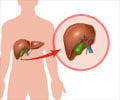
Morbidity following liver transplant is highest among obese patients with diabetes, researchers from New Zealand reveal.
One of the greatest health concerns in developed countries is the increase in obesity, diabetes, and metabolic syndrome, which is a combination of high blood pressure (hypertension), blood sugar (hyperglycaemia), and cholesterol (dyslipidemia) along with increased belly fat. In fact, the World Health Organization (WHO) reported in 2008 that 1.4 billion adults were overweight, and of these 200 million men and 300 million women were obese.
Prior research shows that liver transplant recipients who develop post-transplant diabetes and metabolic syndrome are at increased risk of cardiovascular disease. Moreover, while death and graft loss resulting from organ rejection has improved in past 30 years, up to 42% of non-graft related deaths are attributed to cardiovascular disease according to a 2002 study by Vogt et al.
"There is much evidence on post-transplant obesity and metabolic syndrome. However, the impact of pre-transplant obesity, hypertension and coronary artery disease on post-transplant outcomes has received less attention and is the focus of our study." said lead author Dr. Adam Bartlett with the New Zealand Liver Transplant Unit at Auckland City Hospital.
For the present study, researchers recruited 202 consecutive patients undergoing liver transplantation at a New Zealand center between 2000 and 2010. BMI and percentage of body fat were measured before the transplant to compare methods. Analyses of pre-transplant risk factors such as obesity, diabetes, coronary artery disease were conducted.
Participants undergoing liver transplant had a mean age of 51 years and 67% were male with most common reason for being hepatitis C cirrhosis. The BMI was available for 192 patients—4% were underweight, 27% normal weight, 26% overweight, 28% obese, 9% severely obese and 6% morbidly obese. Researchers determined that BMI and measured body fat were similar in 86% of the study group.
Advertisement
"Our study confirms that BMI is an appropriate measure of body fat and obesity alone should not prevent patients from receiving liver transplants," concludes Dr. Bartlett. "Identifying modifiable risk factors during the pre-transplant assessment allows for earlier interventions including weight control, diabetes management, and coronary interventions such as stenting, all which may improve long-term outcomes following liver transplantation."
Advertisement
Source-Eurekalert