Because the anti-seizure drug is familiar to doctors and has a well-understood safety profile, clinical trials could begin immediately to see whether it can help patients with AT deficiency, said senior author David H. Perlmutter, M.D., physician-in-chief and scientific director, Children's Hospital, and Vira I. Heinz Professor and Chair of the Department of Pediatrics, Pitt School of Medicine.
In the liver disorder, a gene mutation leads to an abnormal protein, dubbed ATZ.
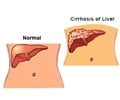
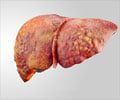
"These aggregates of ATZ accumulate in the liver cells and eventually lead to scarring, or fibrosis, of the organ and set the stage for tumor development," Perlmutter said.
"The disease sometimes doesn't show itself until adulthood, when the liver starts to fail due to cirrhosis or cancer."
Perlmutter and his colleagues treated an ATZ cell line with carbamazepine and found that it could enhance a natural cellular pathway called autophagy, or self-digestion. It caused a marked decrease in ATZ because the abnormal proteins were degraded more quickly via autophagy.
Advertisement
"The most amazing finding was that the drug reversed the fibrosis in the livers of the mice and, after two weeks of treatment, the liver tissue resembled that of a healthy mouse."
Advertisement
Source-ANI