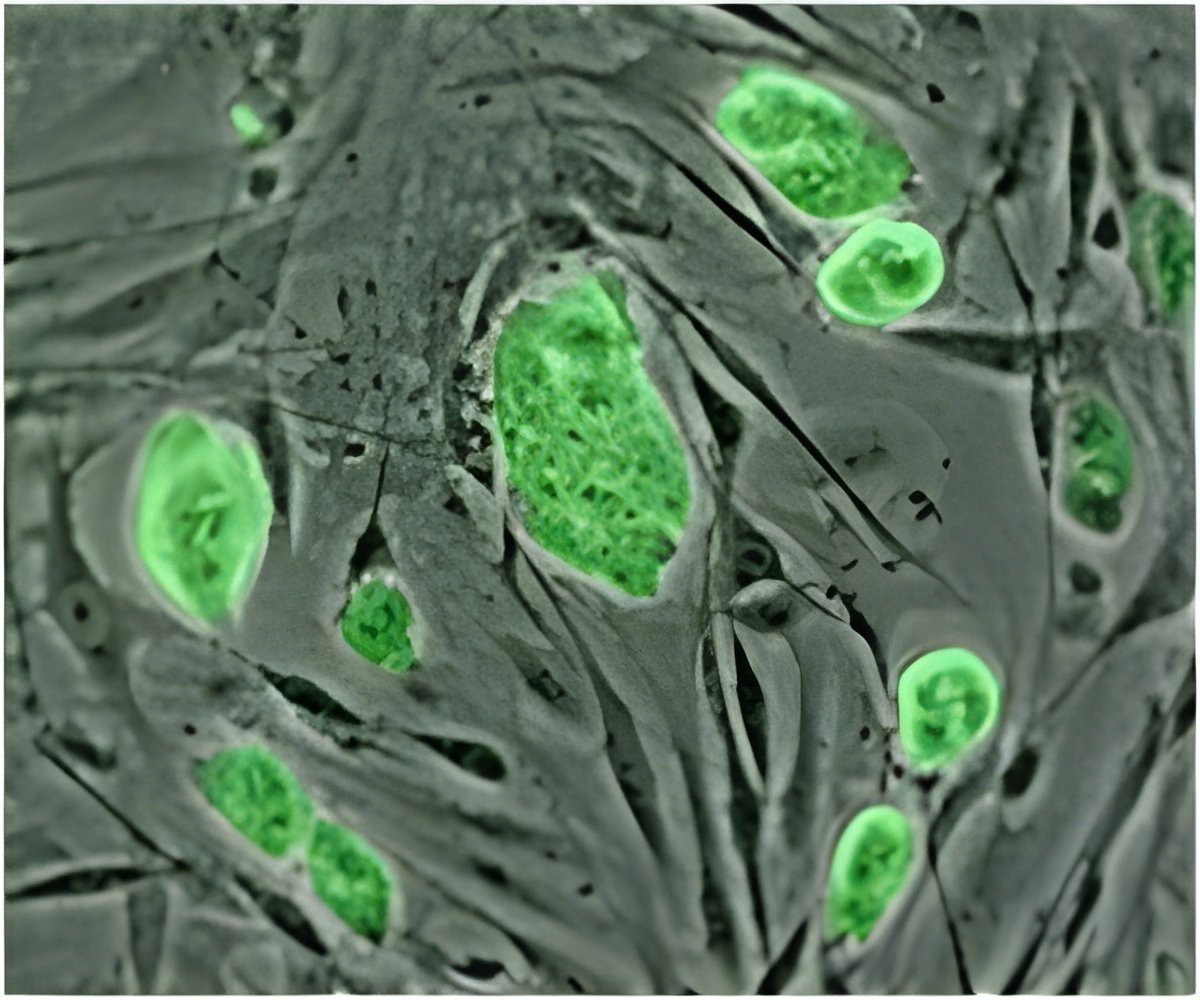
Starting with human embryonic stem cells, UCSF researchers led by Mark Anderson, MD, PhD, an immunologist, and Matthias Hebrok, PhD, a stem-cell researcher and the director of the UCSF Diabetes Center, used a unique combination of growth factors to shape the developmental trajectory of the cells, and eventually hit upon a formula that yielded functional thymus tissue.
The result, reported in the May 16, 2013 online edition of the journal Cell Stem Cell, is functioning tissue that nurtures the growth and development of the white blood cells known as T cells. T cells are a central immune cell population that responds to specific disease pathogens and also prevents the immune system from attacking the body's own tissues.
The thymus might be a bit obscure to the layperson — it's a small gland at the top of the chest beneath the breastbone — but it is in no way expendable, as individuals with defective thymus function succumb to infection early in life.
Given the invasive nature of cell therapy, which remains completely experimental, the first treatments using laboratory-derived thymus tissue would likely be studied in patients with fatal diseases for which there are no effective treatments, Anderson said. For example, one early treatment might be for the genetic disease DeGeorge syndrome, in which some newborns are born without a thymus gland and die in infancy.
Source-Eurekalert