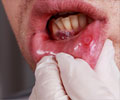
The research is particularly relevant to a rare but devastating cancer of children and young adults known as NUT midline carcinoma (NMC) - a disease so obstinate that no potential therapy for it has ever reached the stage of being tested in a clinical trial.
"In recent years, it has become clear that being able to control gene activity in cancer - manipulating which genes are 'on' or 'off' - can be a high-impact approach to the disease. If you can switch off a cancer cell's growth genes, the cell will die. Alternatively, switching on a tissue gene can cause a cancer cell to become a more normal tissue cell," Nature quoted the study's senior author, Dr. James Bradner, as saying.
In the study, Bradner's lab synthesized a molecule that has both effects: by blocking a specific abnormal protein in NUT midline carcinoma cells, it stops them from dividing so prolifically and makes them 'forget' they're cancer cells and start appearing more like normal cells.
The assembled molecule affects the cell's multi-layered apparatus for controlling gene activity, a set of structures collectively known as the epigenome.
Vast portions of each gene play a regulatory role, dictating whether the gene is active, busily sending orders for new proteins, or inactive, and temporarily at rest.
Advertisement
The instructions themselves take the form of "bookmarks," substances placed on the chromatin by so-called epigenetic "writer" proteins.
Advertisement
Both types of proteins have successfully been disabled by scientists, using molecules made in the lab or taken from nature.
Their success has sparked intense interest in the development of anti-cancer therapies that work by blocking such proteins.
A third variety of epigenetic proteins - potentially the most appealing as therapeutic targets, because they switch genes on or off by "reading" the bookmarks - has received scant scientific attention.
Bradner and his colleagues turned to this little-explored corner of biology by focusing on NMC cells.
The disease is caused by a chromosomal "translocation," in which two genes from different chromosomes become connected and give rise to an abnormal, fused protein known as BRD4-NUT.
A review of the scientific literature suggested that some members of the benzodiazepine family of drugs, which includes Valium, Xanax and Ativan, are active against "bromodomain" proteins such as BRD4.
With that as a clue, Bradner and his Dana-Farber colleague Dr. Jun Qi created an array of molecules to see if any inhibited a "reader" protein of the BRD4-NUT gene.
One did, quite convincingly - a hybrid molecule, which researchers named JQ1, for Qi.
"The activity of the molecule was remarkable. All the mice that received JQ1 lived; all that did not, died," said Bradner.
"This research further illustrates the promise of personalized medicine," Bradner remarks, "which is the ability to deliver selected molecules to cancer-causing proteins to stop the cancer process while producing a minimum of residual side effects. The development of JQ1 or similar molecule into a drug may produce the first therapy specifically designed for patients with NMC."
The study has been published by the journal Nature.
Source-ANI