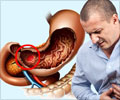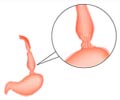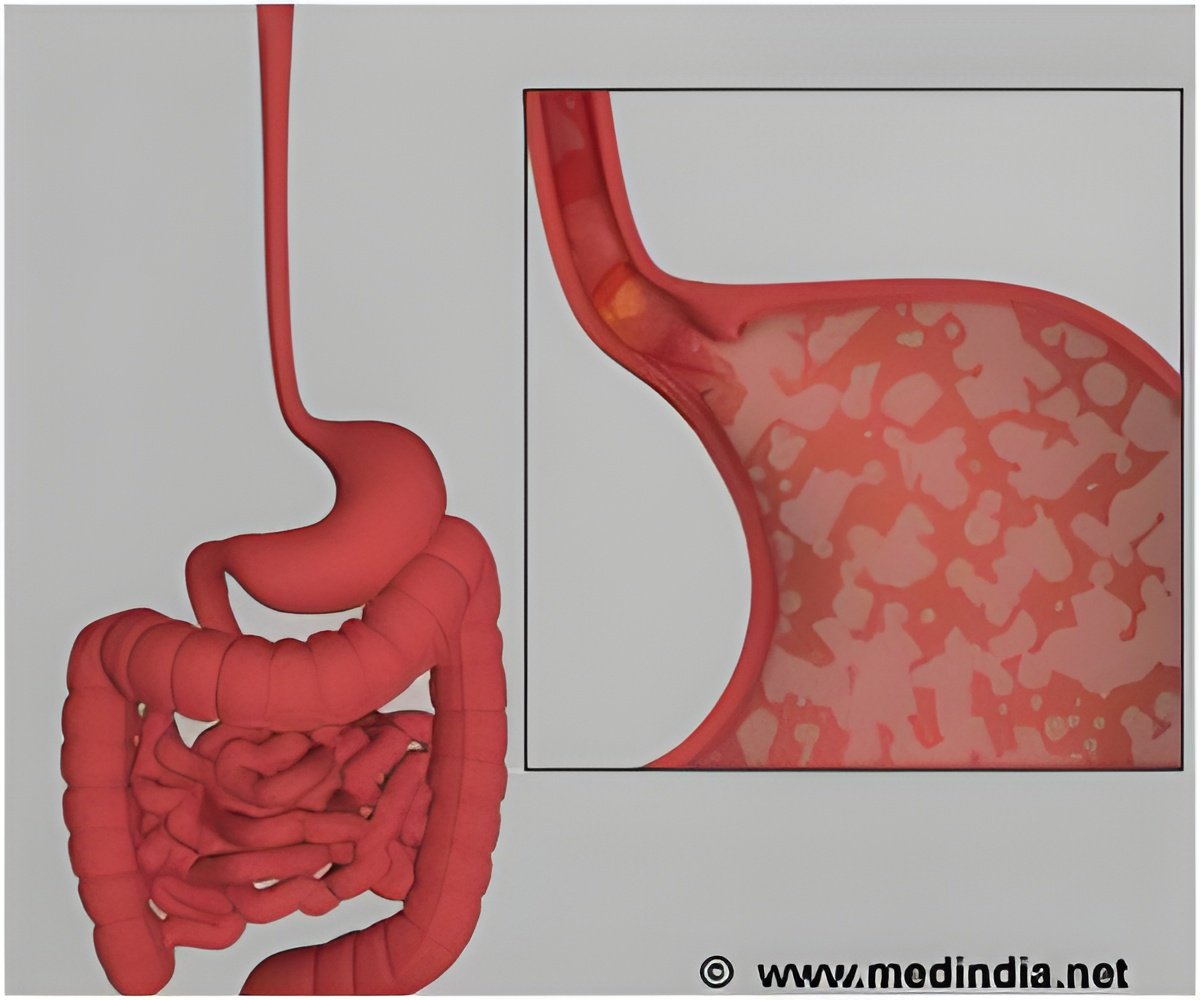
"The clinical problem addressed by this PIVI is the effectiveness and cost of current surveillance protocols, as well as rates of compliance with these protocols. Endoscopic surveillance of Barrett's esophagus (BE), as currently practiced, has shortcomings. Dysplasia (abnormal growth) and early adenocarcinoma may be endoscopically indistinguishable from non-dysplastic (benign) tissue. The distribution of dysplasia and cancer is highly variable, and even the most thorough biopsy surveillance program has the potential for a missed diagnosis due to sampling error. Current surveillance programs are expensive and time consuming," said PIVI Committee Co-Chair Prateek Sharma, MD. "Survey data indicate that while surveillance is widely practiced, there is marked variation from practice guidelines in the technique and interval of surveillance. A recent study found that adherence to guidelines occurred only 51 percent of the time and furthermore, the longer the length of the Barrett's segment, the worse the adherence."
