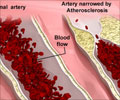
‘Obstructive Sleep Apnea is a prevalent chronic disorder. Although OSA is a common condition, it remains underdiagnosed in women.’
Read More..Tweet it Now
By contrast, in patients with cardiovascular disease, its prevalence can exceed 50% depending on the specific disorder surveyed. Although sex differences have been well described for cardiovascular risk factors; existing data regarding the impact of sex on the relationship between OSA and cardiovascular outcomes is controversial. Read More..
Similarly, while there is strong evidence for increased prevalence of cardiovascular conditions, such as systemic hypertension, atrial fibrillation, as well as heart failure amongst patients suffering from OSA; conflicting evidence exists regarding the incidence and bidirectional relationship between them as well as the impact of treatment of OSA on cardiovascular outcomes.
In this paper, the authors review the associations between OSA and cardiovascular diseases in women. The data on sex differences is limited, due to a number of reasons, including, but not limited to a late presentation of OSA in women, difficulties in diagnosing both OSA and cardiovascular diseases in women and still suboptimal inclusion of adequate number of women in clinical trials.
More studies are needed to better delineate sex differences in the clinical presentation as well as the pathophysiology of the associations between OSA and cardiovascular diseases so that we can provide patients with more personalized care.
This article forms part of a special issue on Women's Cardiovascular Health, guest edited by Gladys P. Velarde. Recent decades have witnessed great progress in the treatment of cardiovascular disease (CVD).
Advertisement
In the United States, CVD far outpaces all other causes of death, including all forms of cancer combined. The statistics are sobering with about one female death in the United States every 80 seconds from CVD. That represents close to 400,000 deaths per year according to the more recent statistics. Of these, more than one-quarter of a million women will die this year from ischemic heart disease (IHD) which includes obstructive and non-obstructive coronary disease, and about 64% of women who die suddenly of IHD have no prior symptoms.
Advertisement
This lack of awareness is more profound (over 60% unaware) among women in higher-risk groups, racial and ethnic minorities, and has changed little in decades.
Poorly understood sex/gender differences in pathobiologic mechanisms, clinical presentation, management and application of diagnostic and therapeutic and preventive strategies have contributed to this gap. A critically important factor has been the underrepresentation of women in CVD research to date. In fact, only one-third of CVD clinical trials report sex-specific results despite The Food and Drug Administration regulations requiring sex stratification data, as well as the National Institute of Health recommendations of increased inclusion of women in clinical trials.
This makes it difficult for researchers and clinicians to draw accurate conclusions about sex differences in mechanisms of disease, accuracy of specific diagnostic modalities and risks or benefits of a particular drug or device for the treatment of women with CVD.
Furthermore, physicians and other healthcare providers continue to underestimate women's cardiovascular risk, in part because of utilization of traditional approaches which can lead to over-testing or inappropriate risk assessment without accurate differentiating who is truly at risk and inadequate use of preventive therapies for women.
The goal of this special edition Cardiovascular Innovations and Applications is to shed some light on specific topics that dominate the spectrum of CVD in women.
Source-Eurekalert