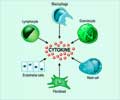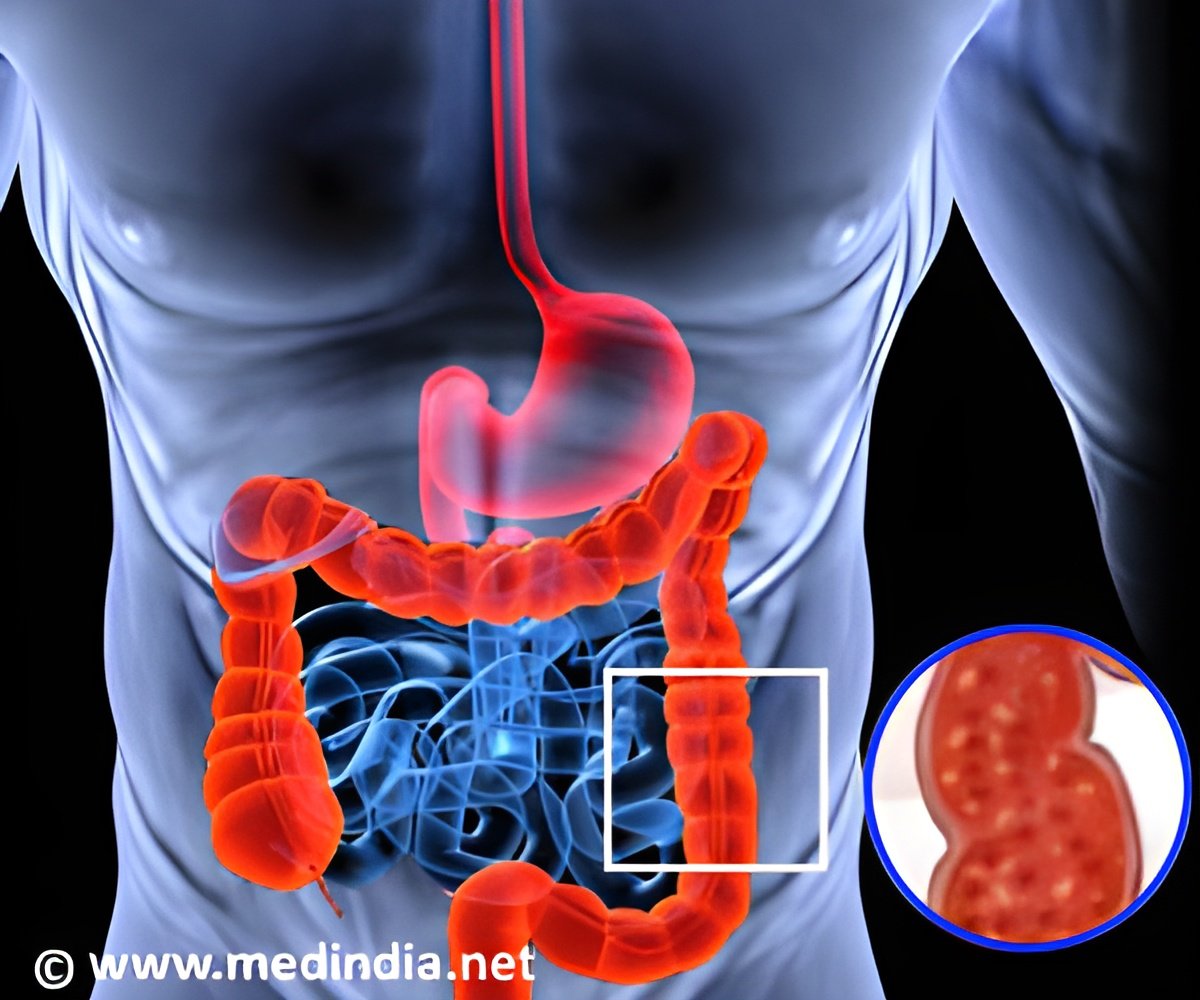
The most damaging strains of H. pylori make a molecular syringe called the cagT4SS, through which bacterial products are injected into cells of the stomach lining. In vitro work using human gastric epithelial cell lines showed that this activates chemical pathways to suppress hβD1 production. These activated pathways are also involved in the stimulation of an inflammatory response, meaning that these H. pylori strains are able to survive and colonise more abundantly, while continuing to cause tissue damage over many decades. Previous research suggests that chronic inflammation of the stomach lining is strongly linked to gastric cancer.
It is estimated that half of the world's population have H. pylori in the mucosal lining of their stomach. For most people the infection is asymptomatic, although 1-2 per cent of those infected will develop gastric cancer. Survival rates for this disease remain low, as diagnosis is often very late, when the cancer is at an advanced stage.
Katie Cook, who is presenting this work says, "To identify people who are likely to suffer from stomach cancer we need to understand how H. pylori interacts with the cells of the stomach lining. Because our research is patient-focused we know that our findings are directly relevant.
"We hope to combine this work with that being carried out by our colleagues in order to develop a diagnostic test to predict the future risk of gastric cancer development."
Advertisement