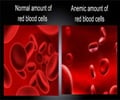
Beta-thalassaemia occurs when a patient is unable to produce enough beta-globin, a component in haemoglobin, which is used by red blood cells to transport oxygen around the body.
The body's organs, depriving of sufficient oxygen, can be badly damaged without regular, and lifelong, blood transfusions.
The alternative treatment is bone marrow transplant, but only a small minority of patients have access to this because of difficulties in finding the right type of donor.
Reporting in the science journal Nature, doctors led by Philippe Leboulch of Harvard Medical School, used a virus as a "Trojan horse" to deliver a slice of DNA into cells which corrected for the flawed beta-LCR gene.
"At present, approximately three years post-transplantation, the biological and clinical evolution is remarkable and the patient's quality of life is good," they said.
Advertisement
Leboulch sounded a note of caution, saying that the Trojan horse, a type of virus that is called a lentivirus, may have altered the function of a gene that controls the behaviour of blood stem cells.
Advertisement
At present, the increase is benign, but in theory it could be a prelude to leukaemia, which is a factor for doctors weighing whether to use the therapy on other patients.
Gene therapy burst on the medical scene in the late 1990s, offering the allure of blocking or reversing inherited disease.
So far, though, successes have been few, limited to single-gene disorders -- as opposed to complex multi-gene disorders that account for the commonest diseases -- and they have been carried out under tightly-controlled lab conditions.
They include six children, blighted by a retinal disease called Leber's congenital amaurosis and two adults with a so-called myeloid disorder, a disease of white blood cells.
But there have also been setbacks, including the tragic death of an 18-year-old US volunteer, Jesse Gelsinger, in 1999, and the development of cancer among two French children treated for "bubble baby" syndrome, a chronic lack of immune defences.
Investigations into these failures have focussed especially on the virus used to deliver the gene, amid suspicions that the vector -- even if disabled -- may unleash an uncontrolled response from the immune system.
Source-AFP