Further, their research demonstrated that aggressive reversal of psoriasis reduces the cardiovascular risk as well.
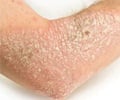
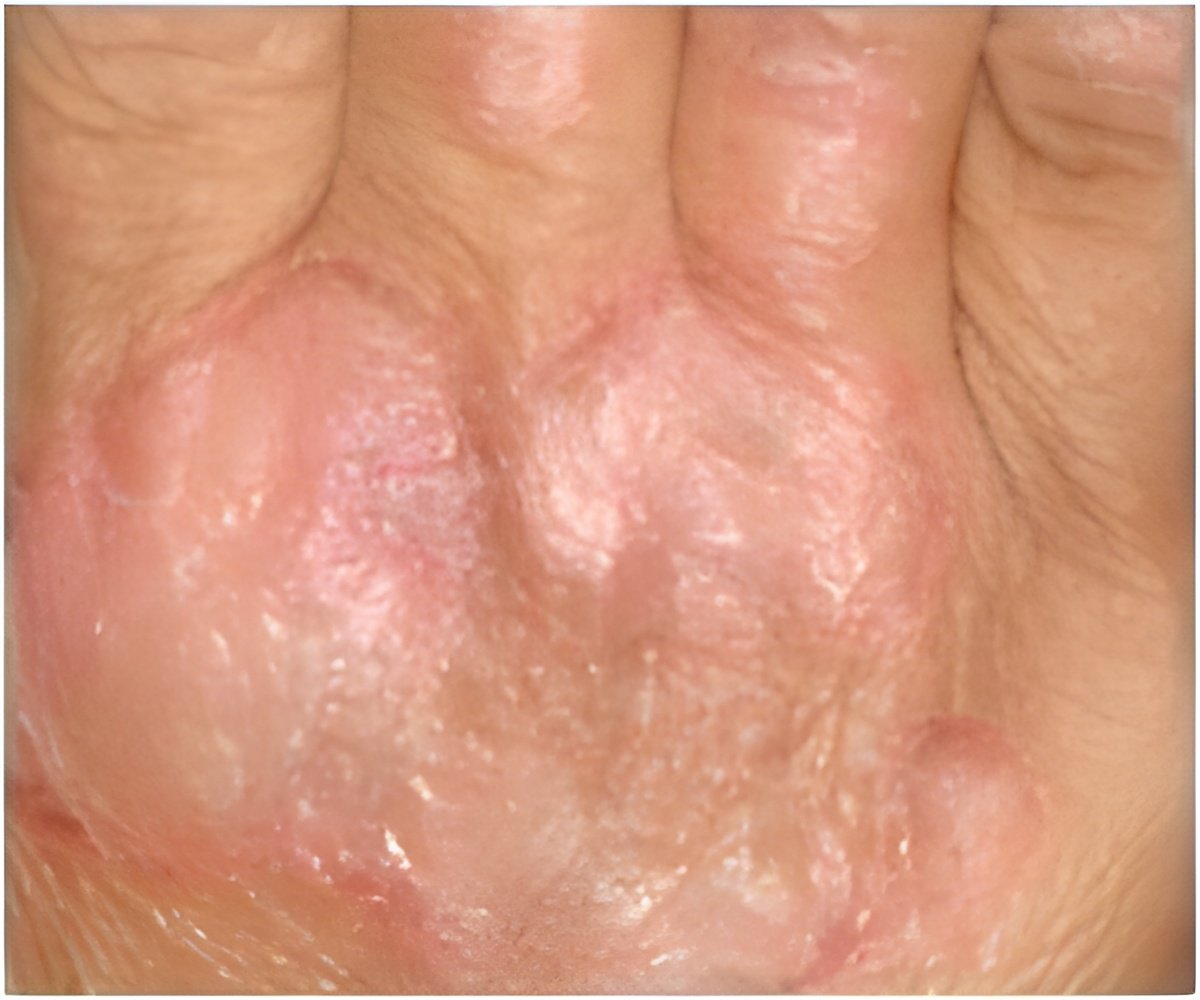
Psoriasis is a chronic disease of the immune system that appears as raised, inflamed, scaly red patches of skin and is often associated with intense itch.
The study used a new, innovative mouse model to demonstrate a causal connection between the skin disease and cardiovascular disease.
Nicole Ward, PhD, senior author of the study, and her team demonstrated that mice engineered to overexpress a protein called Tie-2 in the skin, develop a skin condition similar to human psoriasis. Using this model, they showed that persistent, chronic inflammation confined to the skin could result in inflammation in large arteries, such as the aorta.
"This discovery is paradigm shifting. There has been a link between the two diseases but to date we had not been able to show cause. Epidemiologic evidence from thousands of patients was convincing that psoriasis patients had a much greater chance of developing cardiovascular disease and dying from it," said Ward, PhD, assistant professor of dermatology and neurosciences at Case Western Reserve School of Medicine, and scientist with the Murdough Family Center for Psoriasis at University Hospitals Case Medical Center.
Advertisement
Many researchers showed, statistically, that having psoriasis leads to an increased risk for cardiovascular disease and heart complications, however it was unclear why this occurs and it was challenging to separate out the significance of other lifestyle factors and their contributions to this risk, she added.
Advertisement
They teamed up with experts in the role of inflammation in vessel injury - Yunmei Wang, PhD, assistant professor of medicine at the School of Medicine and Daniel I. Simon, MD the Herman K. Hellerstein Professor of Cardiovascular Research at the School of Medicine, and chief, Cardiovascular Medicine at University Hospitals Case Medical Center.
"We believed that chronic inflammation over a large area of the body may be the reason for an increased risk of cardiovascular complications in skin disease patients; however, until now we had no way to model and definitively prove this," said Dr. Wang.
Dr. Ward and her team measured blood clot formation in the psoriasis mouse model and normal mice, revealing that time was greatly shortened in the diseased mice. This shortened time to vessel blockage is akin to a greater risk for blood vessel blockage in humans that leads to stroke or heart attack.
Further examination revealed that mice with the skin disease also exhibited inflammation of the vessel wall similar to that observed with atherosclerotic lesions or plaques.
Importantly, and highly meaningful for patients with psoriasis, Dr. Ward's work was able to demonstrate that upon reversal of the skin disease, the cardiovascular inflammation and blood clot formation were also decreased.
"Our observations of improved vessel wall inflammation and decreased clot formation following skin-specific repression of disease provide further evidence that skin inflammation promotes vascular inflammation and thrombosis and strongly suggests that aggressive treatment of skin disease may block pathways that produce cardiovascular disease in psoriasis patients," said Dr. Ward.
The study was published in the Journal of Investigative Dermatology.
Source-ANI