dissection provides excellent regional control, it was known to cause harmful side effects. Axillary radiotherapy instead of axillary lymph node dissection was hypothesized to provide comparable regional control and perhaps fewer side effects in this particular group of patients."
The primary endpoint of this EORTC trial was 5-year axillary recurrence rate. At a median follow up of 6.1 years, this rate was 0.54% (4 out of 744 patients) after axillary lymph node dissection and 1.03% (7 out of 681 patients) after axillary radiotherapy. Due to the unexpectedly low number of events, the non-inferiority test was underpowered. The axillary recurrence rate for patients with a negative sentinel node biopsy was 0.8% (25 out of 3131 patients).
Secondary endpoints were overall survival, disease-free survival, quality of life, shoulder movement and lymphoedema at one and five years. No significant differences in overall or disease free survival were observed between the two treatment arms. Five year estimates for overall survival were 93.3% for the arm receiving axillary lymph node dissection and 92.5% for patients in the axillary radiotherapy arm (p=0.34), and fordisease-free survival the five year estimates were 86.9% for axillary lymph node dissection and 82.6% for axillary radiotherapy (p=0.18).
Advertisement
Both results were compatible with two patient reported quality of life items in the arm symptom scale: swelling, where patients in the axillary radiotherapy fared better, and mobility, where patients in the axillary lymph node dissection arm fared better.
Advertisement
Source-Eurekalert