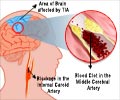
A new research indicates that women who have migraine head aches and associated visual symptom(aura) have a higher risk of getting a stroke compared to women without such complications .Other factors like smoking and oral contraceptives can further enhance the problem. Even recent onset of headaches can increase the risk. The study was reported in Stroke reported in Stroke: Journal of the American Heart Association.
Women with recent onset of probable migraine with visual symptoms (within the prior year) were almost seven times more likely to have a stroke compared to women with no history of migraine,” said Steven Kittner, M.D., M.P.H., senior author of the study and staff physician at Baltimore Veterans Affairs (VA) Medical Center. “Eight percent of stroke cases had onset of probable migraine with visual symptoms in the prior year compared to one percent of controls.“Second, and probably the most important finding, women who had probable migraine with visual symptoms who also smoked and used oral contraceptives had seven times the risk of stroke than women who had probable migraine with visual symptoms alone.”
Migraine and stroke share some common risk factors, including high blood pressure and patent foramen ovale (PFO); both have a hereditary basis. While a baby grows in the womb, he or she has a normal opening between the heart’s left and right atria (upper chambers). If this opening doesn’t close naturally soon after the birth, the hole is called PFO.
Furthermore, migraine has long been regarded as a risk factor for ischemic stroke (stroke caused by a blot clot blocking blood flow to the brain). Few prior studies have addressed the different potential reasons for an association between migraine and stroke.
Researchers analyzed stroke incidence among 386 women 15-to 49-years-old with a first ischemic stroke and 614 women of similar ages and ethnicities who had not had stroke. Based on their responses to a questionnaire, the women were classified into three categories: having no migraine; probable migraine without visual aura; or probable migraine with visual aura.
Kittner and colleagues also reported that, compared to women with no history of migraine, women with probable migraine with visual symptoms had a 1.5 greater risk of ischemic stroke.
Advertisement
However, neurologists and other doctors should encourage their patients who have migraine with associated visual symptoms to minimize other stroke risk factors, he said.
Advertisement
“Other investigators should confirm our findings of an increased risk of stroke associated with recent onset of probable migraine with visual symptoms.”
Source-Eurekalert
BIN/J