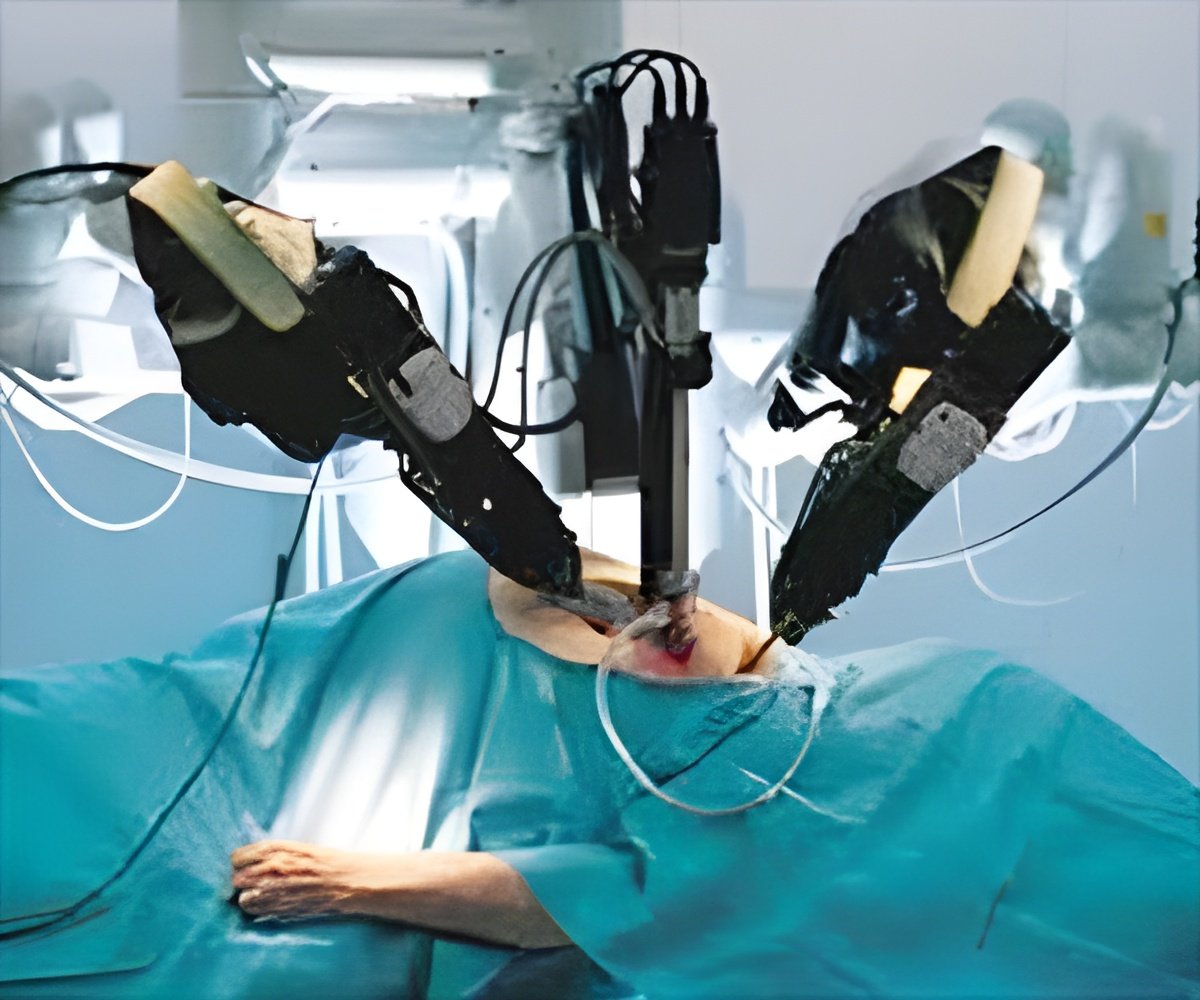
‘A newly developed robot can indeed adjust to the subtle movement and deformation of soft tissue to execute precise and consistent suturing.’
Tweet it Now
Simon Leonard, a Johns Hopkins University computer scientist, is part of a team that has just published research showing that a robot surgeon can indeed adjust to the subtle movement and deformation of soft tissue to execute precise and consistent suturing. The research, which appears in the journal Science Translational Medicine, promises to improve results for patients and make the best surgical techniques more widely available. Leonard, an assistant research professor in the university's Whiting School of Engineering, worked with five co-authors, all affiliated with Children's National Health System in Washington, D.C.: Azad Shademan, Justin D. Opfermann, Peter C.W. Kim, Johns Hopkins alumnus Axel Krieger, and Ryan S. Decker.
"There's a wide range of skills out there among surgeons," said Leonard, who worked for four years to program the robotic arm to precisely stitch together pieces of soft tissue. "Putting a robot to work in this form of surgery really levels the playing field."
The published results involved suturing two structures. The procedure called anastomosis, meaning joining two tubular structures such as blood vessels, is performed over a million times a year in the United States. According to the researchers, complications such as leakage along the seams occur nearly 20% of the time in colorectal surgery and 25-30% of the time in abdominal surgery.
"Robotic soft tissue surgery," the researchers wrote, "promises substantial benefits through improved safety from reduction of human errors and increased efficiency due to procedure time reduction." This surgery, however, can present a challenge in that it can be tricky for a robot to adjust to the soft tissue's slips and squirms during suturing.
Advertisement
The STAR robotic sutures were compared with the work of five surgeons completing the same procedure using three methods: open, laparoscopic and robot-assisted surgery. Researchers compared consistency of suture spacing, pressure at which the seam leaked, mistakes that required removing the needle from the tissue or restarting the robot, and completion time.
Advertisement
"No significant differences in erroneous needle placement were noted among all surgical techniques," the researchers wrote, "suggesting that STAR was as dexterous as expert surgeons in needle placement."
It's not clear when the robotic system will be in use in operating rooms, but the researchers wrote that the intent is not to replace surgeons, but to "expand human capacity and capability."
As Leonard put it, they're designing an advanced surgical tool, "the equivalent of a fancy sewing machine."
Source-Eurekalert