The specific clinical issues addressed by this PIVI are what performance characteristics are required for an imaging technology to eliminate the need for random biopsies during endoscopic surveillance of patients with non-dysplastic Barrett's. The document outlines the following:
- Thresholds recommended for this PIVI
To eliminate the need for random mucosal biopsies during the endoscopic surveillance of patients with nondysplastic Barrett's esophagus, an imaging technology with targeted biopsies should have a per-patient sensitivity of 90 percent or greater and a negative predictive value (NPV) of 98 percent or greater for detecting high-grade dysplasia (HGD) or early esophageal adenocarcinoma (EAC) compared with the current standard protocol (white-light endoscopy and targeted and random 4-quadrant biopsies every 2 cm). In addition, the new imaging technology should have a specificity that is sufficiently high (80 percent) to allow a reduction in the number of biopsies (compared with random biopsies).
- Literature review summary
The most recent meta-analysis of cancer risk in Barrett's esophagus patients produced a pooled estimate of 0.6 percent per year. The majority of patients encountered in clinical practice are those without dysplasia. The operating characteristics of the various currently available imaging modalities for the diagnosis of HGD/cancer were determined by performing a systematic review. Overall, the NPV for current advanced imaging methods ranged from 79 percent to 100 percent, with a mean NPV of 97 percent. The per-patient sensitivity and specificity of new imaging techniques have ranged from 33 percent to 100 percent and 56 percent to 100 percent, respectively. The literature review also outlines the primary costs associated with surveillance.
- Areas for research
Having a better estimate of which patients are at greatest risk of developing esophageal cancer is important because screening and surveillance efforts should be focused more on these patients, with perhaps less frequent or no surveillance in those patients at relatively low risk. New imaging techniques would need to be compared with the "current standard" available endoscope, which could change in the future as the next generation endoscopes will continue to have improved imaging capabilities. Future studies will need to compare the new imaging technology with the standard 4-quadrant biopsy protocol in the same patient population to determine whether the PIVI thresholds are met. Additionally, cost-effectiveness studies will need to be performed related to the operating characteristics of any new imaging modality as compared to the standard biopsy protocol in the same population.Advertisement - Training issues/establishment of competency
Training needs to be available to ensure the effectiveness of any new technology as it becomes used in non-research settings. Quality measures would need to be developed to ensure consistent, high confidence examinations. Gastroenterological societies, such as ASGE, would develop position statements on minimum requirements for both trainees and practicing clinicians. Important tools for training would include educational materials, both in print and online, image libraries and hands-on workshops. There should be a way for individual practitioners to monitor their own accuracy as a performance quality measure (eg, prediction of neoplasia in lesions using white-light and/or enhanced imaging techniques, similar to detection of colonic adenomas).
- Other issues considered in establishing the thresholds
- Limitations of current methods for surveillance of patients with Barrett's esophagus
- Low risk of high-grade dysplasia/esophageal adenocarcinoma in patients with nondysplastic Barrett's esophagus
- Costs of standard endoscopy and biopsy