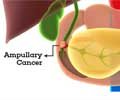
Biliary atresia progresses to end-stage liver disease (cirrhosis) in more than 70 percent of affected children and is the leading indication for pediatric liver transplantation in the world, accounting for about 50 percent of liver transplants in children. Hepatoportoenterostomy (surgery to improve bile drainage) results in successful bile drainage in only about half of patients with biliary atresia treated in the United States, underscoring the need for additional therapies to improve survival without liver transplantation, according to background information in the article. There have been conflicting reports regarding the effectiveness of the use of corticosteroids to improve bile flow following surgery.
Jorge A. Bezerra, M.D., of Cincinnati Children's Hospital Medical Center, Cincinnati, and colleagues randomly assigned 140 infants (average age, 2.3 months) to receive high-dose steroid therapy or placebo following surgery to improve bile drainage.
The researchers found that the proportion of infants with improved bile drainage was not significantly improved by steroids at 6 months following surgery (58.6 percent of steroids group vs 48.6 percent of placebo group). The adjusted absolute risk difference was 8.7 percent.
Survival without liver transplantation at 2 years of age for infants treated with steroids was nearly identical to those who received placebo (58.7 percent vs. 59.4 percent). Serious adverse events were com¬mon in both treatment groups (81.4 percent for steroids vs 80.0 percent for placebo); however, infants treated with steroids experienced their first serious adverse events earlier than those receiving placebo.
"Based on the strength of the evidence, the addition of high-dose steroids as an adjuvant [supplemental] treatment for infants with biliary atresia after hepatoportoenterostomy cannot be recommended," the authors write.
Advertisement