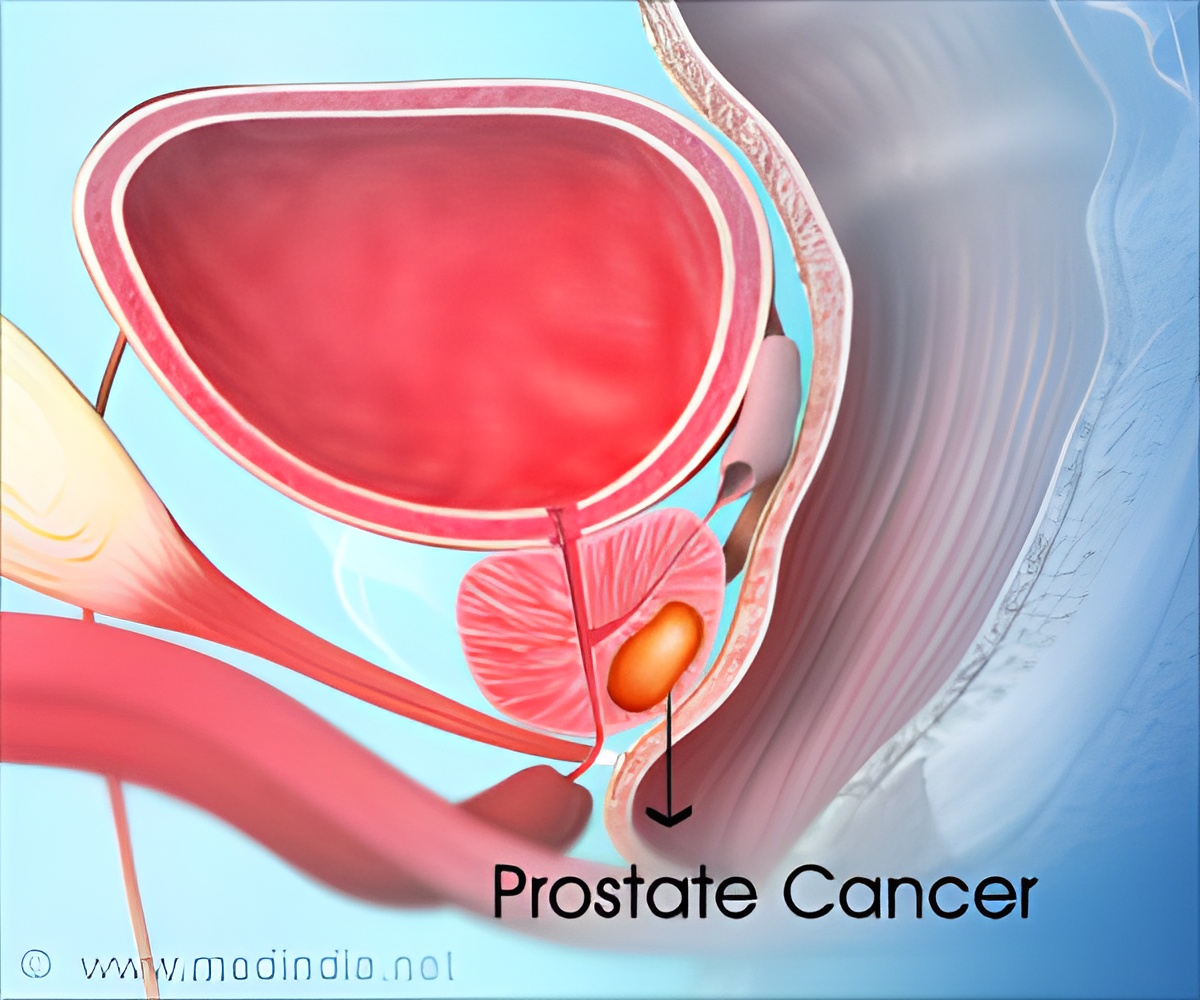
‘Using a novel imaging agent, researchers were able to detect the prostate cancer cells that have metastasized to bone - one of the most difficult areas to evaluate using standard methods.’
Tweet it Now
"This agent is imaged faster than other PSMA-targeting imaging
antibodies due to its small size and has been shown to be safe for
patients," explains Neeta Pandit-Taskar of the Memorial Sloan
Kettering Cancer Center in New York City. "The radiotracer combines a
small amount of the radioactive material zirconium-89 with a fragment of
an antibody called a minibody. This minibody has anti-PSMA qualities
and attaches to overexpression of the enzyme on the exterior of prostate
cancer cells, wherever they may have traveled in the body. Particles
emitted from the site are then detected by positron emission tomography
(PET). The resulting scan highlights 'hot spots' of PSMA
overexpression." She adds, "Using this agent, we can detect the prostate cancer cells that have metastasized to bone - one of the most difficult areas to evaluate using standard methods."
For the study, 18 patients were imaged with the new agent using PET/CT as well as a variety of conventional imaging modalities, including computed tomography (CT), magnetic resonance imaging (MRI), molecular bone scan (SI), and PET with fluorodeoxyglucose (FDG-PET). Suspected disease sites were then selected and biopsied.
Both skeletal and nodal lesions were detected with Zr-89-Df-IAB2M; scans were positive in 17 of the 18 patients, with bone lesions targeted in nine and soft tissue disease seen in 14. In comparison, bone scans with more traditional agents (Tc-99m-methylene diphosphonate and FDG) were positive for bone lesions in nine and six patients, respectively; for nodal/soft tissue disease, CT and FDG scans were positive in 14 and 10 patients, respectively. In two patients, a single site of disease per patient was identified only by the minibody. In total, Zr-89-Df-IAB2M imaging detected 147 bone and 82 soft-tissue or nodal lesions.
"Results of imaging with this Zr-89 radiolabeled minibody have shown that we are able to detect more disease sites in patients than with conventional imaging," Pandit-Taskar states. "We hope that with further development this technology will help us in earlier and more accurate assessment of disease and assist in clinical decision-making." She points out, "With further validation, this agent could potentially be used for targeted biopsies, which could lead to more appropriate, timely treatment for prostate cancer patients. It may also have potential use in targeted radiotherapy."
Advertisement



![Prostate Specific Antigen [PSA] & Prostate Cancer Diagnosis Prostate Specific Antigen [PSA] & Prostate Cancer Diagnosis](https://www.medindia.net/images/common/patientinfo/120_100/prostate-specific-antigen.jpg)