He added: "Preventing these symptoms and complications requires bringing the patient out of AF and back to the normal sinus rhythm. The quickest way to do that is to deliver an electric shock. The shock depolarises and synchronises the heart muscle and allows the sinus node to re-establish a normal rhythm."
Dr Bingen continued: "Shocks are currently the most effective way to get patients directly back into sinus rhythm but they are very painful. To deliver a shock you have to give anaesthesia which comes with its own possible adverse effects."
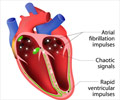
AF usually progresses from a paroxysmal form, in which episodes of AF last from several minutes up to 7 days, to a persistent and eventually a chronic form. People with the latter are in AF 24 hours a day, 7 days a week, and shock treatment no longer works. Dr Bingen said: "AF causes structural changes to the atrium which make patients more prone to subsequent induction of AF. That's another reason to get patients back into sinus rhythm as soon as possible."
For the current study, the researchers devised a method of shockless defibrillation. They used optogenetics to genetically insert depolarising ion channels into the heart that can be activated by light. Dr Bingen said: "The theory was that we could just turn a light switch on and depolarise the entire myocardium without needing a shock. In theory, the patient could be given an implantable device with a mesh of light emitting diodes (LEDs) and when AF occurs you turn the light on and the AF stops."
During arrhythmias there is activity subepicardially but the heart is a complex 3D structure and it is only possible to directly observe the epicardium (outside layer). To see how their method worked subepicardially, the researchers developed 2D hearts. They isolated cardiac muscle cells from the rat atrium, replated them in a culture dish and allowed the cells to form intercellular connections, creating a 2D heart.
Advertisement
Dr Bingen said: "Then it was just a matter of switching on the light and seeing what happened. We found that in all 31 of these 2D hearts we were able to achieve the 2D equivalent of cardioversion into sinus rhythm. The mechanism we saw was a bit different than the normal defibrillation but was equally effective."
Advertisement
Dr Bingen continued: "This is the first evidence of a shockless defibrillation. Our method of using optogenetics to defibrillate by light is completely painless and looks promising but more research is needed before it can be applied in patients."
Source-Eurekalert