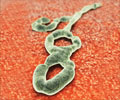
Scientists said Friday an outbreak of Ebola that killed 37 people in Uganda last year was sparked by a hitherto unknown species of one of the world's most notorious viruses.
The strain, provisionally named Bundibugyo ebolavirus after the district where the outbreak occurred, joins four other known species of the pathogen, they said.More than one in three of patients infected with Bundibugyo died, according to their study, appearing in the US journal PLoS Pathogens, published online by the open-access Public Library of Science (PLoS).
Ebola and the Marburg virus are the two main categories of so-called filovirus which causes haemorrhagic fever (VHF), a disease dubbed a "slate-wiper" for its extreme lethality.
The early signs of VHF are usually a high temperature, exhaustion, dizziness, watery diarrhoea and muscle ache. These symptoms are often mistaken for other fevers, such as flu or yellow fever, because VHF is rare.
As the virus spreads, the feverish patient often starts to bleed under the skin and in severe cases, from the mouth, ears and eyes.
Blood loss, shock and organ failure lead to coma and delirium and, in many cases, to death, within three to seven days after onset of symptoms.
Advertisement
Approximately 1,850 cases with over 1,200 deaths have been documented since the virus was discovered, according to the World Health Organisation (WHO).
Advertisement
The least harmful are the Cote d'Ivoire ebolavirus, which was discovered in the Ivory Coast in 1994 and so far has caused only a single, non-fatal case of VHF; and the Reston ebolavirus, identified at a US research facility in 1989, which spread from imported lab monkeys to at least four people, none of whom fell sick.
The newly-discovered species came to light after VHF erupted in the townships of Bundibugyo and Kikyo in November 2007, says the study, authored by US and Ugandan doctors.
The US Centers for Disease Control and Prevention (CDC) tested 29 blood samples, which were negative to high-sensitivity tests tailored to the three known strains of Ebola virus. But the samples tested positive in an older, broad-spectrum antibody assay.
Intrigued, investigators pulled apart the pathogen's genetic code to see what they had snared.
Using ultra-fast sequencing technology, they decoded the virus' genome in a matter of days, finding a variation of 32 percent compared with the three existing strains.
Of the 149 suspected cases of Bundibugyo ebolavirus, 37 were fatal, translating into a mortality rate of 36 percent.
The wide genetic divergence between the strains has major implications, the authors say.
It will require the invention of new diagnostic tools to detect outbreaks and could complicate the quest for vaccines and treatments.
US scientists working in a Pentagon-backed programme successfully tested a vaccine among monkeys in 2005 and 2006, but trialling this formula on humans remains a distant goal.
In the absence of a shield or a cure, the only solution is the time-honoured method of isolating the patient, providing barrier protection (rubber gloves, gowns and goggles) for health workers and rigidly observing hygiene procedures.
Ebola is also lethal for non-human primates, killing thousands of gorillas and chimps in recent years and endangering those who butcher or handle their meat.
The natural reservoir for the Zaire ebolavirus has been found in three species of fruitbat in the rainforests of central and western Africa. The wildlife host for the three other strains is unknown.
Source-AFP
SRM