The January issue of Behavioural Neurology, edited by the journal's co-Editor in Chief, Argye E. Hillis, MD, of the Departments of Neurology, Physical Medicine and Rehabilitation, and Department of Cognitive Science, Johns Hopkins University, Baltimore, Maryland, features papers on two topics that have traditionally captured the interest of behavioral neurologists – aphasia and hemispatial neglect.
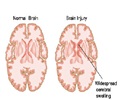
The first section on aphasia includes a number of papers that compare post-stroke aphasia with primary progressive aphasia (PPA), in which the predominant deficit is language (with or without apraxia).
Andreia V. Faria, MD, Department of Radiology, Johns Hopkins University School of Medicine, and colleagues from Johns Hopkins and University College, London, report patterns of dysgraphia (spelling impairment) in participants with primary progressive aphasia, and compare these patterns to those in participants with dysgraphia following stroke. They also report the areas of focal atrophy associated with the most common pattern of dysgraphia in PPA and suggest this can not only provide a better understanding of the neural substrates of spelling, but may also provide clues to more effective treatment approaches.
Matthew A. Lambon Ralph, FRSLT (hons), FBPsS, and colleagues from the School of Psychological Sciences, University of Manchester, UK; the Department of Psychology, University of York, UK; and the Stroke and Dementia Research Centre, St George's University of London, UK, use a novel approach to explore nonverbal semantic processing to demonstrate the qualitative differences between semantic aphasia and semantic dementia. Their conclusions provide further support for the proposal that semantic cognition is underpinned by two principle components: semantic representations and regulatory control processes which regulate and shape activation within the semantic system.
Cynthia K. Thompson, PhD, and colleagues from the Department of Communication Sciences and Disorders, Department of Neurology, Cognitive Neurology and Alzheimer's Disease Center, and Department of Psychiatry and Behavioral Sciences at Northwestern University, Evanston, Illinois, evaluate the distinct patterns of morphological and syntactic errors in the variants of PPA, and compare them with patterns of errors in post-stroke aphasia.
Advertisement
"Together, these papers illustrate how investigating PPA and post-stroke aphasia can yield complementary insights about brain-behavior relationships as well as about potential response to interventions and the normal cognitive processes underlying language," says Dr Hillis.
Advertisement
"Hemispatial neglect remains one of the most remarkable syndromes investigated by behavioral neurologists," comments Dr Hillis. "These novel studies of neglect and related disorders provide new insights into brain-behavior relationships on the basis of detailed analysis of patient performance – and in many cases, their lesion sites."
Source-Eurekalert