Nadeem Khan, PhD, first author said, "This is a major step forward. It brings EPR oximetry technique to the forefront of biomedical research for clinical applications."
Oxygen is necessary to sustain life. A certain level of oxygen in a cell or tissue is necessary to maintain the generation of energy by cells. Oxygen also plays a key role in the development and treatment of various diseases.
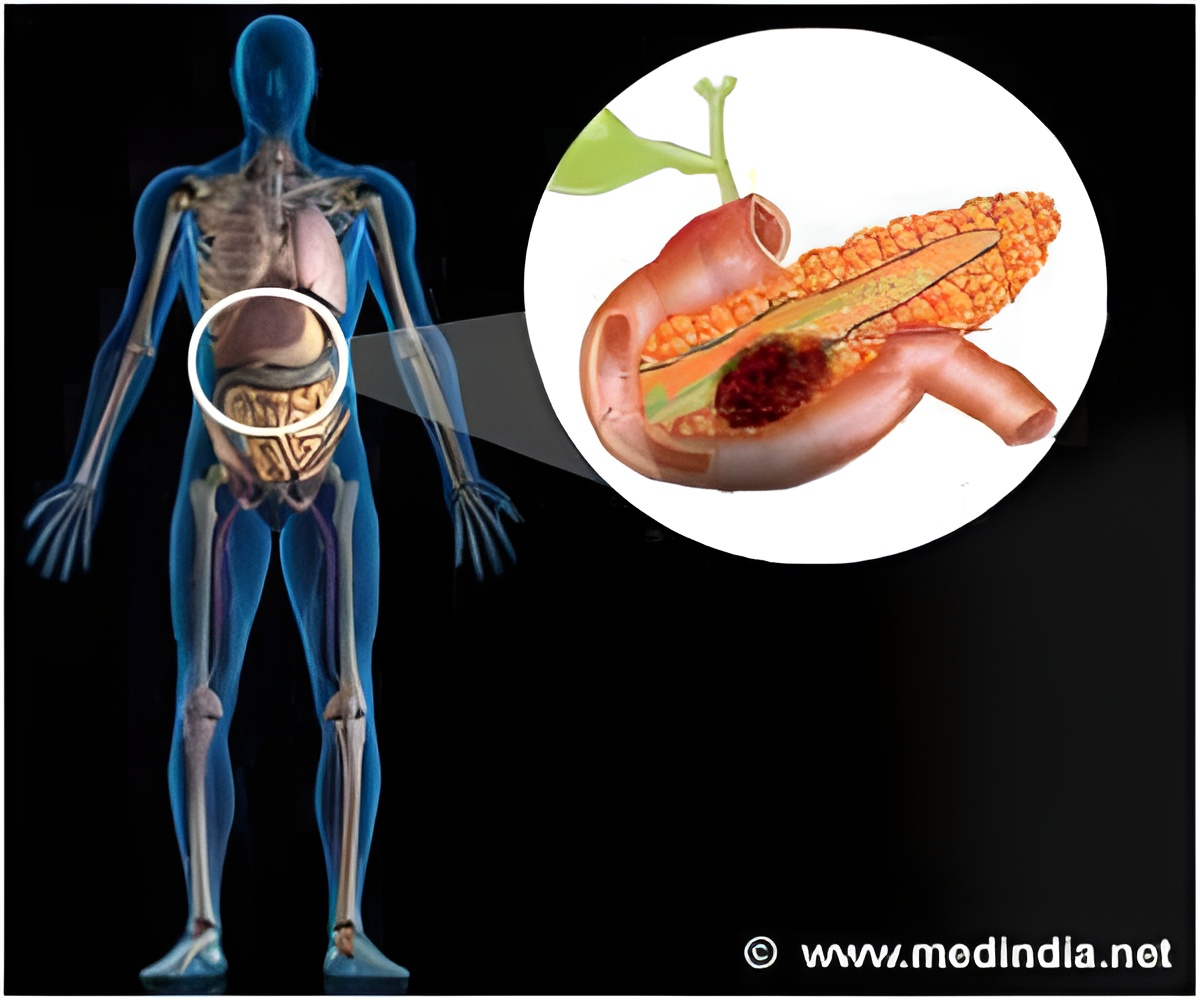
The effectiveness of several therapies also depends on the oxygen levels in a malignancy. For example, a very low level of oxygen in cancer is known to develop aggressive phenotypes, varies with the growth of tumors, and also compromises the effectiveness of chemotherapy and radiation. Hence, it is very important to directly measure oxygen levels to understand disease progression, develop strategies to improve oxygen levels, and optimize the efficacy of therapies.
Oxygen measurement in deep-sited tissue has been a challenge for several techniques, which has unfortunately limited the understanding of various pathologies in large animals and humans. To solve the problem, Dartmouth's EPR team developed implantable resonators made of thin nonmagnetic copper wire to facilitate direct and repeated measurement of tissue oxygenation at any depth from the surface. In their most recent experiment, which demonstrated the efficacy of in vivo EPR oximetry, they used a one-time implementation of the oxygen probes in the brain of a rabbit and successfully monitored oxygen levels for several weeks.
"Other than the implantation, which is done under anesthesia, the rest of the procedure for oxygen measurements is entirely non-invasive. We anticipate that a better understanding of oxygen levels in stroke, for instance, will guide the development of strategies to significantly improve oxygen levels in the ischemic regions of the brain and thereby improve outcomes," explained Khan.
Advertisement
Advertisement