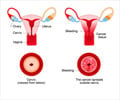
Three studies published on bmj.com today examine the merits of conservative versus aggressive treatment policies of women with low-grade abnormal results detected by cervical screening.
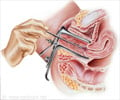
Together they form the Trial of Management of Borderline and Other Low-grade Abnormal Smears (TOMBOLA).The first finds no benefit in referring these women for colposcopy (a detailed inspection of the cervix to detect pre-cancerous cells) compared to regular surveillance.
A second paper also questions the benefit of immediate treatment to remove abnormal tissue from the cervix (a procedure known as large loop excision) over the more conservative strategy of taking small tissue samples (biopsies) and recalling women for treatment only if pre-cancerous lesions are confirmed.
Finally, a cost effectiveness study shows that immediate colposcopy is no more, or no less, cost effective than regular surveillance.
The findings are based on data from about 4,500 women aged 20-59 from two regions of Scotland (Grampian and Tayside) and one of England (Nottingham) with borderline or low-grade abnormal smears detected after NHS cervical screening examinations.
In the first study, women were randomised to either repeat smears or to immediate referral for colposcopy. All women were tracked for three years and underwent a colposcopic examination at the end of the study.
Advertisement
In the second study, women were randomised to either immediate large loop excision or up to four biopsies with recall for treatment if necessary. Again, women were tracked for three years and underwent a colposcopic examination at the end of the study.
Advertisement
A cost effectiveness study shows that, taking into account costs, outcomes, and quality of life, follow-up by immediate colposcopy is no more and no less cost effective than follow-up by regular surveillance. The authors conclude that “there is no compelling economic reason to favour any one follow-up method over either of the others.”
The dilemma of choosing between conservative and aggressive policies remains, adds Professor Eduardo Franco of McGill University in an accompanying editorial. Further analyses and secondary economic evaluations of the TOMBOLA data may help policy makers fully appreciate the evidence from this landmark study, he says.
Source-BMJ
LIN