Dabigatran etexilate (Pradaxa®) is an oral anticoagulant (blood thinner) recently approved by the US FDA to lower the risk of stroke and prevent systemic embolism in persons with atrial fibrillation that is not heart valve related. It is an attractive alternative to other drugs used for atrial fibrillation because it can be taken orally, does not require repeated blood testing, and has little interaction with other drugs or food. Coagulation involves many steps, and anticoagulant drugs inhibit various steps in the coagulation cascade. Platelet function inhibitors, such as clopidogrel, and vitamin K blockers, such as warfarin, act at earlier steps in this cascade and there are readily available means to counter their effects. Dabigatran is a synthetic direct thrombin inhibitor that acts at the end of the cascade, and unfortunately, to date no agent is effective in reversing the drug's effects.
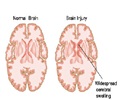
The authors review the case of an 83-year-old man, who fell from ground level and was evaluated for his injuries at the emergency department. Initially, the patient was fully alert and oriented and could respond to all verbal commands; his neurological exam yielded normal findings. Computed tomography (CT) scans revealed small, superficial areas of hemorrhage in his right temporal lobe and left temporal and parietal lobes. Within two hours after the man had entered the emergency department, his neurological state began to deteriorate rapidly, and repeat CT scanning showed extensive progression of brain hemorrhaging. Medical interventions, including intravenous administration of fluids, mannitol, hypertonic saline, and recombinant factor VIIa, proved ineffective at stopping the bleeding. Unfortunately, the patient's neurological state continued to decline rapidly and he lapsed into a deep coma. Six hours after admission, final CT scans showed hemorrhage nearly filling the left hemisphere of the brain and extensive right-sided brain hemorrhage as well. Because it was clear that the patient could not survive this neurological injury, he was given palliative care. The man died soon afterward.
The authors point out that patients treated with dabigatran often are elderly and thus more likely to have problems with balance and falling. In this group of patients, a minor head trauma could result in intracranial hemorrhage with catastrophic outcome. Currently there is no effective medical antidote for dabigatran. The only recognized intervention is early initiation of renal dialysis to speed elimination of the drug, although such clearance may take 12 or more hours. Animal studies also suggest the use of high-dose prothrombin complex concentrate; while it has proved effective in mice, it still needs study in humans. Since the use of direct thrombin inhibitors for treatment of atrial fibrillation and other blood clotting disorders is expected to increase, medical providers and patients taking these drugs need to be aware of the risk for catastrophic hemorrhaging and the importance of rapid assessment and intervention after even seemingly minor trauma.
Source-Eurekalert