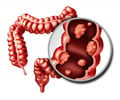
The U.S. Multisociety Task Force — comprised of representatives of the American College of Gastroenterology, the American Gastroenterological Association and the American Society for Gastrointestinal Endoscopy — evaluated the guidelines for colorectal cancer surveillance published in 2006 to determine if they should be updated based on new evidence.
"The U.S. Multisociety Task Force believes that the evidence supporting current recommendations for screening and surveillance intervals has become stronger in the past six years," said David Lieberman, MD, lead author of the guidelines. "While these guidelines are dynamic and will continue be revised in the future as new evidence emerges, we believe the guidelines represent the best science available for the screening, surveillance and prevention of colorectal cancer."
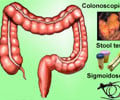
The task force recommends that all endoscopists monitor key quality indicators as part of a colonoscopy screening and surveillance program. The following colonoscopy schedule is recommended following a patient's initial high-quality exam:
| Initial exam finds no polyps or small (< 10 mm) hyperplastic polyps in the rectum or sigmoid colon | Next colonoscopy in 10 years |
| Initial exam finds low-risk adenomas defined as 1-2 tubular adenomas <10mm | Next colonoscopy in 5-10 years |
| Initial exam finds benign, but high-risk neoplastic polyps Includes: adenoma >=10mm, or with villous histology, high grade dysplasia; three or more adenomas; sessile serrated lesions which are dysplastic and/or >=10mm | Next colonoscopy in 3 years |
The guidelines also provide advice on murky areas related to colorectal cancer screening:
Advertisement
- When should colonoscopy be repeated if the patient's bowel isn't properly prepared for colonoscopy? In most cases, repeat the exam within one year. Note that splitting the dose of bowel preparation yields better results.
- Should stool tests (guaiac fecal occult blood test or fecal immunochemical test) be used in between colonoscopies to check for cancer? Fecal testing between colonoscopies isn't necessary within five years of colonoscopy.
- Aspirin and non-steroidal anti-inflammatory drugs may reduce risk of polyps — should screening intervals change for patients on these medications? There is insufficient evidence to recommend any change.
- If new symptoms develop, should a patient receive a colonoscopy earlier than scheduled based on guidelines? The likelihood of finding significant pathology after a complete and adequate colonoscopy is uncertain, but likely to be low. However, if the colonoscopy will answer an important clinical question, it may be valuable to repeat.
- Should surveillance be modified based on patient race, ethnicity or gender? If patients have had a high-quality colonoscopy, there's no reason to alter the surveillance interval based on these factors.
- At what age should colorectal cancer surveillance stop? The decision to continue colonoscopy in the elderly should be individualized based on an assessment of benefit, risk and other medical conditions.
Source-Eurekalert