Within six months the patient self-assessment arm showed 89% of patients completed self-assessment and calculated their Disease Activity Score (DAS). The results were shared with their treating rheumatologist, which resulted in 17.2% changing their drug therapy (p=0.0012).1 Regular assessment of disease activity enables measurement of disease status over time (e.g. flares); while unfeasible in the clinic these data show that it can be undertaken by nurses and patients.
RA patients are at increased risk of associated diseases such as cardiovascular disease (CVD) or infections. In the arm where a nurse-led programme assessed potential co-morbidities and risk factors, at 6 months the number of actions taken to reduce co-morbidities, per patient, was significantly higher (p<0.001).2 The action taken into account varied depending on the co-morbidity, for example patients with CVD might have had lipid-lowering or anti-platelet therapies introduced, whereas those with an infection risk may have been vaccinated.
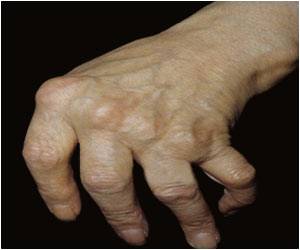
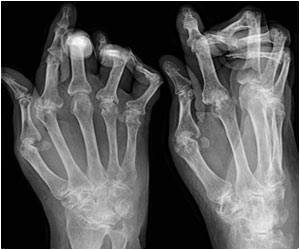
RA is a chronic autoimmune disease that principally attacks flexible joints. Affecting approximately 1 in 100 people worldwide, RA can cause pain, stiffness, progressive joint destruction and also reduce physical function, quality of life and life expectancy. In addition, RA is associated with a number of co-morbidities, including cardiovascular disease, cancer, lung disease, gastrointestinal disorders and infection.3
Prof. Maxime Dougados, Professor of Rheumatology at René Descartes University, Chief of Rheumatology at Cochin Hospital, Paris, France, and a principal investigator on the study said, "Treat to Target* and EULAR recommendations suggest that we should be promoting self-management skills so that patients can regularly assess their own disease activity. Nurses can participate in this teaching. Looking at this data the positive impact of a nurse-led programme is clear; not only did the majority of patients participate in self-assessment, but within just six months the assessments resulted in many patients actually changing treatment."
Commenting on the impact of nurse intervention on comorbidities, Dr. Gossec, Associate Professor of Rheumatology in Paris 6 University and Pitie-Salpetriere Hospital, Paris, France, said "Patients with RA are at an increased risk of developing a number of co-morbid conditions which have a major influence on both mortality and disease outcome. During this trial, the number of actions undertaken to prevent these co-morbidities was significantly greater in the arm where nurses had thoroughly assessed the risks, with particular improvements observed against cardiovascular disease, infections, cancer and osteoporosis."
Advertisement
"These data demonstrate that in the short term, nurse-led interventions can equip patients with the tools required to more effectively manage their disease. Longer-term patient follow up is required to investigate the sustainability of these benefits, but these data have the potential to significantly alter the management of RA," concluded Prof. Dougados.
Advertisement
Source-Eurekalert