Highlights:
- An aggressive stem cell transplant regime to treat systemic sclerosis, a severe form of scleroderma that affects the internal organs, significantly improved survival rates among patients.
- In this study, high-dose chemotherapy and radiation were given to patients to deplete the bone marrow and was followed by autologous Stem Cell Transplant (with cells that were taken out prior to the study and treated) or 12 doses of the immunosuppressant drug, cyclophosphamide.
Scleroderma
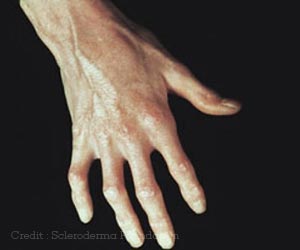
Scleroderma is an autoimmune disease that is characterized by hardening of the skin and connective tissues. Scleroderma can be localized or systemic. The localized form of the disease is relatively mild and usually affects only in a few parts of the skin or muscles, and rarely spreads elsewhere. Systemic scleroderma or sclerosis is a disorder of the blood vessels (vasculopathy), low-grade inflammation and development of excess fibrous connective tissue in the skin and internal organs. This form of the disease is debilitating and potentially lethal, and treatment options available for it are limited. People with systemic sclerosis try to cope by managing the symptoms. They may take antirheumatic drugs and immunosuppressant drugs like cyclophosphamide for this purpose, but none of these medications have been proven to provide long-term benefits."Scleroderma hardens the skin and connective tissues and in its severe form leads to fatal organ failure, most often the lungs" said lead author Keith Sullivan, Professor of Medicine and Cellular Therapy at Duke University. "In these severe cases, conventional drug therapies are not very effective long-term, so new approaches are a priority."
Earlier use of stem cell transplant for systemic sclerosis
In two clinical trials performed earlier, patients received non-myeloablative HSCT, where a less intensive treatment of chemotherapy was used without any radiation; at these doses, the bone marrow was not destroyed completely. These studies showed that stem cell transplant used this way with reduced-intensity chemotherapy improved survival in severe scleroderma. The drawback of this kind of treatment was that the disease often returned and patient safety remained a concern. Hence, the clinical practice of using conventional immunosuppressive drug treatment continued to be the standard of care in the US.Scleroderma Cyclophosphamide or Transplantation (SCOT) trial: Does myeloablative transplant regimen offer better long-term outcomes?
The SCOT trial compared the safety and potential benefits of the two treatment regimens for systemic sclerosis, myeloablative stem cell transplant and immunosuppressive treatment.There were 75 participants with diffuse systemic sclerosis with lung or kidney involvement included in the study.
In the patients who received myeloablative autologous hematopoietic stem cell transplant (HSCT), the doctors collected the participants’ blood-forming stem cells. Chemotherapy and radiation were then employed to destroy the normal and cancerous cells in the bone marrow, followed by transplantation of the person’s own blood-forming stem cells to reconstitute the marrow and immune system.
Thirty six scleroderma patients were assigned in the study to receive myeloablative autologous HSCT. On the other hand, thirty nine patients were randomized to receive one year of treatment with monthly doses of intravenous cyclophosphamide, a conventional immunosuppressing treatment for severe scleroderma.
The results of the study were as follows:
- Participants who received a transplant experienced significantly better outcomes overall than those who received cyclophosphamide: 67 percent of 1,404 pairwise comparisons favored transplant vs. 33 percent favoring cyclophosphamide.
- In addition, fewer transplant recipients resumed the use of antirheumatic drugs for progression of their scleroderma (9 percent) as compared to 44 percent of participants in the cyclophosphamide group.
- The overall survival at 72 months was significantly better in the transplant group (86 percent after transplant vs. 51 percent after cyclophosphamide).
Adverse effects of the Treatments
The participants in both study arms experienced known short-term risks, such as infections and low blood cell counts. Although the overall infection rates in both the arms were similar, transplant recipients were more prone to infections caused by varicella zoster, the virus that causes chickenpox and shingles.Survival rates
- During the study, lesser patients in the transplant arm died (7), compared to the cyclophosphamide arm (14); this included deaths that occurred due to disease progression (2 with transplant versus 11 with cyclophosphamide).
- Equal number of deaths (3) occurred in both arms among those who did not complete the treatment.
- However, the treatment-related deaths were two in number in the transplant category and none in the cyclophosphamide category.
References:
- KM Sullivan et al. Myeloablative autologous stem cell transplantation for severe scleroderma. N Engl J Med 2018; 378:35-47January 4, 2018. DOI: 10.1056/NEJMoa1703327
- Stem cell transplant for severe scleroderma improves survival, quality of life - (https://www.nih.gov/news-events/news-releases/stem-cell-transplant-severe-scleroderma-improves-survival-quality-life)
Source-Medindia